| Editor’s Note: For more information on the safe implementation and use of smart pumps the following link provides the most current ISMP guidelines on this topic. ISMP Guidelines for Optimizing Safe Implementation and Use of Smart Infusion Pumps: https://www.ismp.org/node/13744/ |
Introduction
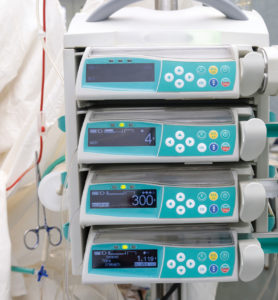 Medication errors are a leading cause of patient harm in hospitals and operating rooms. Greater than 50% of medication errors that lead to patient injury occur during the medication administration phase.1 Historically, medication infusion devices served simply as a mechanical device to infuse medications intravenously. The advent of smart infusion pumps allowed for clinical decision support tools to be integrated into the medication administration process. This decision support in smart infusion pumps includes minimum and maximum alerts for dose, concentration, duration, and rate alerts and is part of the dose error reduction software (DERS) that exists in the majority of infusion pumps on the market today. This decision support can prevent misprogramming of pumps or keystroke errors (examples of this type of error would be programming 55 mg instead of 5 mg).
Medication errors are a leading cause of patient harm in hospitals and operating rooms. Greater than 50% of medication errors that lead to patient injury occur during the medication administration phase.1 Historically, medication infusion devices served simply as a mechanical device to infuse medications intravenously. The advent of smart infusion pumps allowed for clinical decision support tools to be integrated into the medication administration process. This decision support in smart infusion pumps includes minimum and maximum alerts for dose, concentration, duration, and rate alerts and is part of the dose error reduction software (DERS) that exists in the majority of infusion pumps on the market today. This decision support can prevent misprogramming of pumps or keystroke errors (examples of this type of error would be programming 55 mg instead of 5 mg).
Smart pumps with drug libraries have increasingly gained adoption in acute care patient settings including the perioperative area. A survey completed in 2017 by the American Society of Health System Pharmacists (ASHP) identified that 88.1% of hospitals have adopted smart infusion pumps. This was a substantial increase from 2005 when only 35% of hospitals reported using smart infusion pumps.2
In 2010, over 100 stakeholders were invited to attend an ASPF-sponsored medication safety conference to develop new strategies for improving medication safety in the operating room. The output of that meeting was a paradigm that focused on Standardization, Technology, Pharmacy/Prefilled/Premixed, and Culture (STPC). Key recommendations from this meeting involved: 1) ensuring that all medication and fluid infusions are administered via a smart infusion device; and 2) facilitation of adequate training and improved standardization of smart infusion pumps.3 A subsequent 2018 APSF Stoelting Conference on medication safety recommended developing consensus between professional and patient safety organizations on standardization of drug concentrations used in infusion administration.4
Challenges and Barriers to Successful Use of Smart Pumps
There are a variety of challenges and barriers to achieving 100% adoption of smart infusion pumps.5 These challenges include:
- Usability and workflow barriers—Not using the smart infusion pumps or using them incorrectly diminishes their value in reducing medication administration errors. Virtually all infusion pumps in the acute care setting now contain DERS. They also contain the ability to bypass this decision support. Key contributors to noncompliance include outdated interfaces and the ability to easily opt out of the DERS programming.5 Understanding the barriers to compliance with DERS use is the most vital step when evaluating the impact of smart infusion pumps in any organization.
- Building and maintaining custom drug libraries—The drug library which comprises the limits in DERS often need to be created from scratch. This library includes which medications are included as well as the safety alert thresholds for dose, concentration, and duration/rate alerting. The process to build these libraries is time-consuming and resource-intensive. Unfortunately, this resource-intensive process of building a drug library is just the first step. Maintaining and updating this content is of vital importance to achieve optimal results from this technology and if not completed can be an impediment of full smart pump adoption.
- Alarm/Alert fatigue—Smart infusion pumps are no different than any other health care technologies in that excessive alerts/alarms can lead to health care provider alarm or alert fatigue.6–8
Interventions to Overcome Barriers to Smart Pump Adoption
In 2010, the APSF Newsletter reported on a large health system’s implementation of smart infusion pumps. Using the paradigm of STPC described above, Wake Forest University Baptist Medical Center was able to successfully standardize infusion-related practices across multiple patient care areas including the operating room. Key interventions leading to success in this implementation included: 1) Multidisciplinary engagement incorporating pharmacy, nursing, intensive care providers, and anesthesia professionals; 2) A focus on standardization of all IV medications concentrations, dosing units, and adoption of smart pump technology across the continuum of care in the organization; and 3) An emphasis on training staff to ensure there was an understanding of the capabilities and limitations of the infusion devices.9
How intelligent are Smart infusion pumps in your organization?
Infusion pumps collect information ranging from discrete keystroke data to information regarding clinicians’ responses to alerts. This data is frequently communicated wirelessly to a central server. However, this data can be challenging to access and interpret and is often underutilized by clinicians that are responsible for the oversight of these devices. The Institute for Safe Medication Practices (ISMP) completed a survey in 2018 to learn about the current utilization of smart pump data analytics. This survey included responses from pharmacists and nurses at 126 hospitals and concluded that 96% of respondents believe that using data from smart infusion pumps was vital to driving quality improvement. However, only 22% of respondents felt that their organization had the correct resources and skills to capture meaningful and actionable insights from this data. ISMP recommended that organizations utilize external resources, such as data companies or infusion pump manufacturers, to assist with data evaluation when needed.10
What information is captured in infusion devices?
Conventional Data Evaluation and Compliance with DERS
When clinicians program infusion pumps, they are presented with a choice to either use the DERS or use a “no drug selected” or “basic infusion” mode. When DERS is not utilized, clinicians remove all clinical decision support and safety limits from the process. Most infusion pump devices provide data on the percentage of infusions using the DERS. Clinicians may not realize how often programming errors occur and how often DERS is bypassed. It is vitally important to share this data with frontline clinicians to provide an adequate feedback loop to support continuous quality improvement.
Alert and Alarm Data
Alert fatigue and subsequent severe adverse events have been associated with smart infusion pump use.6–8 Alert fatigue is characterized by clinician desensitization to alerts or alarms which can lead to missed clinical alerts, delayed assessment of patients and the potential for serious patient harm.11,12 This desensitization occurs due to presence of clinically meaningless or nuisance alerts.13
Infusion pump logs capture each alert and the clinician’s response to facilitate alert management to reduce fatigue. Infusion pump associated clinical alerts can include minimum and maximum alerts for dose, concentration, and duration or rate alerts. Clinician responses can include overriding an alert and proceeding, cancelling the infusions and preprogramming as a basic infusion, or altering the infusion parameters to be within the alert limits. Assessing alert data has value to understand if alert fatigue exists, if limits need adjusting, or if there are potential unsafe practices surrounding specific medications.
Medication Practice Standardization
In 2015, ASHP initiated their Standardize 4 Safety campaign.14 This was the first national, interprofessional effort to help reduce the incidence of medication errors by standardizing medication concentrations. Access and understanding of infusion device data can provide details that can facilitate this standardization. This data includes the following elements of medication administration: 1) the overall usage of specific agents; 2) the location where these medications are administered; 3) the dose and concentrations that were commonly used; and 4) the total volume administered. For example, analysis of infusion pump data might reveal commonly used medications in anesthesia care areas and their concentrations. Having insight into these practices can play a significant role in achieving standardization. Standardizing concentrations and dosing units between anesthesia and inpatient units is a critical element of medication safety as this might reduce the risk of a medication error when a patient transitions from one care area to another (Figure 1).
Figure 1: Smart Pump Considerations for Anesthesia Professionals
|
Novel Data Evaluation
Infusion pump data describes the total volume of an infusion administered to a patient and may serve to right-size dispensed amounts. For example, if Drug X is dispensed to a procedural area from the pharmacy or an automated dispensing cabinet in 100 mL, how do we know how much of this drug was administered? Traditionally, clinicians have been left to manually examine OR and EHR records to extract this information. However, the data from the infusion devices may provide an additional or more precise measurement of how much medication was administered.
Narcotic Diversion Mitigation
The impact of opioid diversion from health care facilities has been widely documented, but vulnerabilities in monitoring the use of controlled substances still exist.15 ASHP currently recommends implementing a surveillance program, which effectively monitors data from medication technologies in high-risk areas such as the OR.16 Understanding how much drug is dispensed versus how much is administered to a patient can be vital to a narcotic diversion monitoring program. For example, if fentanyl is dispensed in a 2500 mcg/250 mL bag, the infusion pump data records the exact amount of drug administered. The unused medication could potentially be diverted and must be accounted for as wasted. Controlled substance diversion monitoring can compare the dispensed volume with the administered and the wasted volumes to monitor for possible diversion. Minimizing opioid dispensing has been associated with a reduction in opioid-related complications in other patient care settings.17–19
Drug Shortage
Drug shortages have unpredictable onsets and have become a national patient safety crisis. From 2010 to 2018, there were almost 1500 new shortages reported. Up to 63% of these shortages are related to injectable medications.20 Drug shortages potentially force clinicians to use less familiar alternatives that may impact patient safety. Infusion pump data analysis might provide a more precise measurement of what drugs patients are being administered and amounts that are actually wasted which might aid in conserving the drug supply during a national shortage.
Conclusions
Smart infusion pump use has been shown to reduce patient harm from injectable medications, but safety features must be utilized to realize the full benefits of the technology. Health care organizations might seek additional ways to optimize use of this technology including the management of dispensed container volumes, opioid diversion, and drug shortage management. A multidisciplinary effort to build effective anesthesia drug libraries, standardize infusions, and engage in a process of ongoing data analysis will maximize the effectiveness of the devices and reduce the probability of medication errors.
Tim Vanderveen, PharmD, MS is a consultant to ICU Medical. He is a past member of the APSF Board of Directors and is a member of the APSF Committee on Technology. He was previously vice president, Center for Safety and Clinical Excellence for Becton Dickinson, and is a current shareholder.
Dr. O’Neill is the co-founder and chief clinical officer at Bainbridge Health. He is a current shareholder of Bainbridge Health.
Dr. Beard is medical director and shareholder of ICU Medical and a member of the APSF Editorial Board.
References
- Leape LL, Bates DM, Cullen DJ, et al. Systems analysis of adverse drug events. JAMA. 1995;274:35–43.
- Schneider PJ, Pedersen CA, Scheckelhoff DJ. ASHP national survey of pharmacy practice in hospital settings: dispensing and administration—2017. AJHP. 2018;75:1203–1226.
- Eichhorn, JH. APSF hosts medication safety conference. APSF Newsletter. 2010;25:1–20. https://www.apsf.org/article/apsf-hosts-medication-safety-conference/ Accessed November 4, 2019.
- Recommendations of the four work groups at the 2018 APSF Stoelting conference on medication safety. APSF https://www.apsf.org/medication-safety-recommendations/. Accessed November 6, 2019.
- Giuliano KK, Ruppel H. Are smart pumps smart enough? Nursing. 2017;47:64–66.
- Cho OM, Kim H, Lee YW, et al. Clinical alarms in intensive care units: perceived obstacles of alarm management and alarm fatigue in nurses. Health Inform Res. 2016;22:46–53.
- Tran M, Ciarkowski S, Wagner D, et al. A case study of the safety impact of implementing smart patient controlled analgesic pumps at a tertiary care academic medical center. J Qual Patient Saf. 2012;38:112–119.
- Manrique-Rodriquez S, Sanchez-Galindo A, Fernandez-Llamazares CM, et al. Smart pump alerts: all that glitters is not gold. Int J Med Inform. 2012;81:344–350.
- Vanderveen T, Graver S, Noped J, et al. Successful implementation of the new paradigm for medication safety: standardization, technology, pharmacy, and culture (STPC). APSF Newsletter. 2010;25:26-28. https://www.apsf.org/article/successful-implementation-of-the-new-paradigm-for-medication-safety-standardization-technology-pharmacy-and-culture-stpc/ Accessed December 23, 2019.
- Smetzer J, Cohen M, Shastay A, et al. Survey results: smart pump data analytics. Acute Care ISMP Medication Safety Alert. 2018;23:1–4.
- ECRI Institute. Top 10 health technology hazards for 2014. Health Devices. 2013;42:1–3.
- Joint Commission on Accreditation of Healthcare Organizations. The Joint Commission announces 2014 patient safety goal. Jt Comm Perspect. 2013;33:1–4.
- Agency for Healthcare Research and Quality. Alert fatigue. https://psnet.ahrq.gov/primer/alert-fatigue. Accessed November 4, 2019.
- American Society of Health Systems Pharmacists. Standardize 4 Safety Initiative. https://www.ashp.org/pharmacy-practice/standardize-4-safety-initiative. Accessed November 4, 2019.
- Fan M, Tscheng D, Hamilton M, et al. Diversion of controlled drugs in hospitals: a scoping review of contributors and safequards. J Hosp Med. 2019;14:419–441:28.
- Brummond PW, Chen DF, Churchill W, et al. ASHP guidelines on preventing diversion of controlled substances. AJHP. 2017;74:325–348.
- Chen X, Ma Q, Barron J. Effect of controlled substance use management on prescribing patterns and health outcomes among high-risk users. J Manag Care Spec Pharm. 2019;25:392–401.
- Bohert AS, Valenstein M, Bair MJ. Association between opioid prescribing patterns and opioid overdose-related deaths. JAMA. 2011;305:1315–1321.
- Groenewald CB, Zhou C, Palermo TM, Van Cleve WC. Associations between opioid prescribing patterns and overdose among privately insured adolescents. Pediatrics. 2019; 144:e20184070.
- American Society of Health Systems Pharmacists. Drug shortages. Drug shortage statistics. https://www.ashp.org/Drug-Shortages/Shortage-Resources/Drug-Shortages-Statistics. Accessed November 4, 2019.


 Issue PDF
Issue PDF