
![]() Dear Q&A,
Dear Q&A,
Suction in the operating rooms where I work seems inadequate for full stomach or bleeding airways. Are there any guidelines for anesthesia suction for emergency airways?
Lana Wanstreet West Frankfort, IL
![]() Dear Ms. Wanstreet,
Dear Ms. Wanstreet,
Suction plays a critical role in the delivery of anesthesia. There is surprisingly little information about what constitutes adequate suction. The International organization for Standardization (ISO), through ISO 10079-3:2014, specifies safety and performance requirements for medical suction equipment powered from a vacuum. It applies to equipment connected to medical gas pipeline systems and other apparatus. This standard quotes a minimum air flow of 20 liters/minute. All of the machines that were tested (n=5) had a mean flow at the Yankauer tip of 47.6 liters/minute.
Another standards body, the National Fire Protection Association (NFPA 99) states there must be 85 LPM flow of air at the wall with no tubing attached. In the operating rooms reported on here, the maximum flows obtained from the wall vacuum outlets were 114 liters/minute for Diamond fittings and 121 liters/minute for DISS fittings.
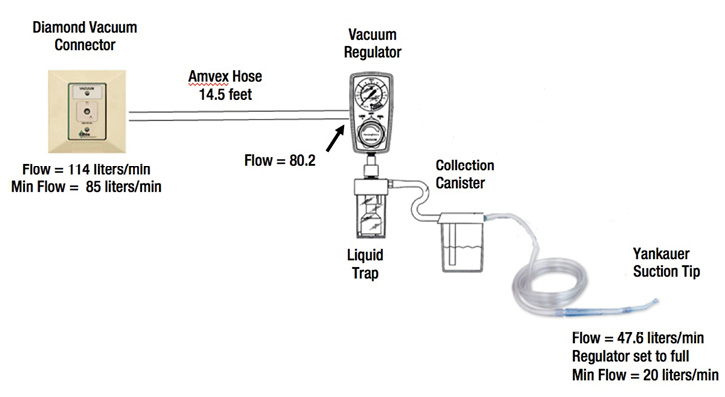
Figure 1. Suction system on several new anesthesia machines (General Electric [Aisys, Aespire, Aestiva] and from Dräger [Apollo, Fabius]) demonstrating demonstrating the step down in air flow from the wall to the tip of the Yankauer.
Unfortunately, the flow of air from the vacuum connector may not guarantee that there will be adequate negative pressure and flow to remove liquids through the comparatively high resistance of the Yankauer tip and the suction tubing.
Classically, in the anesthesia environment suction is assessed by permitting the clean suction tubing from the suction canister to attach to the palm or thumb of the hand. If the suction tubing remains attached to the palm or the thumb without assistance it is assumed to be adequate. Unfortunately, this assessment is really nothing more than a measure of the suction’s ability to support the weight of the suction tubing. Little suction pressure is required if there is a short unsupported length of tubing (tubing coiled on the surface of the anesthesia machine), but fairly high suction pressure is required to support the weight of the entire 6-foot length of tubing. The average weight of the Precision Medical (Northhampton, PA) 6-foot suction tubing was 100.58 grams.
The pressure at which the tubing attached to the palm or thumb (Pattach), and the pressure at which the tubing “let go” from the palm or thumb (Pletgo), was measured 5 times with or without latex gloves in 6 volunteers.
With the subject wearing gloves the pressure required to hold up the 6-foot length of tubing was -100.2 mmHg whereas the pressure required to hold the tubing without gloves was -95.2 mmHg. The average pressure for gloves and no gloves was -97.7 mmHg. Again, the pressure required to hold the tubing is a function of the weight of the tubing, and is unrelated to the suction flow. Remember that pressure is measured when the tubing is being supported by the suction pressure when there is no flow.

Figure 2. Flow of water compared to SAE 40 motor oil (simulating very thick mucous secretions) at different settings of the pressure regulator.
Figure 2 illustrates the flow of water obtained by different settings of the pressure regulator, and the flow of SAE 40 motor oil, which simulates very thick mucus secretions. Viscosity is the resistance to flow due to neighboring particles in a fluid, more commonly referred to as thickness, with water being the reference viscosity of 1 centipoise (cP) and blood of normal hematocrit being 3 to 6 times more viscous at 37° C (Table 1). The vertical line is drawn at the mean of the glove/no glove pressure of -97.7 mmHg. The flow through the Yankauer was 2.88 liters/minute with water. If the suction tubing on a gloved hand just supported the weight of the tubing at our average pressure, the Yankauer tip could remove 2.88 liters/minute of water, or only 60 ml/minute of a fluid with the viscosity of SAE 40 motor oil. With SAE 40 motor oil the flow was reduced to 60 ml/minute. The far right of the graph illustrates the maximum flow of water and oil with the regulator switched to full or maximum, which corresponds to an air flow at the Yankauer tip of 47.6 liters/minute. While the air provides 47.6 liters/minute of flow, that corresponds to only 3.93 liters/minute of water and less for more viscous fluids.
Table 1: Viscosity of various substances that may require suctioning during an anesthetic compared to the viscosity of SAE 40 motor oil.
Viscosity in cP at room temperature |
Reference |
|
| Viscosity of air | 0.081 cP | http://hyperphysics.phy-astr.gsu.edu/hbase/tables/viscosity.html |
| Viscosity of water | 1.0 cP | http://hyperphysics.phy-astr.gsu.edu/hbase/tables/viscosity.html |
| Viscosity of whole blood | 3.6 to 6.0 cP | http://ltd.aruplab.com/tests/pub/0020054 |
| Viscosity of gastric mucus | 75 to 230 cP | Reference 3 |
| Viscosity of SAE 40 motor oil | 650 to 900 cP | http://www.vp-scientific.com/Viscosity_Tables.htm |
| Viscosity of Sputum | 148 cP to 15,000 cP | References 4 and 5 |
Unfortunately, checking air flow out of the wall vacuum outlet is not a good indicator of how the suction system will handle watery secretions, blood, or thick mucus secretions. This study was performed using the common bulbous Yankauer suction in an attempt to demonstrate the factors that contribute to having adequate suction for anesthesia. The real issues are 1) how fast the stomach contents or other substances such as blood are entering the pharynx versus how fast (flow rate) can the suction system remove them, and 2) the ability of suction to remove the substances from the glottis in adequate time so as not to significantly prolong intubation. It is important to have a suction system set to Full or Maximum that can provide removal of 2 1/2 to 4 liters/minute of water. One hopes there will be no particulate matter to clog the Yankauer tip, or fluid that is too viscous to remove quickly.
Dr. Paulsen is chair of the APSF committee on technology and director of the anesthesiologist assistant program at Quinnipiac University, Hamden, CT.
References
- 1. International Organization for Standardization. Medical suction equipment — Part 3: Suction equipment powered from a vacuum or positive pressure gas source. ISO 10079-3:2014. Geneva, Switzerland.
- National Fire Protection Association. NFPA 99: Health care facilities code. Available at https://www.nfpa.org.
- Curt JRN, Pringle R. Viscosity of gastric mucus in duodenal ulceration. Gut 1969;10: 931-934.
- Picot R, Das I, Reid L. Pus, deoxyribonucleic acid, and sputum viscosity. Thorax 1978;33:235-242.
- Jenssen AO. Scanning of viscosity in sputum. Scand J Respir Dis 1976;57:31-36.
The APSF sometimes receives questions that are not suitable for the Dear SIRS column. This Q and A column allows the APSF to forward these questions to knowledgeable committee member or designated consultants. The information provided is for safety-related educational purposes only, and does not constitute medical or legal advice. Individual or group responses are only commentary, provided for purposes of education or discussion, and are neither statements of advice nor the opinions of the APSF. It is not the intention of the APSF to provide specific medical or legal advice or to endorse any specific views or recommendations in response to the inquiries posted. In no event shall the APSF be responsible or liable, directly or indirectly, for any damage or loss caused or alleged to be caused by or in connection with the reliance on any such information.


 Issue PDF
Issue PDF