The Anesthesia Patient Safety Foundation (APSF) has awarded nearly $12 million in funding for anesthesia patient safety research projects over its 30-year history. There were very few funding opportunities for patient safety research in any specialty, let alone anesthesia, when the research program began in 1985.1 The term “patient safety” was relatively new, with the specialty of anesthesiology recognized as a health care leader in the adoption of patient safety as an explicit goal of patient care. APSF became the first foundation dedicated solely to patient safety. One of the most important goals of the APSF was to promote research to improve anesthesia patient safety, and the organization devoted significant monetary resources in support of that goal. The first research grants were awarded in 1986.1 In the early years, small grants of $35,000 were awarded ($74,000 in 2017 dollars adjusted for inflation). The maximum award increased over the years to both keep up with inflation as well as to expand the scope of the projects. Increases in the maximum award amount in 1997 kept up with inflation, while the increase in 2000 went beyond inflation to a maximum of $65,000 in 2000 ($92,000 in 2017 dollars). A major increase in award amounts in 2007 resulted in the current award limit of $150,000, double the initial award amount (adjusted for inflation) from the inception of the program 30 years ago.
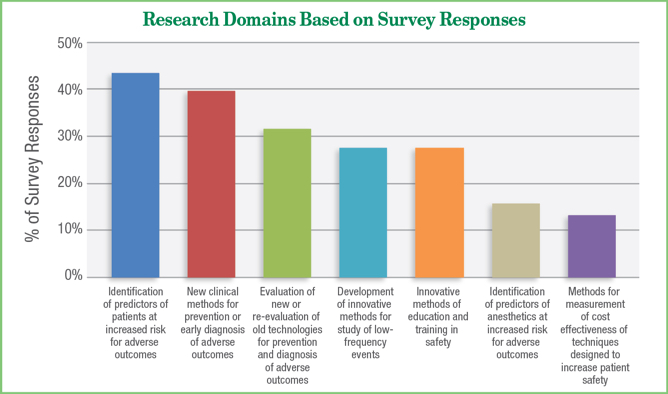
Figure 1: Research domains based on survey responses. Note that some respondents indicated more than 1 category. “Other” = 12% of responses
In addition to changes in the maximum allowable budget per grant, APSF has increased the total number of awards in years when sufficient organizational funds were available. Funding for anesthesia patient safety research has now expanded from strictly APSF funds to grant awards sponsored by the American Society of Anesthesiologists (ASA), industry, and other donations. The 2017 funding cycle included awards sponsored by the ASA (APSF/ASA President’s Research Award and Endowed Research Award), industry (APSF/Medtronic Research Award), and donations (APSF Ellison C. Pierce, Jr., MD, Merit Award).
The program has also expanded over time from solely scientific research projects to encompass educational research and curriculum development. Special requests for proposals (RFPs) targeting selected areas of interest are periodically solicited, as are Safety Scientist Career Development Awards to promote career development in anesthesia patient safety research. Annual funding amounts for all projects over the years (in 2017 dollars) ranged from $145,000 to >$1,200,000, with an average total of $400,000 per year over the APSF grant program’s 30-year history.
APSF has reviewed the progress and impact of its grant program at various intervals.1,2 In the spring of 2017, the APSF conducted a survey of past and current research grant and Safety Scientist Career Development Award recipients going back to 1986 when the first grant was awarded. The survey was emailed to all living principal investigators (PIs) whose contact information was available—a total of 113 individuals representing 118 awards.
The goal of the survey was to evaluate and further promote the effectiveness of the APSF Research Program. A total of 76 responses from 71 different PIs (some individuals had received funding more than once) were received and analyzed. The results are described in the following sections.
APSF Grant Program 2017 Survey Results
Types of Grants Awarded
The grants covered a variety of research topics related to patient safety (Figure 1) and a number of grants addressed more than one patient safety domain. As reported by the respondents, the most common domains included identification of predictors of patients at increased risk for adverse outcomes (43.4%), new clinical methods for prevention or early diagnosis of adverse outcomes (39.5%), evaluation of new or re-evaluation of existing technologies for prevention and diagnosis of adverse outcomes (31.6%), development of innovative methods for the study of low-frequency events (27.6%), innovative methods of education and training in patient safety (27.6%), and methods for measurements of cost-effectiveness of technologies designed to increase patient safety (13.2%).
Survey responses also indicated specific study categories (Figure 2). Top categories were human factors or human performance (43.4%), outcomes or incident measurement (40.8%), risk assessment or risk factors (34.2%), monitoring and injury prevention (30.3%), prevention of specific complication or injury (30.3%), and education or training (29%).
Study methodologies varied, most frequently representing clinical trials (34.2%), simulation or computer modeling (30.3%), non-clinical human subject studies (26.3%), database analysis (18.4%), and medical records review (13.2%) as shown in Figure 3.
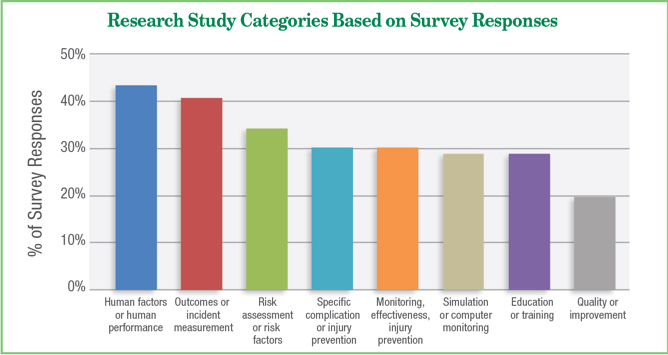
Figure 2: Research study categories based on survey responses. Note that some respondents indicated more than 1 category. Only top 8 responses are included in this figure.
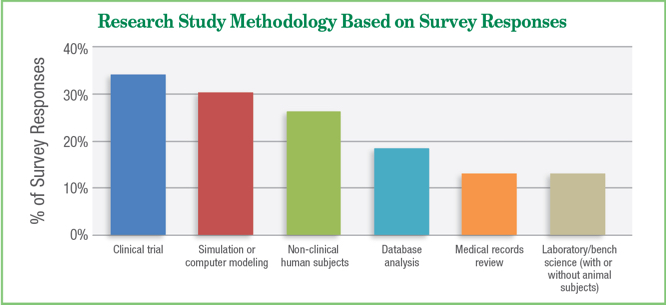
Figure 3: Research study methodology type based on survey responses. Note that some respondents indicated more than 1 category. “Other” = 14% of responses
Grant Results and Impact on Anesthesia Patient Safety
When asked about major findings of the project and associated changes to anesthesia practice, education, or public policy, investigators reported a wide range of impact on patient care. Many APSF-funded projects have led to direct improvements in patient safety. Earlier projects supported human factors research, crisis management and simulation, checklists, device development, and patient monitoring and alarm generation. One project used human factors techniques for measuring intraoperative vigilance by embedding vigilance probes in the workplace. Another research grant aided in funding a study that applied cognitive analysis techniques to investigate how clinicians think about respiratory function and what the cognitive challenges are for assessing patient ventilation status. The analysis was then used to map the demands of ventilation-related events and the effectiveness of medical equipment in supporting clinical decision-making.
Several simulation-based projects have been funded by the APSF. These projects addressed issues such as improving technical performance skills, team dynamics and crisis resource management, facilitated simulation use in educational assessment, and health systems integration. APSF has also funded a number of education-related grants, including an examination of the impact of long work hours on performance and on the learning of anesthesia providers. Other education-oriented studies created a web-based program for ultrasound training and validated methods for assessing performance of first-year anesthesia residents to ensure minimum levels of competency. This latter project developed simulation-based assessment metrics to identify anesthesia residents who may not have attained sufficient skills expected for their stage of training. Another grant was used to design and build an adjustable airway task trainer able to assume numerous anatomic configurations and to model four laryngoscopic views using combinations of unfavorable airway factors. This model subsequently has been used in multiple research projects, supported several publications and grants, and proved useful in resident training.3
Other important perioperative safety topics supported by APSF funding have included an investigation of postoperative delirium and cognitive dysfunction after cardiac and noncardiac surgery, such as the effects of surgery and anesthesia on postoperative cognitive dysfunction and the onset and progression of Alzheimer’s disease; the effects of perioperative hypothermia on bleeding and wound infection; novel approaches to difficult airway recognition and management; and identification of the incidence and risk factors associated with perioperative vision loss.
APSF-funded projects continue to address a wide variety of important perioperative safety issues and stimulate broad areas of continued research. Recent examples include opioid safety in children and adults, better ways of risk assessment and monitoring for postoperative respiratory depression, as well as strategies for improving perioperative outcomes through preoperative evaluation including frailty, nutritional status, obstructive sleep apnea, and cognitive status. Techniques to improve communications in emergent situations have been studied and implemented, including studies on the effectiveness of emergency manuals and other decision aids, handoffs, and transitions in critical care. Given the increasing importance of big data in outcomes research, APSF funding has recently enabled one investigator to integrate several distinctly different patient databases that existed at one institution and to pursue large-scale epidemiologic studies of perioperative outcomes. Investigators have used intraoperative physiologic markers such as heart rate variability and vasoactive drug use patterns to identify risk factors for postoperative deterioration. Another recent grant provided the initial funding to develop a collaborative implementation research program within a large network of hospitals. This program integrated information systems to disseminate evidence-based practice and answer research questions to which multisite big data resources are uniquely suited.
Grant Program Impact on Patient Safety Research
In addition to exploring the direct impact of APSF grants on improving patient safety, the survey also inquired about the role the grant program had on an individual’s career in patient safety. Overall, the respondents praised the program as helpful to both beginners and established researchers. Many described unique opportunities afforded by the grants to receive mentorship as well as to mentor others.
APSF grants have contributed to developing patient safety research expertise beyond the principal investigator. For example, one respondent commented that, in addition to studying an important clinical question, APSF funding “allowed the support of junior faculty who gained academic experience and publications. All have progressed in their careers and continue as investigators.” APSF funding has also helped many investigators establish collaborations with colleagues nationally and internationally, maintain an academic career, and engage in projects for which there otherwise would be no or limited funding available. According to another respondent, “APSF funding not only made the work possible, but it validated the notion of patient safety research (i.e., simulation, decision-making, cognitive aids, etc.) as an appropriate line of academic endeavor.” There are even instances where the funding allowed the investigator to initiate a completely new and innovative line of research and move beyond basic science to translational research involving human subjects.
Having dedicated, protected time from clinical duties is often necessary for pursuing an academic career. APSF funding has helped secure academic time for the vast majority of investigators and this time has been instrumental in getting their projects completed and advancing their careers in patient safety. The ability to do research is becoming much more difficult in the current academic environment where clinical productivity has become the priority of many institutions. One respondent commented that, “As research faculty are becoming a smaller fraction of our academic population in anesthesia…these grants are becoming increasingly more important to the survival of our academic missions.” As many as 86% of prior recipients who responded to the survey are still actively involved in patient safety research and other similar activities not directly related to clinical work.
One important metric of any research grant program is whether it has led to additional extramural funding for the investigator. For many respondents, initial APSF grant support contributed to additional peer-reviewed funding. Approximately 68% of applicants conducted additional related studies following up on their APSF grant activities. The National Institutes of Health (NIH), Agency for Healthcare Research and Quality (AHRQ), Patient-Centered Outcomes Research Institute (PCORI), other government organizations such as NASA and the Veterans Administration, nonprofit foundations, professional societies, and industry have served as additional funding resources. Overall, APSF funding has resulted in a significant “return on investment” as evidenced not only by follow-up funding successes, but also by development of patient safety careers, high-impact peer-reviewed publications, and clinical practice improvements adopted by our specialty to improve patient safety.
Future Directions
The APSF leadership is using the information obtained from this survey to gain perspective on the successes of this long-standing grant program and to address unmet needs with future awards aiming to further advance perioperative patient safety.
The importance of mentorship was a significant theme in many of the responses as a major factor in successful completion of projects and subsequent successes of grant recipients as patient safety researchers. Thus, the APSF is reviewing opportunities to bring prior grant recipients together and create a network of patient safety leaders, mentors, and educators. In the survey, we proposed an idea for creating an Anesthesia Patient Safety Leaders Alumni Network (APSLAN)—an active community of prior and current grant recipients to promote stronger engagement with APSF and across the specialty. Specifically, a network such as APSLAN holds the potential to stimulate and promote future patient safety initiatives and create a formal mechanism for mentoring a new generation of patient safety researchers. An overwhelming number of respondents (~ 80%) expressed interest in participating. More information about this important initiative will be forthcoming.
In summary, during its 30-year existence the APSF grant program has funded many successful research projects that have produced significant improvement in perioperative patient safety. The grant program has also helped to nurture the careers of patient safety scientists by helping them to develop qualitative, clinical, and educational research skills. APSF funding has provided the support needed by a majority of grant recipients to successfully pursue additional large patient-safety-oriented awards from federal agencies, foundations, and industry. Our survey results show significant overall satisfaction with the program and the desire by many prior recipients to stay engaged with APSF to help shape the future of perioperative patient safety research. The APSF is grateful to its individual and practice donors, corporations, and anesthesia organizations for their continued support.
Dr. Richard Urman is Associate Professor of Anaesthesia at Harvard Medical School and is in the Department of Anesthesiology at Brigham and Women’s Hospital, Boston, MA.
Dr. Karen Posner is the Research Professor and Laura Cheney Professor in Patient Safety in the Department of Anesthesiology & Pain Medicine at the University of Washington, Seattle, WA.
Dr. Steven Howard is Professor of Anesthesiology, Perioperative and Pain Medicine at Stanford University School of Medicine and Staff Physician at the VA Palo Alto Health Care System, Palo Alto, CA.
Dr. Mark Warner is currently President of the APSF and the Annenberg Professor of Anesthesiology, Mayo Clinic Rochester, MN.
Disclosures: Dr. Richard Urman has received APSF research funding in the past, and Dr. Steven Howard currently chairs the APSF Scientific Evaluation Committee. Neither Dr. Karen Posner nor Dr. Mark Warner have any disclosures with regards to the content of the article.
References
- Cooper JB. 10-Year program review reveals variety of topics, success of many projects. APSF Newsletter, Spring 1996. Available at https://www.apsf.org/newsletters/html/1996/spring/apsf.grnt.html. Accessed December 9, 2017.
- Posner KL. APSF Scientific Grant Program: improving patient safety through research funding. APSF Newsletter 2004;19:10–12. Available at https://www.apsf.org/newsletters/html/2004/spring/06grant.htm. Accessed December 9, 2017.
- Delson N, Sloan C, McGee, et al. Parametrically adjustable intubation mannequin with real-time visual feedback. Simul Healthc 2012;7:183-91.


 Issue PDF
Issue PDF