
Expert panelists fielded questions from the audience at the APSF- sponsored conference (at the 2017 ASA Annual Meeting in Boston, MA) entitled “Postoperative Infections: Can the Anesthesia Provider Be at Fault?” From Left to Right: Daniel Sessler, MD; G. Burkhard Mackensen, MD, PhD; Silvia Munoz-Price, MD, PhD; Richard C. Prielipp, MD, MBA; and David J. Birnbach, MD, MPH.
Richard C. Prielipp, MD, MBA, FCCM, professor of Anesthesiology at the University of Minnesota, introduced this provocative and timely topic on October 21, 2017, at the ASA Annual Meeting by noting that two million hospitalized patients develop health-care-associated infections (HCAI) annually, contributing to over 90,000 deaths each year in the United States.1 The source of these infections may be unknown, but the consequences are profound, including increased costs, selection pressure for drug resistant organisms, patient and family dissatisfaction, increased morbidity and mortality, and even potential liability. Surgical site infections (SSI) are especially relevant to the anesthesia community, as they account for 20% of all HCAI. Indeed, SSI afflict 1–3% of all surgical patients, increasing the hospital length of stay (LOS) from 3 to 10 days and increasing mortality 2- to 10–fold.1 Because the majority (60% or more) of SSI are considered preventable, payers and insurers may no longer cover the incremental cost of approximately $20,000 per episode.
Heightening the concern of anesthesia professionals, Dr. Prielipp noted a recent study that identified bacterial contamination of drugs during routine administration of anesthesia in the operating theater. Over 6% of microbial filters placed in standard IV tubing of anesthetized patients were contaminated with Staphylococcus (S.) capitis, S. hemolyticus, Corynebacterium, and Bacillus species.2 Equally alarming, 2.4% of fluid samples from the residual drug within syringes at the end of cases grew these same organisms, plus Staphylococcus aureus and S. hominus. Thus, there seems little doubt that anesthesia caregivers have a substantial stake in understanding and preventing SSI (Figure 1).
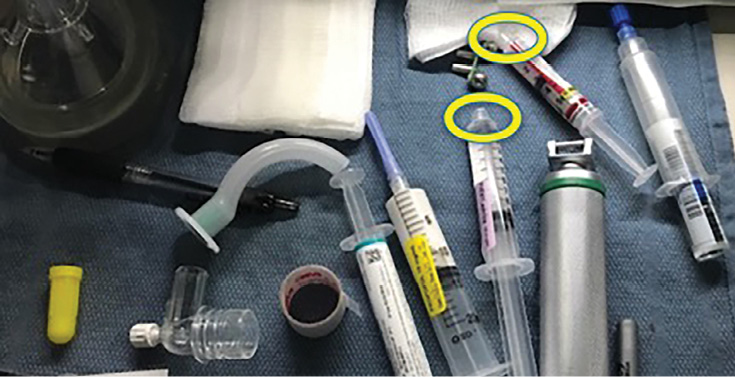
Figure 1: Intraoperative photograph of the anesthesia work surface during the maintenance phase of a routine general anesthetic. Note two medication syringes are uncapped (circled highlights) while in close proximity to the patient’s airway equipment.
Silvia Munoz-Price, MD, PhD, enterprise epidemiologist and professor of Medicine, Division of Infectious Diseases at the Medical College of Wisconsin, led an engaging discussion of the interactions between anesthesia professionals and operating room equipment, the anesthesia machine, monitor surfaces, vascular catheters, stopcocks, and intravenous tubing. She noted the frequency of these interactions during 8 hours of operating room (OR) observation during which the anesthesia provider touched surfaces 1,132 times, completed 66 stopcock injections, and inserted 4 vascular catheters. Unfortunately, appropriate hand hygiene preceded only a small fraction of these anesthesia actions.
In addition, Dr. Munoz-Price enlightened the audience of approximately 250 participants about key features of environmental disinfection (“room cleaning” between patients). Surfaces in a typical OR are likely to grow pathogens such as methicillin-resistant Staphylococcus aureus (MRSA), vancomycin-resistant enterococci (VRE), methicillin-sensitive Staphylococcus aureus (MSSA), E. coli, and Acinetobacter spp. after room cleaning! Decontamination of the environment becomes critical as additional evidence highlights that the probability of bacterial growth in injection stopcocks is a function of the number of bacterial colonies infesting the anesthesia machine as well as baseline hand contamination of anesthesia providers.3 Dr. Munoz-Price described the “Fecal Patina,” as the coating of enteric organisms that are not only limited to the patient’s skin, but also are on common surfaces in the health care environment that are touched and contaminated by patients and health care providers. Clinicians will likely identify several avenues to improve disinfection practices in their own institution to battle this “Fecal Patina in the Anesthesia Work Area.”4
David J. Birnbach, MD, MPH, Miller Professor of Anesthesiology, senior sssociate dean for Patient Safety and vice provost at the University of Miami, illustrated how readily—and rapidly—anesthesia providers’ hands can contaminate the anesthesia work surfaces within a few minutes after routine induction and endotracheal intubation.5,6 Dr. Birnbach presented data concerning contamination of presumably clean OR surfaces following intubation and showed powerful visual evidence of contaminated areas using fluorescent techniques. Of particular interest, Dr. Birnbach showed evidence of 100% contamination of the IV hub, anesthesia circuit, and anesthesia cart (Figure 2). In addition, he showed compelling evidence of contamination of unused syringes, suggesting that all syringes (even if unused) be discarded at the end of each case. Several recommendations were made regarding methods to reduce OR contamination, including the potential advantages of anesthesia professionals wearing double gloves during intubation.6,7
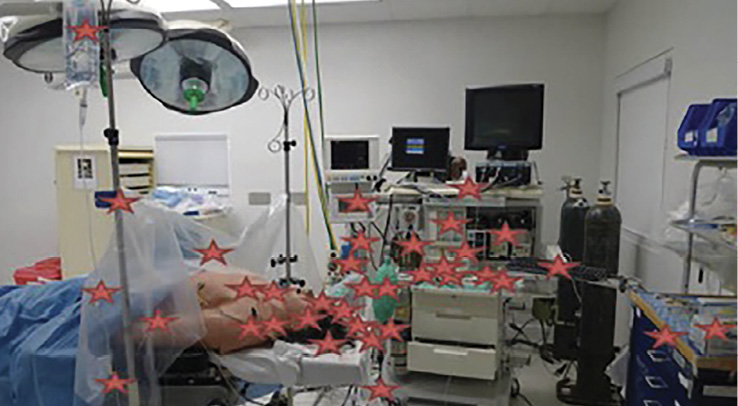
Reproduced and modified with permission. Birnbach DJ, Rosen LF, Fitzpatrick M, et al. Double gloves: a randomized trial to evaluate a simple strategy to reduce contamination in the operating room. Anesth Analg 2015;120:848–52.
Figure 2: Anesthesia residents (unaware of the study design) performed routine induction of general anesthesia with endotracheal intubation in a high-fidelity simulator. Invisible fluorescent dye—secretly painted in the “patient’s mouth”—was traced to an alarming multitude of anesthesia work surfaces within six minutes of the start of anesthesia (each star indicates contamination by the oral tracer).6
Dr. Birnbach completed his talk with a discussion of neurologic infections due to contamination by the anesthesia professional. He highlighted several cases of meningitis where the causative bacteria were isolated from the anesthesiologist’s nasopharynx8 and informed the audience about the scientific literature suggesting the importance of routinely wearing masks during placement of neuraxial blockade.
G. Burkhard Mackensen, MD, PhD, FASE, professor in the Department of Anesthesiology and Pain Medicine at the University of Washington, and chief of the Division of Cardiothoracic Anesthesia, provided an illuminating discussion regarding reusable vs. disposable laryngoscopes. Flexible and rigid laryngoscopes—both blades and handles—are classified as semicritical devices (because they contact mucous membranes), and therefore require both cleaning and high-level disinfection or sterilization. He cited the deaths of two infants in a California neonatal ICU due to an outbreak of Pseudomonas aeruginosa attributed to reusable laryngoscopes used during their hospitalization.9 However, many institutions are discovering that the cost of reprocessing reusable laryngoscopes to this new standard is substantial. While cost allocation data depend on your specific organization, adopting single-use products may actually be quite favorable and even less expensive. Table 1 compares several aspects of these two laryngoscope options.
| Table 1: Comparison of Reusable to Disposable, Single-Use Laryngoscopes | |
| Traditional, Reusable Laryngoscopes | Single Use (‘Disposable’) Laryngoscopes |
| Batteries wear out, need replacement | Batteries always brand new |
| Bulbs dim and eventually burn out | Light source always new |
| On-off switch prone to wear and failure | Switch is new; testable while still in package |
| Handles require disassembly to disinfect | No cleaning or maintenance of device |
| Requires sterilization or high-level disinfection after each use | Provided sterile in new, transparent package |
| Costs rise rapidly with newly required processing and sterilization | Costs at parity or even less expensive depending on the institution20 |
| Performance is well known with a familiar feel | Performance now usually rated at parity with reusable laryngoscopes21 |
Daniel Sessler, MD, discussed hypothermia and other related factors as he highlighted several confounding variables related to SSI. He began by noting how general and neuraxial anesthetics profoundly impair thermoregulatory control. Consequently, nearly all unwarmed surgical patients become hypothermic. Intraoperative hypothermia results initially from a core-to-peripheral redistribution of body heat; thereafter, it results from heat loss exceeding metabolic heat production.10 Randomized trials have shown that mild hypothermia increases blood loss and transfusion requirements,11 promotes surgical site infection,12 and slows drug metabolism thereby prolonging recovery. Professional groups in various countries have, therefore, published guidelines indicating that core temperature should be monitored during both general and neuraxial anesthesia, and that surgical patients should be kept normothermic.
Forced-air warming (FAW) is by far the most commonly used intraoperative warming system worldwide, but clinicians are free to adopt any system that keeps patients normothermic. In recent years, there has been some concern that forced-air might disturb laminar flow and thus promote infection during orthopedic procedures. In fact, Brandt and colleagues suggested that laminar flow increases infection risk,13presumably by detaching bacteria-laden particles from the heads of surgeons and scrub nurses, and driving them directly into the surgical wound. However, the only clinical study of forced-air and laminar flow showed that there was no interference whatsoever.14 Supporting this conclusion, the United States Food and Drug Administration in August of 2017 provided the following guidance: “The FDA has been unable to identify an association between forced-air (FAW) and surgical site infection. Therefore, the FDA continues to recommend the use of thermoregulating devices (including forced air thermal regulations systems).”
In addition, to the effects of hypothermia on infection risk, Dr. Sessler provided evidence to support the following concepts:
- Timely antibiotic administration helps to reduce surgical site infections.15
- Supplemental oxygen does not seem to reduce risk of infection.16
- Little evidence supports which fluid strategy and what type of fluid may reduce infection risk.17,18
- Smoking increases infection risk but it is presently unknown if perioperative cessation reduces this risk.19
The panelists concluded by answering questions from the engaged audience of approximately 250 participants.
Dr. Richard C. Prielipp is Professor of Anesthesiology at the University of Minnesota in Minneapolis. He serves on the Board of Directors of the APSF.
Dr. David J. Birnbach is Miller Professor of Anesthesiology, Senior Associate Dean for Patient Safety and Vice Provost at the University of Miami. He serves on the Board of Directors of the APSF.
Both report no COI relevant to this presentation.
The opinions expressed in this article are not necessarily those of the Anesthesia Patient Safety Foundation. The APSF neither writes nor promulgates standards, and the opinions expressed herein should not be construed to constitute practice standards or practice parameters. Validity of opinions presented, drug dosages, accuracy, and completeness of content are not guaranteed by the APSF.
References
- Davis CH, Kao LS, Fleming JB, et al. Multi-institution analysis of infection control practices identifies the subset associated with best surgical site infection performance: A Texas Alliance for Surgical Quality Collaborative Project. J Am Coll Surg 2017;225:455–464.
- Gargiulo DA, Mitchell S, Sheridan J, et al. Microbiological contamination of drugs during the administration for anesthesia in the operating room. Anesthesiology2016;124:785–94.
- Loftus RW, Muffly MK, Brown JR, et al. Hand contamination of anesthesia providers is an important risk factor for intraoperative bacterial transmission. Anesth Analg 2011;112:98–105.
- Munoz-Price LS, Weinstein RA. Fecal patina in the anesthesia work area. Anesth Analg 2015;120:703–705.
- Birnbach DJ, Rosen LF, Fitzpatrick M, et al. The use of a novel technology to study dynamics of pathogen transmission in the operating room. Anesth Analg2015;120:844–47.
- Birnbach DJ, Rosen LF, Fitzpatrick M, et al. Double gloves: a randomized trial to evaluate a simple strategy to reduce contamination in the operating room. Anesth Analg 2015;120:848–52.
- Birnbach DJ, Rosen LF, Fitzpatrick M, et al. A new approach to pathogen containment in the operating room: sheathing the laryngoscope after intubation. Anesth Analg 2015;121:1209–14.
- Schneeberger PM, Janssen M, Voss A. Alpha-hemolytic streptococci: a major pathogen for iatrogenic meningitis following lumbar puncture. Infection 1996;24:29–33.
- Muscarella LF. Reassessment of the risk of health care-acquired infection during rigid laryngoscopy. J Hosp Infect 2008;68:101-7.
- Sessler DI: Perioperative thermoregulation and heat balance. Lancet 2016;387:2655–64.
- Rajagopalan S, Mascha E, Na J, et al. The effects of mild perioperative hypothermia on blood loss and transfusion requirement: a meta-analysis. Anesthesiology 2008;108:71–7.
- Kurz A, Sessler DI, Lenhardt RA. Study of wound infections and temperature group: perioperative normothermia to reduce the incidence of surgical-wound infection and shorten hospitalization. N Engl J Med 1996;334:1209–15.
- Brandt C, Hott U, Sohr D, et al. Operating room ventilation with laminar airflow shows no protective effect on the surgical site infection rate in orthopedic and abdominal surgery. Annals of Surgery 2008;248:695-700.
- Oguz R, Diab-Elschahawi M, Berger J, et al. Airborne bacterial contamination during orthopedic surgery: A randomized controlled pilot trial. J Clin Anesth 2017;38:160–64.
- Berríos-Torres S, Umscheid CA, Bratzler D, et al. Centers for Disease Control and Prevention guideline for the prevention of surgical site infection. JAMA Surgery 2017;152:784–791.
- Wetterslev J, Meyhoff CS, Jorgensen LN, et al. The effects of high perioperative inspiratory oxygen fraction for adult surgical patients. Cochrane Database Syst Rev2015;25:1–80.
- Kabon B, Akca O, Taguchi A, et al. Supplemental intravenous crystalloid administration does not reduce the risk of surgical wound infection. Anesth Analg2005;101:1546–1553.
- Wakeling HG, McFall MR, Jenkins CS, et al. Intraoperative oesophageal Doppler guided fluid management shortens postoperative hospital stay after major bowel surgery. Br J Anaesth 2005;95:634–642.
- Gronkjaer M, Eliasen M, Skov-Ettrup LS, et al. Preoperative smoking status and postoperative complications: a systematic review and meta-analysis. Ann Surg2014;259:52–71.
- McGain F, Story D, Lim T, et al. Financial and environmental costs of reusable and single-use anaesthetic equipment. Brit J Anaesthesia 2017;118:862-869.
- Amour J, Le Manach Y, Borel M, et al. Comparison of single-use and reusable metal laryngoscope blades for orotracheal intubation during rapid sequence induction of anesthesia: a multicenter cluster randomized study. Anesthesiology 2010;112:325-32.


 Issue PDF
Issue PDF