
APSF panelists field questions from the audience at APSF Workshop on implementation of emergency manuals.
On Saturday, October 11, 2014, the APSF/ASA sponsored the Ellison C. Pierce, Jr., MD, Patient Safety Memorial Lecture at this year’s Annual ASA Meeting in New Orleans, LA. Dr. David M. Gaba presented the timely topic, Competence and Teamwork Are Not Enough: The Value of Cognitive Aids. Dr. Gaba is associate dean for Immersive and Simulation-Based Learning and professor of Anesthesia at Stanford University School of Medicine and co-director of the Simulation Center of Innovation at the VA Palo Alto Health Care System. It was particularly poignant that Dr. Gaba gave the EC Pierce Memorial Lecture as Jeep Pierce was a mentor and close friend of Dr. Gaba’s for many years. Dr. Gaba’s experience as an innovator and expert in the fields of simulation and crisis management made this a fantastic educational experience for the hundreds of attendees at this timely lecture. Dr. Gaba pointed out the aviation analogies for emergency manuals and cognitive aids used by pilots and challenged anesthesia professionals to embrace the use of and training about these important tools.

Dr. Stoelting (left) and Dr. Gaba enjoy the enthusiastic response to the E.C. Pierce, Jr., MD, Lecture and APSF Workshop.
Dr. Gaba presented examples of how emergency manuals could assist in the recognition, diagnosis, differential diagnosis, considerations, and critical treatment steps of perioperative emergencies. He also gave examples of pitfalls that may occur with cognitive aids and strategies to mitigate these pitfalls, noting that not all possible events are included in a manual, that some events happen too quickly to utilize a manual, and the need to recognize the tradeoff between completeness and usability. Dr. Gaba’s take home points for his lecture and the subsequent workshop included the following:
- Anesthesiologists, Nurse Anesthetists and Anesthesiologist Assistants need cognitive aids—especially “emergency manuals” or “emergency checklists” because our memory is limited and fallible especially under stress and about uncommon and unexpected events.
- Emergency manuals help us with both diagnosis (figuring out what is going on) and treatment (what to do once we know what is going on). Failures of both types have been documented in real patient care and in simulations.
- Well-developed manuals that have been extensively tested in simulation and in real patient care, are now available from multiple sources. Several such manuals are available for free. See www.emergencymanuals.org.
- Although there are a number of pitfalls to using cognitive aids, there are mitigating strategies available for all of them. The net benefit of using such aids very likely far outweighs the possible pitfalls and limitations.
Following Dr. Gaba’s lecture, the APSF sponsored the 2014 Board of Directors Workshop Competence and Teamwork Are Not Enough: Implementing Emergency Manuals and Checklists. Based upon the previous content presented in Dr. Gaba’s lecture, the workshop concentrated on the practical aspects of systematically implementing emergency manuals in perioperative settings. Experts on the development and production of emergency manuals gave guidance about key aspects of how to use emergency manuals with a focus on the process of implementation. The critical elements of implementation were discussed in introductory presentations, followed by a panel discussion and facilitated breakout groups. The sessions provided an interactive experience for attendees to learn about how to incorporate emergency manuals. The following objectives were intrinsic to the workshop:
- To be able to explain the value of emergency manuals to hospital leadership (anesthesia, surgery, nursing, administration)
- To be able to explain to others what is meant by each of the 4 elements to implementation of emergency manuals
- To know options for how to select a manual for their organization (adopt an existing one or create one de novo)
- To be prepared to address challenges from colleagues who are opposed to using a manual.

Participants at the APSF Cognitive Aid workshop are (left to right) Dr. Jeffrey Cooper, Dr. Sara Goldhaber-Feibert, Dr. Matt Weinger, Dr. David Gaba, Dr. Paul Preston and Dr. William Berry.
The workshop opened with an introduction by Jeffrey B. Cooper, PhD, APSF vice president and professor of Anesthesia at Harvard Medical School and founder and executive director of the Center for Medical Simulation. Dr. Cooper’s global perspective included admonitions that people should not expect the effective introduction of emergency manuals will be easy. Dr. Cooper also noted that it is relatively easy to just put emergency manuals in various locations where they may be needed; however, it is usually going to be very hard to get them to be used effectively. Clinicians should not underestimate the degree of culture change that is needed. The introduction of these tools can be an opportunity to help the culture change happen, and can be a reason to train together to facilitate effective implementation. As such, the process of introduction of emergency manuals is a great opportunity for good interactions and practice within the OR team. These interactions can promote a healthier safety culture.
Dr. Gaba presented a summary of why emergency manuals are needed in perioperative care, which dovetailed quite nicely with his prior lecture and his take home points. Following Dr. Gaba, Sara N. Goldhaber-Fiebert, MD, presented a lecture pertaining to the basic principles of implementing of emergency manuals. Dr. Goldhaber-Fiebert is clinical assistant professor and co-director of Evolve simulation program at the Department of Anesthesiology, Perioperative and Pain Medicine at Stanford University School of Medicine. She was lead author along with co-author, Dr. Steve Howard, on the recent publication, “Implementing Emergency Manuals: Can Cognitive Aids Help Translate Best Practices for Patient Care During Acute Events?” that appeared in Anesthesia & Analgesia in 2013. Dr. Goldhaber-Fiebert offered the following take home points:
1. Training and familiarity are necessary to facilitate effective use.
2. Implementation can be facilitated by
a. local champions and an interdisciplinary team
b. leadership buy-in
c. educational use and familiarity to enable clinical use
d. resources for training
e. using the “exclamation point” model of implementation (Figure 1).
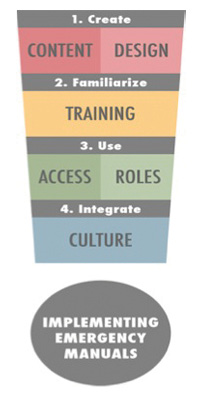
Figure 1. Exclamation point model of implementation for emergency manuals. Four vital elements for implementing emergency manuals. © 2012 Diagram: S. Goldhaber-Fiebert and S. Howard; first printed in Anesth Analg 2013;117:1149–61.
Following Dr. Goldhaber-Fiebert, Dr Paul Preston, safety educator for The Permanente Medical Group and a senior physician at the San Francisco Kaiser Foundation Hospital, presented, “What’s the right manual for your organization, group, or hospital?” Dr. Preston’s talk was on point and relevant to all of us, some of whom are in large academic organizations, as well as those of us in private practices, both large and small. Dr. Preston provided the following take home points germane to his lecture including:
1. There are no perfect lists, don’t take forever looking for them.
2. Strongly consider adapting what is already created to save time.
3. Make sure to allow time for testing these and training in the actual workplace. Doing so helps anesthesia providers decide which lists are best and most appropriate
4. Training and testing in the operating room environment is important because that is where the rescues truly happen.
At the conclusion of Dr. Preston’s lecture a panel discussion was held regarding when and how emergency manuals should be used, and a small group break-out session was held discussing values of the concept, how an example of a manual protocol would be practiced and used, as well as identifying challenges intrinsic to the implementation process.
Finally, Dr. William R. Berry, MPH, FACS, and principal research scientist at the Harvard School of Public Health as well as chief medical officer for Ariadne Labs, shared his expertise regarding overcoming the cultural barriers. Dr. Berry’s highly personal approach included his own story of being a survivor of sudden cardiac arrest. Dr. Berry offered these take home points for our participants and readers of this Newsletter:
- Implementing cognitive aids in the surgical environment is more than distributing manuals—it will require a culture shift. Currently in medicine, competence is measured by the ability to remember.
- Our ability to perform in an emergency can be compromised.
- Achieving behavior change is hard and it requires more than evidence. Individuals need to believe that cognitive aids are the “right” thing to do.
- We need to move from learning how to treat every emergency to any emergency. This can be achieved by learning teamwork, communication, and how to leverage cognitive aids.
- Checklists and cognitive aids can help us remember every critical step. Training how to effectively use cognitive aids in crisis situations is crucial.
- Training to improve teamwork and communication can help us deliver better care in every crisis.
This workshop was extremely well received and will likely have a significant impact on the participants. Our readers are highly encouraged to seek out and consider the implementation of cognitive aids that are becoming increasingly available. The Stanford Emergency Manual is an excellent starting place and is but one of the downloadable manuals (see http://emergencymanual.stanford.edu.) For further resources and links see the global site www.emergencymanuals.org.
Dr. Morell is the Senior Co-editor of the APSF Newsletter, a member of the APSF Executive Committee, and a private practice anesthesiologist in Niceville, FL.


 Issue PDF
Issue PDF