Economic realities of health care reimbursement and growing consumer demand have shifted health care delivery: from in-hospital to outpatient settings, and recently to physicians’ offices. The number of offices, patients, variety, and complexity of procedures continues to increase with 12 million office-based procedures performed in 2009. This is due to decreased cost and improved provider patient access and convenience, without regulations similar to those at hospitals or ASCs (Ambulatory Surgical Centers) Office personnel often are not prepared for complications. An increased incidence of adverse events in office-based surgery has caught the public’s attention due to highly publicized fatalities, such as the death of Kanye West’s mother and of young, healthy patients undergoing routine procedures.
Currently, only 23 U.S. states have some regulation for office-based surgery. In addition, a vast majority of offices lack accreditation by one of the major accrediting agencies (AAAHC, AAAASF, JCAHO). Whether such procedures are performed with or without an anesthesia care team provider, current issues include patient and procedure selection, perioperative management, complications, and recovery. Non-patient related issues include proceduralists performing outside their scope of practice, substandard facilities, and lack of qualified office personnel. As of 2001, the ASA Closed Claims analysis has only 37 office-based cases, due to a 3-5 year lag between occurrence and entry into the database. One study showed that office-based claims were 3-times higher in severity (67% vs. 21% deaths), and in a higher proportion and amount of payment compared to ASCs. Further, 46% of office claims (vs. 13% for ASCs) were deemed preventable by better monitoring—e.g., by pulse oximetry in the postoperative setting.1
A controversial study by Vila et al. found a 10-fold increase in adverse incident and death in the office compared to the ASC setting in Florida.2 A retrospective review by Keyes et al. examined 1.1 million accredited office cases and recorded 23 deaths.3 Thirteen deaths were due to pulmonary embolism. The number of offices involved in this study represents a small fraction of office-based surgery practice, because the majority of offices are unaccredited. A Society for Ambulatory Anesthesia newsletter highlighted the need for better office education of surgeons, proceduralists, nurses, legislators and the public.4 In addition, OBS practices face increased pressure by “medical necessity” policies instituted by commercial insurers.
What’s the best way to improve patient safety in this “Wild West of Healthcare?” A recent editorial in the New England Journal of Medicine pointed out that, according to the Agency for Healthcare Research and Quality, only 10% of patient safety studies have been performed in outpatient settings. The authors called for “creating a culture of safety,” acknowledging that safety oversight of office-based surgery is often “fragmented and disorganized and lacking in clear leadership.”5
Over the past decade, several professional organizations such as the ASA and ASPS (American Society of Plastic Surgeons) have generated recommendations and guidelines to improve office safety. In addition, anesthesiologists are leading in their attempts to collect ambulatory outcomes data through the Society for Ambulatory Anesthesia SCOR database and the Anesthesia Quality Institute to develop the National Anesthesia Clinical Outcomes Registry (NACOR).
As a result of concerns for patient safety, a few dedicated physicians representing different specialties came together to form The Institute for Safety in Office-Based Surgery (ISOBS), a Boston-based, independent, 501(c)(3) non-profit organization. The Institute’s mission is “to promote patient safety in office-based surgery and to encourage collaboration, scholarship, and physician and patient education.” The ISOBS is an organization of individuals from diverse professional backgrounds. The idea is to have an entity endorsed by, and affiliated with, a range of anesthesia and non-anesthesia professional organizations. With leadership drawn from several specialties, the ISOBS would seek to engage these groups with the common goal of building consensus for best practices and defining uniform regulation, rather than having individual, uncoordinated efforts, or externally imposed regulations. In addition, the ISOBS wants to help patients learn about safe OBS practices and to obtain the tools needed to understand their health care provider’s and facility’s credentials. Thus, patient education is a large part of its mission.
The ISOBS was recently interviewed by the Wall Street Journal and a few other national newspapers, discussing the current issues facing office practices.6,7 Less than 2 years after inception, the ISOBS recruited an excellent team of experts representing various medical, surgical, and dental specialties, in addition to board members from the business, law, and public policy sectors. The ISOBS plans to provide opportunities for safety training through a variety of tailored online educational modules: to enable office personnel to assess mastery of core safety competencies and to develop a “Certificate Program” for office practices that have successfully completed this educational process.
The ISOBS hopes to serve as a knowledge resource for patients and health care providers, detect educational gaps of the medical personnel involved in patient care, and encourage outcomes research and adverse event reporting. This is particularly timely given recently updated CMS guidelines that reflect future changes in cost and reimbursement of healthcare. In 2010, the Institute sponsored a CME course at Harvard Medical School, “Anesthesia in the Office-Based Setting: Safe, Simple, and Pain Free,” followed by an inaugural reception to honor pioneers in patient safety, Drs. Ellison “Jeep” Pierce and Jeffrey B. Cooper (see photo).

ISOBS honors pioneers in patient safety at 2010 inaugural reception: Left to right, front row: honorees Jeffrey Cooper, PhD, Ellison “Jeep” Pierce, Jr, MD.; back row: Fred E. Shapiro, DO, president and founder, Richard D. Urman, MD, MBA, chief executive officer.
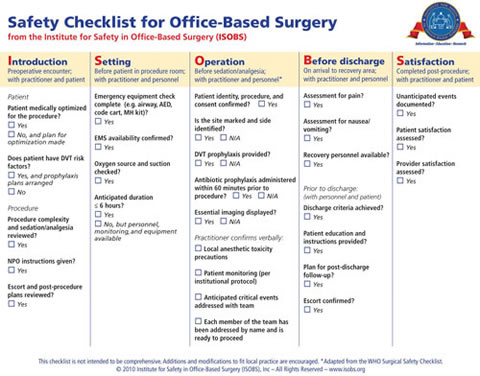
The ISOBS has developed an OBS surgical safety checklist (see Figure).8 Recent studies have shown that checklists can reduce costs, complications, and mortality, and improve patient safety and quality of care.9,10 We hope to find the same results for the office.
The ISOBS will organize patient safety symposia at subspecialty meetings, to generate discussion regarding providers administering deep sedation and utilizing ASA outcome data collection systems.
The ISOBS has caught the attention of the Institute for Healthcare Improvement, the Massachusetts Medical Society, the Massachusetts Coalition for Prevention of Medical Error, Massachusetts Board of Registration, as well as national malpractice and health care organizations.
For additional information, visit www.ISOBS.org.
Richard D. Urman, MD, MBA, is an Assistant Professor of Anesthesia at Harvard Medical School, Director of Procedural Sedation Management at Brigham and Women’s Hospital, and Chief Executive Officer for the Institute for Safety in Office-Based Surgery, Boston, MA.
Fred E. Shapiro, DO, is an Assistant Professor of Anesthesia at Harvard Medical School, President of the Massachusetts Society of Anesthesiologists, and President and Founder of the Institute for Safety in Office-Based Surgery, Boston, MA.
References
- Domino KB. Office-based anesthesia: lessons learned from the Closed Claims Project. ASA Newsletter 2001;65(6):9-11, 15.
- Vila H Jr, Soto R, Cantor AB, Mackey D. Comparative outcomes analysis of procedures performed in physician offices and ambulatory surgery centers. Arch Surg 2003;138:991-5.
- Keyes GR, Singer R, Iverson RE, et al. Mortality in outpatient surgery. Plast Reconstr Surg 2008;122:245-50.
- Ahmad S. Office based—is my anesthetic care any different? Assessment and management. Anesthesiol Clin 2010;28:369-84.
- Gandhi TK, Lee TH. Patient safety beyond the hospital. N Engl J Med 2010;363:1001-6.
- Landro L. “Taming the Wild West of Outpatient Surgery—Doctors’ Offices. Wall Street Journal. October 26, 2010. Available at: http://blogs.wsj.com/health/2010/10/26/taming-the-wild-west-of-outpatient-surgery-doctors-offices/. Accessed April 11, 2011.
- Midey C. “Doctor’s Offices Doing More Surgeries.” Arizona Republic. November 7, 2010. Available at: http://www.azcentral.com/arizonarepublic/news/articles/2010/11/07/20101107doctors-office-surgery.html. Accessed April 11, 2011.
- Safety Checklist for Office-Based Surgery. Developed by the Institute for Safety in Office-Based Surgery with contributions by Alex Arriaga, MD, Richard Urman, MD, MBA, and Fred Shapiro, DO, 2010.
- de Vries EN, Prins HA, Crolla RM, et al. Effect of a comprehensive surgical safety system on patient outcomes. N Engl J Med 2010;363:1928-37.
- Semel ME, Resch S, Haynes AB, et al. Adopting a surgical safety checklist could save money and improve the quality of care in U.S. hospitals. Health Aff (Millwood) 2010;29:1593-9.


 Issue PDF
Issue PDF