Pioneering Success in Safety, But Challenges Remain
- Success and Recognition
- Original Serendipitous Coincidence
- APSF Organized
- Early Action
- Simulation Targeted
- Evolution
- Spreading the Word
- Advantageous Alliances
- New News
- Copious Concerns
- Research Renaissance
- Structural Scaffolding
- Reflections and Conclusion
- Acknowledgments
 A quarter-century after establishing “patient safety” as a specific concept and a discipline, the Anesthesia Patient Safety Foundation (APSF) pauses in the autumn of 2010 for its 25th anniversary celebration to reflect on its innovative contributions and accomplishments and also on the many challenges yet ahead.
A quarter-century after establishing “patient safety” as a specific concept and a discipline, the Anesthesia Patient Safety Foundation (APSF) pauses in the autumn of 2010 for its 25th anniversary celebration to reflect on its innovative contributions and accomplishments and also on the many challenges yet ahead.
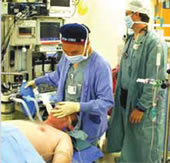
Technological intensification in the OR has increased monitoring and equipment training needs.

Dr. Ellison C. (Jeep) Pierce, Jr., receives award from Dr. Robert K. Stoelting at his retirement from APSF.
From the start, the APSF has been driven by the vision “that no patient shall be harmed by anesthesia.” The APSF was the very first patient safety organization. While rarely recognized as the true pioneer it is, the APSF can legitimately be credited with igniting the “patient safety movement” which has (appropriately) blossomed into one of the major forces in modern health care everywhere. Every patient safety organization, committee, and program as well as every patient safety department and officer have followed after the original inspiration of the APSF. The “patient safety movement” was borne from the profession of anesthesia, where the term “patient safety” originated. The APSF was, and remains, the driving force behind this movement as the organizational catalyst.
As detailed below, while inspiring so many others outside anesthesiology, the APSF has worked tirelessly since 1985 to accomplish its mission: “to improve continually the safety of patients during anesthesia care by encouraging and conducting:
- Safety research and education;
- Patient safety programs and campaigns;
- National and international exchange of information and ideas.”
Since its first issue in 1986, the APSF Newsletter has been a main vehicle for communication and education on issues related to anesthesia and patient safety. This highly respected quarterly publication became, and remains, the anesthesia publication with the largest circulation in the world and serves to transmit safety-related news, ideas, and opinions. The APSF research grant program helped validate high-fidelity simulation as an education and research tool and, beyond that, has funded many projects that have provided insight into and suggested solutions for safety problems. Over the years a cadre of patient safety investigators has evolved as a result of the APSF research program. Safety advocacy and educational efforts have included publication of books, co-sponsorship of a large video series, and organization of the heavily-trafficked “patient safety booth” among the exhibits at the ASA and AANA annual meetings. More recently, APSF has sponsored targeted workshops and consensus conferences resulting in recommendations for definitive action. It now hosts the popular APSF website (www.apsf.org) that includes a wealth of safety-related resource material and attractive interactive features such as the monthly poll on a current anesthesia question and also the Virtual Anesthesia Machine, which the APSF helped to support over the years.
Success and Recognition
The success of the anesthesia patient safety movement was recognized significantly in 1996 when the American Medical Association and corporate partners founded the National Patient Safety Foundation (NPSF), based directly on the APSF as the model. The NPSF persists today as a major national and international force in patient safety advocacy. Further recognition of the APSF for leadership and safety efforts came in the landmark 1999 report “To Err is Human” from the Institute of Medicine on morbidity and mortality caused by errors in medical care. The APSF was the only organization mentioned as one that had made a demonstrable positive impact on patient safety. [While honored, the APSF felt compelled to publicly respond to the IOM report and advocate for more of a quality management “systems” approach to patient safety rather than their proposed program to identify and punish “bad practitioners.”] Further, a June 21, 2005, front page article in the Wall Street Journal singled out the anesthesia profession, the ASA, and APSF for their roles in making anesthesia safer resulting in dramatic decreases in professional liability insurance premiums paid by anesthesiologists.
A “culture of safety” has developed in anesthesia practice, by the hard work of the APSF, the ASA, the AANA, and as well as by the adoption of a more systems-based approach by many anesthesia departments and groups and all of the anesthesia professionals interested in optimizing anesthetic outcomes. Overall, the combined impact of all these efforts has been a 10- to 20-fold reduction in mortality and catastrophic morbidity for healthy patients undergoing routine anesthetics. This is an evolutionary accomplishment of which the entire profession can be justifiably proud. By the early 1990s, liability payouts from anesthesia accidents had decreased from a disproportionately high share to something less than would be expected for such inherently risky work. The insurance “risk relativity rating” for anesthesia practice compared to other specialties had been reduced dramatically.
Original Serendipitous Coincidence
As with most major historical developments, coincidence played a role in the creation of the APSF. Several factors came together to facilitate the development of an idea held by Ellison C. (“Jeep”) Pierce, Jr., MD, who was then chair of Anesthesia at the New England Deaconess Hospital in the Harvard Medical School system. As he related in his 1995 Rovenstine lecture to the ASA,1 Dr. Pierce was originally stimulated in 1962 as a junior faculty member when assigned to give a lecture on “anesthesia accidents.” After that, he kept files, notes, and clippings and spoke often of his concerns about major anesthesia accidents that harmed patients, particularly unrecognized esophageal intubations. Then, in April 1982, the ABC television program 20/20 aired a segment entitled “The Deep Sleep: 6,000 Will Die or Suffer Brain Damage.” It opened with: “If you are going to go into anesthesia, you are going on a long trip and you should not do it, if you can avoid it in any way. General anesthesia is safe most of the time, but there are dangers from human error, carelessness and a critical shortage of anesthesiologists. This year, 6,000 patients will die or suffer brain damage.” Following scenes of patients who suffered anesthesia mishaps, the program went on to say, “The people you have just seen are tragic victims of a danger they never knew existed—mistakes in administering anesthesia.” In another example shown on the program a patient was left in a coma following the anesthesiologist’s error in turning off oxygen rather than nitrous oxide at the end of an anesthetic. This watershed presentation provoked public concern about the safety of anesthesia. Dr. Pierce transformed this potential problem for the specialty into an opportunity to take positive, proactive measures. Taking advantage of his impending year as ASA president starting in October 1983, he convinced the ASA leaders to create the Committee on Patient Safety and Risk Management. He saw that the problems of anesthesia accidents and malpractice costs had the same solution—making anesthesia safer.

At the same time, ground-breaking research led by Jeffrey B. Cooper, PhD, a bioengineer in the Department of Anesthesia at the Massachusetts General Hospital, had focused on revealing how human errors were a major and fundamental cause of preventable anesthesia accidents. He and his colleagues adapted the techniques of “critical incident analysis,” used in the study of aviation accidents, to study analogous events that were occurring in anesthesia.2 Based on Cooper’s work, Richard J. Kitz, MD, then chair of that anesthesia department, lectured on this topic in England to the Royal College of Anaesthetists. The esteemed Professor T. Cecil Gray was in the audience. He was stimulated to suggest that an international meeting be convened to reveal more about these preventable anesthesia injuries. Dr. Kitz brought the idea to Drs. Cooper and Pierce, who was by then president of the ASA. The three collaborated to organize and host in Boston the International Symposium on Preventable Anesthesia Mortality and Morbidity in 1984, timed to follow immediately the ASA meeting that year. Fifty invited participants attended and grant support from various corporations was raised to fund the meeting. At the closing session, Dr. Pierce reflected on the obvious great interest and relevance of the topic, the lively debate, the need for action, and the potential to raise funds to support efforts to make anesthesia safer. After the close, a small nuclear group stayed behind and Dr. Pierce outlined his proposal to build on the idea and create an independent foundation dedicated solely to improving the safety of anesthesia care to the point “that no patient shall be harmed by anesthesia.” Enthusiastic agreement was unanimous. Dr. Pierce asked, “What should we call it?” Dr. Cooper suggested that it simply be called what it would be, the “Anesthesia Patient Safety Foundation.” And, so it was.
APSF Organized 

Front page of the first issue of the APSF Newsletter, Vol.1, No.1, March 1986 with a photo of the first APSF Executive Committee members.
Dr. Pierce, having just finished his term as ASA president, envisioned a relatively small dedicated core group driving an independent foundation that was not directly controlled by any large organization. This would facilitate nimble, rapid, targeted action unfettered by a slow bureaucratic approval process and also open engagement on the politically sensitive topic of anesthesia accidents. Importantly, this would allow a very broad base of participants including all possible interested groups of constituents: anesthesiologists, nurse anesthetists, nurses, bioengineers, epidemiologists, equipment and pharmaceutical manufacturers, government regulators, risk managers and insurance industry executives, and even surgeons.
An organizational executive meeting was held in July 1985. Initial goals for the APSF were established:
- Sponsor investigations that will provide a better understanding of preventable anesthetic injuries.
- Encourage programs that will reduce the number of anesthetic injuries.
- Promote national and international communication of information and ideas about the causes and prevention of anesthetic injuries.
- Establish an information newsletter to be delivered free of charge to all anesthesia providers.
Potential by-laws, committees, directors, and funding were discussed. Dr. Pierce agreed to approach the ASA with a request for an annual contribution equivalent to the funding for the ASA Committee on Research.
At the 1985 ASA meeting, over 30 potential APSF officers and dirctors met. Importantly, an initial contribution of $100,000 from the ASA had been secured and this also was matched by contributions from the Parker B. Francis Foundation (an offshoot of the Puritan Bennett Corporation) and from Ohmeda, Inc. Accordingly, with the viability of the foundation clearly established, the articles of incorporation dated October 2, 1985, were accepted. It was then agreed that the four officers would be members of a 7-person executive committee (EC) and that there would be a 30-person Board of Directors with half appointed by the ASA and half by the APSF.
By the time of the New York Post-Graduate Assembly in December, the EC was set:
- President: Ellison C. Pierce, Jr., MD
- Vice President: W. Dekle Rountree, Jr. (CEO of Ohmeda)
- Secretary: E.S. Siker, MD (a past president of the ASA)
- Treasurer: Burton S. Dole (CEO of Puritan Bennett)
- At large: Jeffrey B. Cooper, PhD, Joachim S. Gravenstein, MD, and James E. Holzer (CEO of the Risk Management Foundation, Harvard’s liability insurer)
Committees were addressed. The proposed quarterly newsletter was considered the top priority. Dr. Pierce, recognizing the potential value of the prior newspaper editing experience of John H. Eichhorn, MD, persuaded him to create and edit the APSF Newsletter and chair the editorial board. An ambitious target was set to publish the first issue that coming March (which was achieved). The research grant program was the other priority. Arthur S. Keats, MD, was named chair of the Scientific Advisory Committee. He stated his intention to structure this effort along the rigorous lines of an NIH study section, including seasoned senior researchers as grant reviewers. The Committee on Education and Training was formed and J. S. Gravenstein, MD, was appointed as its chair. The Committee on Technology was also formed (David B. Swedlow, MD, would later become its chair).
All but one of the members of the Board of Directors were appointed. As hoped, and crucial to the undertaking, the make-up of the Board did achieve the goal of an extremely wide cross-section of professionals interested in anesthesia patient safety and empowered to act on that interest. Included were relevant ASA committee chairs, officials, and members who were respected researchers, as well as representatives of the profession of nurse anesthesia, the medical liability insurance industry, the FDA, and anesthesia equipment and pharmaceutical corporations.
At that meeting, a proposal was adopted that the first APSF research grants would be awarded at the APSF annual meeting in October 1986, in the amount of up to $35,000. Also, a lively discussion about the potential value of standards for intraoperative monitoring and whether the APSF could have a role was held with no resolution or recommendation resulting. Dr. Pierce initiated that discussion in part because of his awareness of three related efforts: the work of the Harvard Risk Management Committee, chaired by Dr. Eichhorn, and the recent adoption of formal anesthesia monitoring standards within the Harvard system; a meeting of an industry-sponsored “Anesthesia Safety Consortium” that wanted to support standards; and the work on monitoring by the newly formed ASA Committee on Standards of Care (initiated during Dr. Pierce’s presidency of the ASA). Eventually a consensus was achieved that the APSF would not hold itself out as a formal standards-setting organization but rather would focus on education and advocacy to further the improvement of anesthesia patient safety.
Early Action
Organizational efforts came to fruition. Bookkeeping and secretarial functions were formalized and divided among the ASA office, Dr. Pierce’s office in Boston, and Dr. Siker’s office in Pittsburgh. Efforts to create, edit, print, and mail the initial Newsletter proved to be a formidable task for Dr. Eichhorn. That work was significantly facilitated by a generous further donation to the APSF from Mr. Dole and the Puritan Bennett Corp. of free use of that company’s graphic arts and printing facilities outside Kansas City. (Likewise, somewhat later, an additional contribution from The Hewlett-Packard Company of what was then novel technology, a computer that did word processing, also helped the publishing process.)
The first issue of the Newsletter was mailed to 45,000 recipients (ASA, AANA, risk managers, corporate and international supporters) in March 1986. Beyond the lead story about the creation of APSF, there was a long article by Dr. Gravenstein questioning whether there was such a concept as “minimal intraoperative monitoring” and also a report of the initiation of the ASA Closed Claims Study. Other stories concerned the expansion of the Confidential Enquiry into Perioperative Death in England, the publication of the statistics on cardiac arrest due to anesthesia at one teaching hospital, and a discussion of the relative dangers of hypoxemia and hypercarbia. The first Newsletter was very well received and set the tone for all subsequent issues. Later the first year, there were discussions of: an ECRI report on “Deaths during General Anesthesia,” verification of correct endotracheal tube placement, analysis of anesthesia deaths in Australia, and decreasing anesthesia claims at one major insurance company. There was announcement of the first FDA anesthesia machine check-out protocol and reprinting of Dr. Pierce’s important article, “Risk Modification in Anesthesiology.” Standards figured prominently in early issues as there was extensive discussion of the 1986 ASA adoption of “Standards for Basic Intra-Operative Monitoring” and also the various evolving anesthesia machine device and performance standards (fresh gas ratio protection, vaporizer exclusion, etc.) intended to enhance safety. Strong support for the universal use of intraoperative pulse oximetry, and later capnography, was a major early APSF theme. This support contributed to the establishment of these monitors as standards of care, which significantly help ensure patient safety to this day. The concept of special safety risks outside traditional hospital operating rooms was introduced in the Newsletter, as was the idea of support systems to facilitate the conduct of anesthesia practice, and the idea of provider fatigue as a special danger to anesthetized patients.
The APSF partnered in the beginning with the ASA in co-producing a series of educational videotapes about a wide variety of anesthesia patient safety topics. Dr. Pierce was intensely involved in many of the productions. The finished tapes were distributed to all anesthesia departments in the U.S. by what was then the Burroughs-Wellcome Co. This tradition continued for many years but eventually fell victim to rising costs, corporate consolidations, and evolving media. (However, just recently, such efforts were revived when the APSF partnered with ECRI Institute to produce and distribute a DVD on “Prevention and Management of Operating Room Fires.”)
The APSF tradition of education and advocacy though targeted workshops, seminars, and task forces began in 1987 with the convening of a 2-day meeting, “Safety and Cost Containment in Anesthesia.” Critical issues of danger to patients created by enforced cost-cutting measured were discussed in detail and contrasts made with the safety conscious commercial aviation industry. The proceedings were published in a book that was used in many hospitals to help advocate for resources (as also were various issues of the Newsletter when key safety programs and equipment were presented). An early workshop focused on “Needed Research in Patient Safety.” However, there was a learning curve. An overly ambitious proposed national APSF Grand Anesthesia Safety Symposium (“GASS”) was cancelled due to a paucity of registrants. Nevertheless, after gaining better organizational skills, in 1990, the APSF, partnering with the FDA, convened an unprecedented expert workshop on human error in anesthesia practice that helped stimulate later advances.
Sponsorship of patient safety research was (and remains) one of the core goals of APSF. In the first year, 27 research grant applications were received and 4 grants were awarded. The titles of the 4 were “Defining Outcomes Associated with Anesthesia,” “A safer Anesthesia Machine Through Model-Based Alarms,” “The Risk of Surgery and Anesthesia: A Retrospective Analysis,” and, from David M. Gaba, MD of Stanford, “Evaluation of Anesthesiologist Problem Solving Using Realistic Simulations.” Dr. Gaba went on to become one of the founders and leaders of using high-fidelity simulation in patient safety, human factors research, and medical training and research in general, as well as a fixture in the APSF leadership. Others researching human factors have also been supported, and they have contributed to the understanding of the fine details of our OR practices and their safety implications. The first APSF Young Investigator award went to Richard I. Cook, MD, a computer scientist before he became an anesthesiologist, to study the impact of high-tech equipment such as integrated monitors on practice behavior in the OR. Each year since 1986, the research grant recipients and outlines of their projects appear in the Winter issue of the APSF Newsletter (the complete catalogue of which is readily available on the website: www.apsf.org). Periodically, articles in the Newsletter (Winter, 1994; Spring, 1996; Spring, 2004) have reviewed completed projects and lists of peer-reviewed publications resulting from research funded by APSF grants and also presented follow-up reports of particularly valuable research results. One prominent early example was an important study from the Massachusetts General Hospital that showed the complementary intertwined value of adding capnography to pulse oximetry as a routine intraoperative monitor. Those data soon played a significant role in the evolution of the ASA monitoring standards, changing the routine use of end-tidal carbon dioxide monitoring from recommended to mandatory, which the APSF supported and promoted. APSF funding supported the initial development of “smart alarms” on patient monitors and anesthesia machines. Likewise, seminal human factors research into how anesthesia professionals see, absorb, and process monitoring information was funded by APSF.
Simulation Targeted
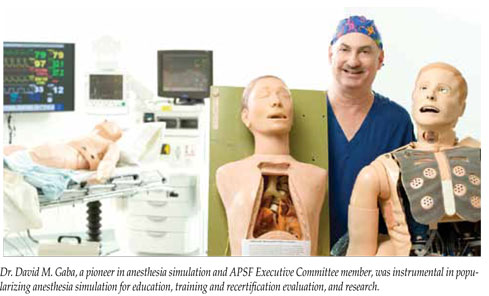
The APSF helped organize in 1988 what well may have been the first meetings on medical simulation, featuring 8 types of simulators. Then, in 1989 the APSF sponsored the Anesthesia Simulator Curriculum Conference that, despite just dodging a hit from Hurricane Hugo, attracted 92 exhibitors and educators to an intense, extremely productive meeting that included the first attempt at collaboration to advance anesthesia simulator technology. In 1995, APSF convened a national conference on simulation in anesthesia education. Overall, the APSF extensively supported (intense advocacy, and both regular and special research grant funding over several years) the development and implementation of simulation in anesthesia. The APSF had a major early role in catalyzing and supporting simulation to become a significant tool in research (human performance), training (teamwork, crisis management), and education (residents attempting new skills and procedures for the first time on a mannequin rather than an actual patient). Again, while little recognized over the years, the APSF appropriately deserves credit for a truly pivotal role in the development and popularization of medical simulation, which is now a hugely successful, universal, integral component of health care. As true with the original concept of patient safety and with formal standards of care, with simulation, the profession of anesthesiology was there first and should be proud of its leadership. This theme is well captured in a book summarizing the formative years of the APSF, including reprints of key Newsletter articles.4
Evolution
One important function provided by the APSF over the early years was the documentation of the decrease in morbidity and mortality from anesthesia accidents—the beginning of the remarkable improvement in anesthesia patient safety that persists today. There were multiple Newsletter articles, mainly from malpractice insurance companies in the U.S. and from safety researchers in several other countries, as well as editorials and reports at APSF meetings that discussed statistics, trends, and observations of the positive evolution of the safety of anesthesia care. An interesting footnote is a 1990 Newsletter announcement that the ASA had published a 12-page brochure, “FYI… A commitment to Patient Safety,” its first on this topic, for distribution to the public and all interested parties, which contained prominent reference to the ASA’s support of the APSF.
The APSF/Ellison C. Pierce, Jr. Award was established for presentation to the exhibitor and sponsor of the Scientific Exhibit at the ASA Annual Meeting that best demonstrates new and effective methods of safe anesthesia practices. Its first presentation in 1989 recognized an exhibit describing improved approaches to airway management in the OR, one of several winners on this general topic over the years. That October, a runner-up was named and singled out for distinction; it was an exhibit of a computer-generated screen-based anesthesia simulator. Furthermore, each year since its creation, the APSF Newsletter has carried an extensive account of the patient-safety related presentations and activities at the ASA Annual Meeting. Possibly one of the most dramatic illustrations of the evolution of anesthesia patient safety is the increase in the emphasis on patient safety at this meeting. It started with a handful of presentations in the late 1980s that had been added to the end of “more traditional” abstract sessions and grew consistently until now when there are multiple entire abstract and poster sessions involving well over a hundred safety-related presentations spread over the entire meeting.
Spreading the Word
Implementing one of the APSF core goals, rapid communication of safety-related clinical information directly relevant to the primary practice of anesthesia professionals, the APSF has consistently over its history received, researched, and publicized alerts on previously unknown issues. The APSF thus has been a key central clearing house for critical safety information, one of its most important and well-recognized roles in promoting patient safety. In 1991, the Newsletter published the first report of “Monday morning carbon monoxide poisoning” from the unusual interaction of desiccated CO2 absorbent material with halogenated volatile anesthetics. That went on to become a major national story, one that later stimulated the APSF into sponsoring a national workshop to review the topic of CO2 absorbents and refine recommendations for action. More recently, the related issue of “canister fires” was first publicized by the APSF. Support for and publicity of the ASA Difficult Airway Algorithm has been consistently strong, and this was the subject of one of the APSF videotapes. Checklists such as the pre-anesthesia machine check-out, particularly emphasizing the analogy to pilots preparing for takeoff, have been continually promoted. Latex allergy danger, when it first came to prominence in anesthesia practice, was the subject of an APSF campaign. The first discussion of potential patient danger from sevoflurane contaminated with acid from an alteration in its manufacturing process was published in the APSF Newsletter (along with an outline of the remedial action by the manufacturers). The question of danger to allergic patients from the inclusion of sulfite as a preservative in a new formulation of propofol was first raised by an alarming communication to the Newsletter from a prominent academic department chair who noted he himself was at risk. More recently, the danger of outbreaks of infectious complications, particularly hepatitis, from use of syringes of anesthetic medication on more than one patient were broadcast by APSF. Another of the widely-quoted “alert” functions has been served by the APSF calling attention to reports of unusual events that harmed patients. One prominent example concerned the unfortunate death of a patient whose IV tubing had been connected to his tracheostomy tube cuff inflation port instead of the adjacent central venous catheter, highlighting the issue of dangers from connection compatibilities (a problem that continues to defy solution). Others involved obstruction to ventilation from a variety of objects somehow accidentally getting wedged in breathing circuits, connectors, or tubes as well as fires that started due to damaged O2 tank gaskets.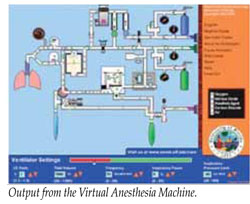
Another key opportunity to raise awareness and advocate for anesthesia patient safety occurs each October at the ASA annual meeting where the APSF “patient safety booth” sits prominently in the exhibit hall. Skillfully organized and crafted by Dr. Robert A. Caplan of the APSF Executive Committee, the booth draws in passers-by with bold displays of intensely relevant current patient safety news, reprints of and from the Newsletter, as well as on-screen presentations of safety videos and the Virtual Anesthesia Machine program. A fairly frequent comment from booth visitors is something like, “Wow, I didn’t know you guys did all this.”
In the 1990s Dr. Pierce was appointed as the ASA representative to the AMA’s newly formed forum on the then-new idea of “practice parameters.” He, as a safety expert and as a representative of the APSF, advocated vigorously for the ASA to adopt the practice parameter model, which thrives still today as a significant tool in advancing patient safety.
The patient risks associated with anesthesia professionals not fully familiar with or understanding their own equipment, particularly ever-increasingly complex anesthesia machines, monitors, pumps, etc., were recognized early on by the APSF. This topic in various forms has been (and still is) a major emphasis of the Committee on Technology, the Committee on Education and Training, and the subject of research, workshops, dedicated meetings, and widespread publicity.
One activity that has been especially well received has been the surveys of anesthesia professionals conducted by the APSF. One of the best-known surveys was conducted in late 1998. It asked what were the most important issues (associated with the greatest risks) in anesthesia patient safety. The results (percent of respondents naming an issue) were:
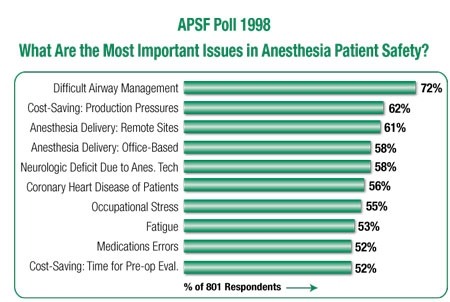
Interestingly, while the terminology and definitions may have changed slightly, these issues likely would be similarly identified today. For the past few years, the APSF website has included a participant poll on one safety issue of interest each month or so. The results appear and stay on the website. Recent poll questions concerned post-op monitoring of OSA patients getting PCA, substitute drugs when propofol is unavailable, and management of patients in the beach-chair position for shoulder surgery. Another service at one point was the compilation in one file of the applicable regulations from all 50 states governing office-based anesthesia, which was then provided as a resource to anyone interested in this often contentious topic that directly impacts anesthesia patient safety.
Advantageous Alliances
Collaboration with other professional organizations interested in patient safety has consistently been a feature of APSF activities. A few years ago, the APSF partnered with the American College of Surgeons to submit a grant application regarding the feasibility of direct electronic input of relevant data from anesthesia information management systems into the National Surgical Quality Improvement Program (NSQIP). The APSF partnered with the journal Anesthesia and Analgesia in 2007, creating a new patient safety section in that journal. The chair of the APSF Committee on Scientific Evaluation, Sorin J. Brull, MD, was named section editor. Submissions of papers concerning anesthesia patient safety and visibility of the topic have increased substantially. Also, the APSF has sponsored panel discussions at the annual meeting of the International Anesthesia Research Society, ably organized and conducted by Richard C. Prielipp, MD, chair of the APSF Committee on Education and Training.
Another major initiative arose from a collaboration (and co-funding) with the inventors and manufacturers of anesthesia information management systems (AIMS). This led APSF to organize the development of a common terminology in clinical anesthesia practice that would allow all the computerized records and information systems to generate consistent, compatible (and comparable) data with standardized definitions. Known as the Data Dictionary Task Force, this effort has been ably chaired by Terri G. Monk, MD, and has worked for several years to develop the anesthesia lexicon for these systems. Its work product has been adopted and incorporated by national and international (IOTA = International Organization for Terminology in Anesthesia) groups responsible for establishing accepted medical terminology. This is a major accomplishment with great impact on the future of anesthesia practice. It is also another instance of very few people being aware of the key seminal role of APSF.
On a different tack, an alliance with the Society for Pediatric Anesthesia along with special APSF funding helped launch “Wake Up Safe,” a formally approved patient safety organization that is a network of pediatric hospitals within the Society for Pediatric Anesthesia with the mission of creating an incident reporting system, event analysis paradigm, and safety data clearing house. Recently, the APSF was an endorser of the World Health Organization global safety campaign, “Safe Surgery Saves Lives,” which features the “Surgical Safety Checklist,” and the APSF conducted an extensive informational campaign to help facilitate implementation.

New News
The APSF Newsletter has evolved also. Founding Editor Dr. Eichhorn turned over the proverbial editorial pen and scissors in 2002 to Dr. Robert C. Morell. The next year,
Newsletter issues became available in .pdf format on the website, so the electronic experience would closely resemble the printed hard copies, which were then mailed to nearly 73,000 readers, making it by far still the largest anesthesia publication in the world (circulation has now grown to more than 80,000). Also, full color was added to the traditional “oxygen-tank green” highlight color that had marked the publication since its birth. Spirited, stimulating “pro-con” debates played out on its pages, covering topics such as the safety implications of anticoagulation and regional anesthesia, routine succinylcholine in children, reading (and now surfing or texting) in the OR during cases (many times), risks of pulmonary artery catheterization, concentrated lidocaine in spinals, safety of PCA narcotic infusion pumps (again), and even a mock debate on syringe reuse. Later, the “Dear SIRS” column (“Safety Information Response System”) was added, initiated by Michael A. Olympio, MD, then chair of the Committee on Technology. Technical issues, often involving problems with equipment were discussed by panels of experts, including usually the manufacturer of any equipment in question. This feature quickly became one of the most popular ever in the Newsletter. On the strength of that experience, another well-liked column, titled simply “Q and A,” was added to handle many of the more focused technical questions that arrive at the APSF office and are directed to the Committee on Technology. Also, while “Letters to the Editor” always was and is a popular feature, the volume and intensity of submissions has increased in recent years. It is not unusual for there to be 8 or 10 thoughtful letters on a broad spectrum of topics published in a given Newsletter issue. Various landmark articles have had widespread impact on perceptions in anesthesia patient safety over the years. Examples include “How Safe is Safe?” by Dr. Gravenstein in 1995 and “Patient Perspectives Personalize Patient Safety,” authored by Dr. Eichhorn in 2005. The latter was a report on the dramatic APSF workshop, conceived and organized by Dr. Cooper, in which surviving family members and one actual survivor herself detailed the impact of catastrophic anesthesia accidents (including on the involved providers).
Other recent APSF workshops conducted at the time of the annual meeting reflect and illustrate several of the major initiatives of the APSF and the intense efforts to keep up momentum for improvement of anesthesia patient safety. Long-term patient outcome and the potential for deleterious effects of anesthetics (postulated by some researchers potentially to be related to provocation of inflammation by anesthesia) were dissected in one session. The safety of postoperative opioid medication, particularly administered by patient-controlled analgesia (PCA), has been considered (provoking a special Newsletter editorial: “Dangers of Postoperative Opioids—Is There A Cure?”). Medication safety in the OR and the implications of medication errors by anesthesia professionals is a recurrent subject. A recent iteration in 2008 had “Medication Mishap Mitigation” as its theme, and this was a stimulus for the comprehensive special invitation-only workshop in January of this year designed by APSF to map out a strategy for definitive action to decrease patient injuries from OR anesthesia medication errors. “Technological intensification” and technology training (or the lack of it) for anesthesia professionals faced with an ever-more-complex array of machines, monitors, pumps, and adjunct devices has been a major topic. The danger of decreased cerebral perfusion pressure in “head-up” cases such as shoulder surgery in the “beach-chair” position (billed as “How low can you go?”) attracted a great deal of attention and interest. The importance and acuity of this topic led to a special Newsletter editorial by a Mayo Clinic world-class neuroanesthesia expert entitled “Cerebral Perfusion: Err on the Side of Caution.” Further, the APSF has recently funded a new case registry, Neurologic Injury after Non-Supine Shoulder Surgery (NINSS) (modeled after the ASA Postoperative Visual Loss Registry) to compile and analyze cases of severe neurologic injury occurring after surgery in the beach chair position and develop recommendations to help prevent them.
Copious Concerns
Beyond those already mentioned, the list of other initiatives and projects undertaken by the APSF during its quarter century is long and varied. A partial accounting of additional APSF themes over the years includes action on the patient safety implications of
- Reuse and attempted resterilization of disposable equipment
- Outdated anesthesia machines without modern safety features
- Evolution of the practice standards of the World Federated Societies of Anesthesiologists
- OR crisis management, including team work, team training, and resource management
- “Production pressure” causing dangerous omissions and corner cutting
- IV procedural sedation by non-anesthesia personnel
- Contamination of medical gasses and disruption of pipeline flow (including a dramatic travelling exhibit created by Ervin Moss, MD)
- Contamination of IV medications, such as the original propofol
- Office-based anesthesia special risks
- Obstructive sleep apnea patients and their postoperative care
- Postoperative cognitive dysfunction (particularly in the elderly)
- Possible long-term increase in morbidity and mortality after extensive general anesthesia
- Postoperative vision loss, especially in extensive prone spine surgery
- Wrong-site surgery
- Residual neuromuscular blockade and postoperative complications
- Failure to activate audible alarms on anesthesia machines and monitors
- An update of the “adverse event protocol”
- Persistence of deaths from malignant hyperthermia
- Dangers and challenges in patients with coronary artery stents
- An update of the anesthesia machine checkout protocol
- Possible impact of anesthesia management on cancer recurrence
- Persistence of OR fires—leading to production with ECRI of the recent “Fire Safety Video” that is now readily available and has been enthusiastically received and praised.
On the other hand, it is undeniable that certain APSF initiatives, however enthusiastically launched at the time, did not come to the full fruition that was originally hoped within the APSF. In most of these instances, the projects were extremely ambitious, involving proposed profession-wide, resource-intense behavior modifications that proved to be beyond the sphere of the very influential but still comparatively small APSF. Included in that group would be the plan to devise, establish, and promulgate a uniform patient safety curriculum, continuously updated, that would be taught in every anesthesiology residency and CRNA training program in the U.S. Another example would be the heavily promoted proposed universal adoption of electronic automated anesthesia information management systems. Likewise, the transformation of all surgical suites into “high reliability organizations” (analogous to the extraordinary coordination, efficiency, teamwork, and safety of the deck of a massive aircraft carrier) is a laudable and very logical goal that was featured prominently for some time by the APSF until it ran into the predictable resource limitations and entrenched cultures. Another topic that still proves difficult to tackle was the desire to try to organize thoughts and then proposed protocols to help deal with the realities of aging (or impaired) anesthesia professionals who might themselves create threats to patient safety. Finally, one of the significant concepts that has been debated, mostly within the APSF, throughout the history of the organization and without resolution is the desire for a genuine incident reporting network coordinated by the APSF, the originator of many of the relevant ideas. It has always been proposed that in addition to gathering and analyzing anonymous legally protected information about anesthesia adverse events and generating insightful recommendations, there would also be a rapid-response accident investigation team of highly experienced anesthesiologists and human factors researchers that could be activated in hours and flown immediately to the facility where a catastrophic anesthesia accident has occurred. This team, analogous to the one the NTSB sends to the scene of an airliner crash, would assist in or even direct the investigation of the anesthesia catastrophe—with complete dissociation and protection from the regulatory and medical-legal processes. Of course, the still-largely-volunteer APSF has not had the resources in time or finances to even begin to overcome the automatic strong resistance from multiple quarters to such a proposal. So, to quote a popular organizational mantra: “We’re still working on that.”
Research Renaissance
 Prior to APSF initiating it, there was no research funding specifically for patient safety. As noted, sponsorship and promotion of research on anesthesia patient safety has remained from the outset one of the top APSF priorities, consuming the large majority of the APSF budget and a great deal of time by its dedicated volunteer reviewers on the Scientific Evaluation Committee. In recent years, significant increases in research grant funding have been made possible by donor contributions of funds targeted for research support. In the current cycle, the maximum possible grant award stands at $150,000, a dramatic increase (more than double the rate of inflation) from the original 1986 award. The ASA funds 2 full grants. The review committee designates which funding source is matched with which approved grant based on the subjects involved. Various corporate and organization donors have contributed funds specifically for research grants and these donors are named in the Winter issue of the Newsletter. (Note that all corporate, group, and individual donors are listed in every issue of the Newsletter and those contributions all help fund the regular APSF-sourced research grants.) For the years 2008 (9 grants) and 2009 (6 grants), research support by the APSF reached its peak to date with total awards of approximately $1 million in funding for each of those years. The downturn in the economy did reduce contributions and, for 2010, there were 5 grants totaling nearly $670,000.
Prior to APSF initiating it, there was no research funding specifically for patient safety. As noted, sponsorship and promotion of research on anesthesia patient safety has remained from the outset one of the top APSF priorities, consuming the large majority of the APSF budget and a great deal of time by its dedicated volunteer reviewers on the Scientific Evaluation Committee. In recent years, significant increases in research grant funding have been made possible by donor contributions of funds targeted for research support. In the current cycle, the maximum possible grant award stands at $150,000, a dramatic increase (more than double the rate of inflation) from the original 1986 award. The ASA funds 2 full grants. The review committee designates which funding source is matched with which approved grant based on the subjects involved. Various corporate and organization donors have contributed funds specifically for research grants and these donors are named in the Winter issue of the Newsletter. (Note that all corporate, group, and individual donors are listed in every issue of the Newsletter and those contributions all help fund the regular APSF-sourced research grants.) For the years 2008 (9 grants) and 2009 (6 grants), research support by the APSF reached its peak to date with total awards of approximately $1 million in funding for each of those years. The downturn in the economy did reduce contributions and, for 2010, there were 5 grants totaling nearly $670,000.

Overall, the spectrum of research topics—funded because of their potential positive impact on safety—is vast and fascinating. A mere sampling of recent projects funded includes: “Obstructive Sleep Apnea and Adverse Perioperative Outcomes,” “Pathophysiology of Postoperative Delirium,” “Supplemental Oxygen: A Reduction in Pulse Oximetry Sensitivity, or an Increased Margin of Safety?,” “Patients after Minor Surgery with Monitored Anesthesia Care: Is It Safe to Drive?,” “Evaluation of an Anatomically Guided, Logically Formulated Airway Measure to Predict Difficult Intubations,” “Facilitating Patient Safety through Resident Hand-off Training,” “User Interface to Prevent Intravenous Infusion Pump Errors,” “Educational Value of an Adjustable and Life-Like Laryngoscopy Simulator,” “Challenging Others in the Operating Room: Testing an Educational Patient Safety Initiative for Anesthesia Faculty,” and “Virtual Anesthesia: An Online Simulation of Intraoperative Hemodynamic Management in Major Surgical Procedures.”
Structural Scaffolding
 As the APSF took hold in the early 1990s, it began to outstrip its ability to get things done with a 100% volunteer organization. Dr. Pierce was doing things out of the base of his private practice anesthesia group and was clearly stretched. It was a great fortune that Dr. Siker was stepping down as chair of his department in Pittsburgh. Recognized as one of ASA’s most effective past presidents, Dr. Siker was a perfect match for what APSF needed. He graciously took on the new role of Executive Director and formed an effective administrative office, with the compensation of a small fraction relative to the value of the dedicated effort he gave. Later, as Dr. Pierce and Dr. Siker were preparing for retirement, the APSF struck gold again, and Robert K. Stoelting, MD, took on the job of part-time president. Dr. Pierce stepped into the Executive Director role for a few years to make an effective transition. When Dr. Pierce fully retired in 2003, the APSF reorganized to reflect its new needs, and Dr. Stoelting became the full-time president and 2 executive vice president positions were established to expand APSF capabilities, initiatives, and infrastructure. Mr. George A. Schapiro and Dr. Cooper currently occupy those positions and bolster the managerial team with APSF Vice President Mr. Nassib G. Chamoun. Matthew B. Weinger, MD, recently took over the position of secretary of the APSF from Dr. Gaba. He continues the high standards set by his predecessor in keeping detailed, accurate accounts of the Executive Committee deliberations. The Executive Committee has turned over almost completely since 1985 (only Dr. Cooper remains of the original 1986 seven). What is so remarkable is that without exception, each new member has brought new vitality and ideas while maintaining the collegiality that permits lively debate and disagreement over issues of importance to serving the APSF mission. The organization remains lean and highly leveraged, persistently and remarkably effective for a national group with its size and its budget (which is ably managed by long-time APSF Treasurer Dr. Casey D. Blitt).
As the APSF took hold in the early 1990s, it began to outstrip its ability to get things done with a 100% volunteer organization. Dr. Pierce was doing things out of the base of his private practice anesthesia group and was clearly stretched. It was a great fortune that Dr. Siker was stepping down as chair of his department in Pittsburgh. Recognized as one of ASA’s most effective past presidents, Dr. Siker was a perfect match for what APSF needed. He graciously took on the new role of Executive Director and formed an effective administrative office, with the compensation of a small fraction relative to the value of the dedicated effort he gave. Later, as Dr. Pierce and Dr. Siker were preparing for retirement, the APSF struck gold again, and Robert K. Stoelting, MD, took on the job of part-time president. Dr. Pierce stepped into the Executive Director role for a few years to make an effective transition. When Dr. Pierce fully retired in 2003, the APSF reorganized to reflect its new needs, and Dr. Stoelting became the full-time president and 2 executive vice president positions were established to expand APSF capabilities, initiatives, and infrastructure. Mr. George A. Schapiro and Dr. Cooper currently occupy those positions and bolster the managerial team with APSF Vice President Mr. Nassib G. Chamoun. Matthew B. Weinger, MD, recently took over the position of secretary of the APSF from Dr. Gaba. He continues the high standards set by his predecessor in keeping detailed, accurate accounts of the Executive Committee deliberations. The Executive Committee has turned over almost completely since 1985 (only Dr. Cooper remains of the original 1986 seven). What is so remarkable is that without exception, each new member has brought new vitality and ideas while maintaining the collegiality that permits lively debate and disagreement over issues of importance to serving the APSF mission. The organization remains lean and highly leveraged, persistently and remarkably effective for a national group with its size and its budget (which is ably managed by long-time APSF Treasurer Dr. Casey D. Blitt).
Reflections and Conclusion
As in the past, future successes in safety will often result from the desire to do the “right thing because it makes sense.” This approach is based on sound principles, technical theory, experience, and pursuit of real-life problems that have not been subjected to controlled experiments. This does not mean that evidence-based medicine should be ignored. Rather, this viewpoint recognizes that safety changes that impact extremely rare events may not lend themselves to traditional “randomized double blind studies with p<.05” to determine validity or efficacy.
Leape, Berwick, and Bates, nationally recognized leaders in patient safety, commended the profession of anesthesia as ‘the only system in health care that begins to approach the vaunted “six sigma” level of perfection’ in their seminal 2002 JAMA article “What Practices Will Most Improve Safety?”5 They noted that achievement of improved anesthesia patient safety cannot be attributed to any single practice or development of new anesthetic drugs or any technologic advance, but rather to application of a broad array of changes in process (including behavior), equipment and technology, resources, organizations, supervision, training, teamwork, and even practitioner personalities. No single one of these changes has ever been “proven” to have a clear-cut impact on morbidity and mortality outcome. Rather, anesthesia safety has been dramatically improved by applying an entire collective host of changes that made sense in all these areas. Anesthesia patient safety in the past and in the future “is doing a lot of little things that in the aggregate make a big difference.”5 The APSF has led the way in this regard at many junctures over the last quarter century.
One observation by the original visionary, Dr. “Jeep” Pierce, was: “Patient safety is not a fad. It is not a preoccupation of the past. It is not an objective that has been fulfilled or a reflection of a problem that has been solved. Patient safety is an ongoing necessity. It must be sustained by research, training, and daily application in the workplace. I fear that we may be entering an era that could easily undo many of the gains that we cherish so highly. This is the era of cost-containment, production-pressure, and bottom-line decision-making by corporate deal-makers. The forces underlying this new era are driving us to be leaner, faster, and cheaper. To some extent, these changes may bring a measure of immediate health and vigor to the practice of medicine; they also pose a worrisome threat. If we try to meet financial challenges by short-cutting our daily attention to patient safety or by minimizing our long-term commitments to education and research, we may not be able to carry forward the gains of the immediate past or pursue the exciting insights and innovations that are just emerging. . . . Patient safety is truly the framework of modern anesthetic practice, and we must redouble efforts to keep it strong and growing.”1
The work of improving anesthesia patient safety is by no means done. Systems, organizations, and equipment still at times fail and, also, basic preventable human errors still do sometimes occur. Further, as noted, increasing “production pressure” in anesthesia practice from expanding clinical demands in the face of diminishing resources may threaten previously won gains. The anesthesia profession as a whole must consider and address this danger. The APSF continues to work hard both on established tenets and new safety principles. It serves as a model of the pioneering successful collaboration and commitment of the entire constellation of anesthesia-related professions and groups to the common goal of optimal patient safety. Very proud of its precedent-setting contributions and accomplishments, the APSF persists vigorously in pursuit of its mission “that no patient shall be harmed by anesthesia.”
Happy 25th Anniversary, APSF! Many, many more.

Acknowledgments
Source material for this retrospective included the minutes of the APSF Executive Committee back to 1985 and each Newsletter issue since Volume 1, Number 1 in March 1986, as well as fond memories from some of those named above and occasional borrowing from excellent prior accounts written by Drs. E.S. “Rick” Siker, Ellison C.“Jeep” Pierce, Jr., Jeffrey B. Cooper, and Robert K. Stoelting. Special great thanks to Dr. Cooper for his thoughtful review and editing.
References
- Pierce EC, Jr. The 34th Rovenstine Lecture: 40 years behind the mask: safety revisited. Anesthesiology 1996;84:965-975.
- Cooper JB. Patient safety and biomedical engineering. In: Kitz RJ (Editor). This is no humbug: reminiscences of the Department of Anesthesia at the Massachusetts General Hospital. Boston: Department of Anesthesia and Critical Care, Massachusetts General Hospital; 2002. p. 377-420.
- Gaba DM, Howard SK, Fish K, et al. Simulation-based training in anesthesia crisis resource management (ACRM): A decade of experience. Simulation & Gaming 2001;32:175-193.
- Eichhorn JH. Anesthesia patient safety: a modern history. Boston: Anesthesia Patient Safety Foundation; 1995.
- Leape LL, Berwick DM, Bates DW. What practices will most improve safety? Evidence-based medicine meets patient safety. JAMA 2002;288:501-507.


 Issue PDF
Issue PDF