Introduction
During inhalation anesthesia, the patient’s airway is connected to a breathing system through which gases are delivered and eliminated. In addition to these functions, most anesthesia systems are capable of positive pressure ventilation of the patient’s lungs. It is well known that inadequate or inappropriate ventilation during anesthesia has been responsible for many mishaps. How to avoid inappropriate ventilation, including the avoidance of delivering gases with inappropriately low FiO2, is the subject of this discussion.
Current models of anesthesia machines and ventilators incorporate many features specifically designed to optimize their saw. Due to budgetary constraints faced by most institutions, many anesthesia practitioners do not have the luxury of frequently replacing all their old equipment with newer systems incorporating new safety features. We must strive, therefore, to make our existing anesthesia machines and delivery systems as safe as budget and design will allow. This can be achieved by always monitoring the performance of the equipment and sometimes by modifying it. Where neither can satisfy safety requirements, a machine or ventilator must be replaced.
The following are features of anesthesia machines and delivery systems that deserve attention:
1. Standing Ventilator Bellows
Older anesthesia ventilators were equipped with bellows that ascend during inspiration. The bellows are weighted to ensure descent and filling during expiration. When disconnected from the patient, the ventilator’s weighted bellows will fall and aspirate air, and it will continue to function, aspirating and delivering room air. Listening to the ventilator or monitoring inspiratory or even expiratory tidal volume will not reveal a disconnection of the ventilator from the patient. Some ventilators have pressure alarms that are activated when a predetermined pressure-for instance, 8 cm of water-is not reached during inspiration. However, this pressure may be reached during inspiration even after disconnections depending on the size and location of the leak, the inspiratory flow rate, and the tidal volume set. In some systems, the low pressure alarm limits can be adjusted. It is important in these systems to set the alarm threshold * below peak inspiratory pressure (the highest setting that fails to activate the alarm during normal mechanical ventilation).
Because, after a disconnection, the ventilator with an ascending (hanging) bellows (see Figure 1) will continue to move up and down and because a low pressure alarm may not he triggered, it is essential that the patient’s ventilation be monitored by auscultation (pretracheal, precordial or esophageal), inspection of chest excursion and capnography. The standing bellows (rising on exhalation) on modem ventilators will function only if the patient exhales into the bellows via a correctly connected breathing system, causing the bellows to ascend. Usually, if there is a disconnection, the bellows will not function. However, the clinician must be aware that partial obstruction of disconnected tubing and high fresh gas flow can cause the bellows to rise.
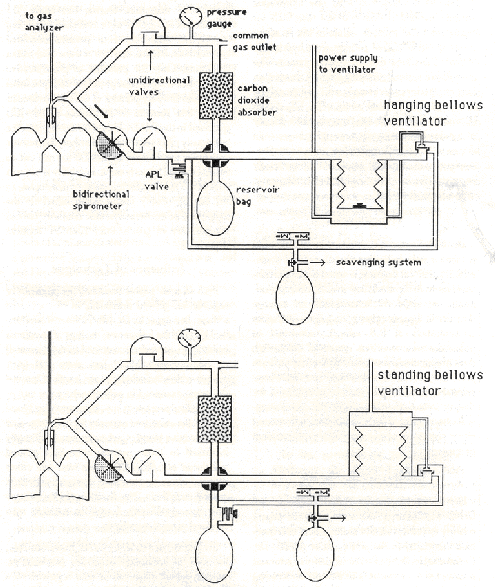
Figure 1: Circle breathing system and ventilator shown late in expiration with the expiratory valve still open. Top: Hanging Bellows Ventilator. In a disconnection, the weighted bellows will have aspirated ambient air. The APL (“pop-off”) valve is positioned as found in many older anesthesia machines. The valve must be closed when the ventilator is in use. Bottom: Standing Bellows Ventilator. ‘Me bellows will not rise in a disconnection, as the bellows will not fill spontaneously. The APL valve is positioned as found in many modem anesthesia machines. The valve need not be closed when the ventilator is in use.
2. Bag Pop-off */ventilator Selector Valve.
*The “pop-off” valve is formally called the adjustable pressure limiting (APL) valve.
Equipment with this selector switch locks out the bag and pop-off valve when the switch is turned to the ventilator mode (figure 1, bottom). In machines lacking the device, the practitioner must remember to close the pop-off valve when connections the patient to the ventilator (Figure 1, top). Otherwise, part of the tidal volume likely will be delivered to the ambient air (or scavenging system) instead of to the patient. Monitoring peak inspiratory pressure and expired tidal volume help in detecting such a leak through the open pop-off valve. Captio8raphy and eventually pulse oximetry will also reveal the effects of inadequate ventilation due to a leak through the open pop-off valve.
3. Locking Common Gas Outlet
A locking connection at the anesthesia machine outlet prevents the unintentional disconnection of the fresh gas delivery hose from the machine. Depending on circumstances, a partial disconnection here will decrease the delivery of fresh gas to the breathing system below the volume set on the flow meters on the anesthesia machine. This can set the stage for a progressive decrease in FiO2, as the patient may consume more oxygen than is supplied in the partially diverted fresh gas flow. Monitoring FiO2 with an oxygen analyzer and pressure in the breathing circuit are essential safety measures to guard against this unusual but potentially devastating development. As with other disconnects, a disconnection between anesthesia machine and common gas outlet creates a huge breathing system leak.
4. Breathing System Pressure Monitor
During manual positive pressure ventilation, partial or complete obstruction of the airway or breathing system components can be detected by the feet of the breathing bag upon compression. With mechanical ventilation, the clinician must rely on a pressure gauge to detect excessive pressures. In older machines, a mechanical manometer (the Bourdon gauge) was employed. The clinician has to inspect mechanical gauges frequently in order to detect unusual pressures. Modern equipment employs solid state electronic pressure monitors with an audible alarm in case of sustained, excessively high, or inappropriately low peak pressures in the breathing circuit.
5. Valve Function in Circle Systems
The unidirectional valves in the inspiratory and expiratory limb of a breathing circle system prevent rebreathing. Inspection of the valve leaflets during ventilation ran detect some valve malfunc6ons. Difficult to see are malfunctions caused by a warped valve disc. Spirometry in the circle system helps monitor valve function. If the inspiratory valve becomes incompetent, some of the expired volume returns into the inspiratory limb of the breathing circle; the expired tidal volume, therefore, is reduced. A spirometer in the expired limb will help diagnose an incompetent inspiratory valve. When the expiratory valve malfunctions, gas flow in the expiratory limb becomes bi-directional; a bi-directional flow meter will reveal this evidence of an incompetent expiratory valve as reverse flow. Typical capnograms for valve malfunctions are shown in Figures 2 and 3.
6. Scavenger Connections
In older anesthesia machines, it was possible to connect mistakenly the scavenging system to the breathing circuit. With such misconnection, catastrophe will result because the patient cannot inhale or exhale. Sensing the pressure in the breathing circuit with monitors armed with appropriate low (subatmospheric) and high alarms and monitoring and expired tidal volume will help provide an early alert to this rare but very serious error.
Modem anesthesia machines are standardized so that all connections of the breathing circuit are either 15 mm or 22 mm and the scavenging fittings are 19 nun or a diameter index safety system (DISS). Accordingly, the dissimilarities of the fittings make incorrect connections much more difficult.
7. Diameter Index Safety System
In years gone by, it was possible to connect oxygen or nitrous oxide from the central supply to either the nitrous oxide or oxygen system of the anesthesia machine. Male/female connectors that are specific for each gas, the DISS, reduce the hazard of having nitrous oxide piped into the oxygen flow meter of the anesthesia machine. However, even this safeguard does not rule out the possibility of accidental crossing of gas pipelines, for instance during renovation or maintenance in the hospital in which gas pipelines must be manipulated. Therefore it is essential and now universally recognized that the oxygen concentration must be monitored in the breathing circuit of the patient, usually in the inspired side. With rapidly responding oxygen analyzers, both inspired and expired oxygen can be monitored.
8. The Pin Index Safety System
The pin index safety system is to gas cylinders what the diameter index safety system is to pipes carrying compressed gases. It assures that only an oxygen cylinder can be attached to the oxygen yoke, a nitrous oxide cylinder connected to the nitrous oxide yoke, and so on. This is accomplished by two pins on the anesthesia machine that match with holes on the cylinder. Unfortunately, when one pin falls out or when several washers instead of a single one are used, the pin index system can be defeated. Therefore, the oxygen monitor in the breathing system provides an essential backup safety feature.
9. PEEP
Valves PEEP valves can be added to any machine utilizing 22 mm fittings. Some PEEP valves are unidirectional and therefore, when placed inappropriately in the inspiratory limb, can obstruct flow entirely. Several deaths have been linked to this. Monitoring pressure in the breathing system, monitoring expired tidal volume and the capnogram, and carefully observing the patient’s ventilation will help prevent the inappropriate placement of PEEP valves. Manufacturers have incorporated PEEP valves into modem anesthesia machines, thereby making it difficult to place them incorrectly. Note, however, that some of these integral PEEP valves can be hard to read and are easily accidentally left “on” from one patient to the next and this may be dangerous.
10. The C02 Absorber Bypass Switch
On older anesthesia machines, it was possible to bypass the carbon dioxide absorber in order to increase the patient’s alveolar PC02When the bypass was unintentially turned on, or when the clinician failed to turn it off, patients developed severe hypercarbia. Monitoring carbon dioxide in the breathing system will help to prevent this occurrence.
Modem anesthesia machines no longer carry a bypass switch for the carbon dioxide absorbent. Presented here are comments and suggestions regarding ten features of older anesthesia delivery systems. AN can he involved with inadequate ventilation under anesthesia. Attention to the points outlined here should help eliminate accidents associated with these older configurations.
Ms. Nichols is Chief Nurse Anesthetist, Department of Anesthesiology, University of Texas, Health Science Center at Houston.
Editor’s note: Letters to the editor on this topic of older anesthesia equipment are welcome and will be considered for publication in a future issue.
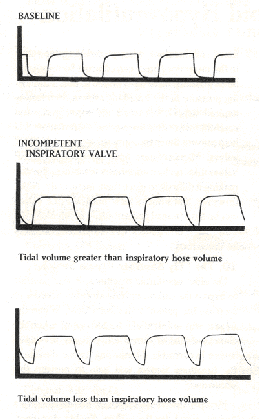
REVERSE FLOW OCCURS IN THE INSPIRATORY HOSE
Figure 2: Capnograms with normal valve function (top) and with a detective inspiratory valve (middle and bottom). End-tidal values were increased in the latter two. In the middle panel the volume of gas deposited into the inspiratory hose during expiration was smaller than the next inspiratory volume. Therefore, the capnogram eventually reached the baseline. In the bottom figure, the inspired volume was not large enough to replace all carbon dioxide-containing expired gas, and the capnogram could not reach baseline. A sloping descending limb of the capnogram is typical for an incompetent inspiratory valve.
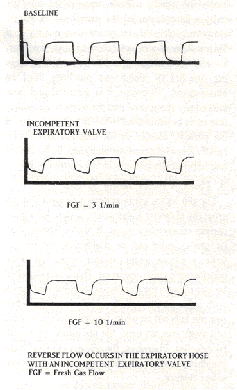
Figure 3: With an incompetent expiratory valve, endtidal values increase, and inspiratory values do not return to baseline. The same picture is seen when the carbon dioxide (CO2) absorber is exhausted. However, increasing fresh gas flow lowers both end-tidal and inspired values when the C02 absorber is exhausted, but not when the expiratory valve is incompetent,

