Editor’s Note: Dr. Betts was a recipient of an APSF Research Grant. He gives here a preliminary report on a portion of his work.
The optimal timing for anesthesia and surgery for children with an active or recent upper respiratory infection (URI) remains controversial. This study tested the hypothesis that the incidence of perioperative oxygen desaturation, laryngospasm, or bronchospasm in otherwise healthy children receiving general anesthesia who have or have recently had a URI is the same as in controls. The institution’s human study review board approved the study.
ASA physical status one or two day surgery patients with an active URI were enrolled in the study after the patient’s parents and the attending surgeon gave informed consent. These patients were compared to similar patients who ‘Were healthy with and without a history of having had a URI within the past six weeks.
The study protocol did not alter the anesthetic technique, including the premedication. After induction, in addition to the Nellcor N-200 pulse oximeter used clinically, the patient’s oxygen saturation and pulse rate were recorded by a Radiometer pulse oximeter in analog and histogram forms. A research technician monitored the study oximeter for artifacts. Data collection continued uninterrupted until the patient was discharged from the recovery room. Desaturation was defined as 90% hemoglobin oxygen saturation for more than 2.5 minutes (the minimum duration displayed by the oximeter histogram). Control patients were selected by matching them with active or recent URI patients primarily by age and procedure and secondarily by weight, sex and surgeon.
In addition, data on the occurrence of laryngospasm, bronchospasm and the necessity of airway maneuvers during the anesthetic and in the recovery room were collected. Telephone follow up one and seven days post anesthetic secured data on the development of post anesthetic complications.
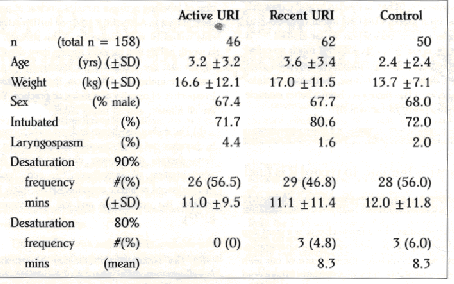
The results are summarized in the Table. There was no statistical difference in the demographics or in the incidence of laryngospasm or desaturation among the three groups. Only one postoperative complication occurred, a case of mild pneumonia in a six month old following a bilateral herniorrhaphy. The patient had had a recent URI and was treated at home with antibiotics. No patients developed bronchospasm or post intubation croup.
The incidence of desaturation appears quite high in this study because the oximeter reports fractional saturation (oxyhemoglobin(oxy + deoxy + deshemoglobins)) rather than functional saturation (oxyhemoglobin (oxy + deoxyhemoglobin)) which the Nellcor and most other American made oximeters report. Functional saturation typically runs four percentage points higher than fractional saturation.
Patients with lower airway disease as manifested by rales, ronchi or a productive cough were excluded from the study. Even so, one patient in the pilot study plus another patient in this study were diagnosed by their pediatricians as having mild pneumonia, treated at home in both cases with antibiotics. No chest x-rays were taken to confirm the diagnosis in either case.
Records were not kept of the number of potential study cases where either the surgeon, attending anesthesiologist or the patient’s parents declined to have the patient with an active URI anesthetized. This occurred bemuse most of these decisions were made by the surgeon and attending anesthesiologist before the study team was notified of the potential study patient. However, there was a noticeable softening of the surgeons’ and anesthesiologists’ attitudes as the study progressed, even though the results of the study were not made known to the medical community. Wormed consent makes this bias unavoidable
In a group of healthy pediatric patients having superficial surgery, the incidence of desaturation, laryngospasm, bronchospasm, and croup was not increased if the patient had or recently had had an upper respiratory infection. Caution should be used in applying the results of this study to the clinical situation as all of these patients were basically healthy and did not appear sick or toxic from their URI when they were anesthetized. In addition, 58 more control patients are needed to complete the study.
Dr. Betts is from the Department of anesthesiology and Critical Care Medicine, The Children’s Hospital of Philadelphia.