INTRODUCTION
Anesthesia providers participate in patient handoffs several times for each patient under their care. Each handoff has the potential for poor communication that may jeopardize patient safety. In fact, a recent study suggested that more operating room (OR) anesthesia handoffs are associated with increased adverse events.1 With this potential for adverse events in mind, the Joint Commissions 2006 National Patient Safety Goal requires “a standardized approach” for handoffs.2
As a quality improvement initiative, our institution has focused on the anesthesia team-to-PACU nurse handoff. The ASA defines the standard for OR-to-PACU handoff: “Upon arrival in the PACU, the patient shall be re-evaluated and a verbal report to the responsible PACU nurse by a member of the anesthesia care team who accompanies the patient.”3 In spite of these guidelines, the quality and quantity of information exchanged can still be variable. Some institutions have adopted standardized handoffs, such as SBAR (situation, background, assessment, recommendation) to try to ensure a quality exchange of information. However, no large scale studies have indicated the best structured approach and no widely accepted guidelines exist for PACU handoff.4
Prior efforts to standardize the PACU handoff have been viewed as a burdensome addition to the handoff process. Therefore, our aim was to create a succinct checklist to help expedite the handoff process while increasing meaningful communication between anesthesia provider and PACU nurse.5 We hypothesized that we would still observe a significant increase in information exchanged despite fewer checklist items. In addition, a more succinct checklist would allow for an easier transition into everyday practice and would avoid the negative response that similar checklists have received in the past.
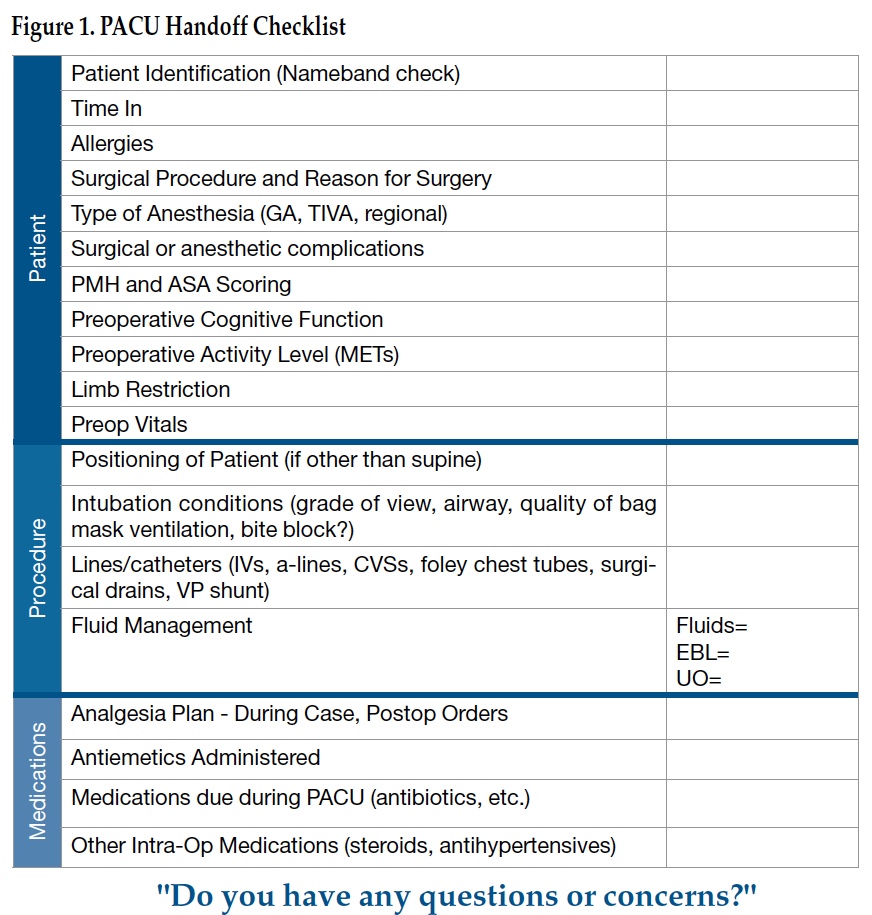
Figure1. PACU Handoff Checklist
METHODS
Institutional Review Board approval was obtained prior to this study. To create our checklist, we first used the information published in prior studies and anesthesia textbooks to create an all-inclusive 42 itemized list in a PACU handoff.5 We modified our checklist to include only data relevant to our institution’s PACU handoff process. For example, during casual conversation with our PACU nurses, residents, CRNAs, and attending anesthesiologists, we found that “failed punctures” and “inspection of all lines and catheters” were addressed during a separate nursing assessment so they were excluded from the checklist. This feedback helped reduce our checklist down to 17 items.
The third step of preparing the PACU Handoff Checklist was to measure its effectiveness during actual PACU handoffs. We randomly observed 10 PACU handoffs and screened for additional items exchanged that should be included in our handoff checklist. We found that “preoperative vital signs” and “other medications (antihypertensives and steroids)” were an integral part of the handoffs process but were not included in previous lists.
Our final checklist (Figure 1) included a unique checklist item, “closed loop communication,” in order to address two-way communication between PACU nurse and anesthesia provider. Both the ASA and the Joint Commission describe two-way communication as an integral part of any transition of care.
An item was counted as successfully exchanged between anesthesia resident and PACU nurse if the item was mentioned in any capacity. Data collectors were volunteer medical students who were independent from the care team and study team. They observed the handoff without intervention and made no assessment of the quality of the information exchanged. A stopwatch was used to record the time from the start to finish of the sign out. All times were rounded to the nearest second.
We observed PACU handoffs completed by residents of all years of training during the months of April to June, so that all residents had at least 6 months of clinical training before participating in our study. We collected baseline data (Group A) by observing residents complete the PACU handoff without the aid of a checklist. We observed 50 handoffs in this group. The data collectors used the PACU Handoff Data Collection sheet to record the items that were exchanged during handoff as well as the time it took to complete the handoff. The data for these 50 handoffs made up our control group.
Once baseline data was collected, the checklist was introduced to our residents. Prior to the start of one of our daily academic conferences, each item on the checklist was reviewed with the residents so that they were able to appreciate a successful handoff of information. After this introduction to the checklist, Group B data were collected as residents completed the PACU handoff by using the PACU Handoff Checklist as a guide for exchange of information. The same PACU Handoff Data Collection Sheet was used to record items exchanged and the time it took to complete the handoff.
RESULTS
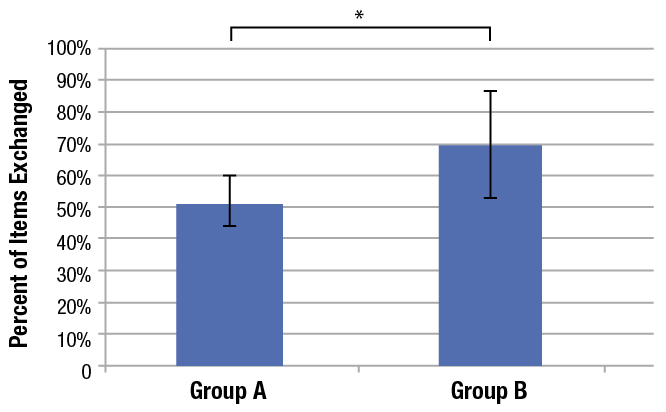
A total of 14 residents (6 CA-1 residents, 4 CA-2 residents, 4 CA-3 residents) were observed for patient handovers in Group A (control group). A total of 8 residents (4 CA-1s, 3 CA-2s, 1 CA-3s) were observed for patient handoffs in Group B (experimental group). Six residents participated in handoffs in both groups (4 CA-1s, 2 CA-2s). Each resident participated in 1-8 handovers. The percentage of overall items handed off increased significantly with the use of the PACU Checklist (Group B: average, 69.5% +/- 16.5%, Group A: average, 51.50% +/-8.28% p = 0.018) (Figure 2).
Residents who used a checklist (Group B) handed off 8 items on the checklist with a significantly higher frequency compared to residents who did not use a checklist (Group A). These items were: Antibiotics (p = 0.016), Standing Medications (p <0.001), Preoperative Cognitive Function (p < 0.001), Complications (p < 0.001), Patient Positioning (p < 0.001), Limb Restriction (p < 0.001), and Preoperative Activity Level(p < 0.001). They also completed the task of Closed Loop Communication more often (p < 0.001)
While they included significantly more items in their handoff, residents who used the PACU Handoff Checklist spent a significantly longer amount of time completing their handoff compared to those that did not use a checklist (Group B: 126.4 +/- 52.25 seconds; Group A: 100.86 +/- 36.00 seconds, p = 0.011).
The six residents that participated in handoffs in both groups (4 CA-1s, 2 CA-2s) accounted for 28 handoffs in Group A and 20 handoffs in Group B. In a subgroup analysis, percentage of overall items exchanged by this crossover resident subgroup was very similar to the total (Group B [crossover residents]: average, 69.96% +/- 12.62%; Group A [crossover residents]: average 52.23% +/- 8.96%, p = 0.014). They also spent a significantly longer amount of time completing their handoffs with the checklist (Group B: 131.5 +/- 56.43 seconds; Group A: 106.61 +/- 40.44 seconds, p = 0.002).
The more time spent on the handoff, the more items were addressed. Handoffs with the use of the checklist (Group B) spent less time discussing each item than handoffs that did not use the checklist (Group A), although this difference did not approach statistical significance (Group B: 7.71 +/- 3.17 seconds per item, Group A: 8.23 +/- 2.70 seconds per item, p = 0.366).
Closed suction catheter that was misused resulting in oxygen desaturation.
DISCUSSION
With the use of a checklist, the percentage of items exchanged during PACU handoff increased significantly (Figure 2). The checklist clearly increased the amount of information exchanged during our handoffs; but only 4 out of 50 handoffs included 100% of the information listed. Items most commonly missed include Preoperative Cognitive Function, Lines/catheters, and Antiemetics. Missed items may have been excluded for 2 reasons. The resident may have deemed a particular item non-essential to the transition of care or may have missed the item due to general unfamiliarity with the new tool. In the latter case, further use of the checklist would likely lead to an additional increase in amount of information included in the PACU handoff.
Failure in communication has been shown to risk patient safety in several studies across different specialties.6-9 When checklists were introduced to preoperative and intraoperative care, there has been an association with a significant reduction in morbidity and mortality.10,11 Agarwal and colleagues introduced a standardized handoff tool for transition of care from the operating room to pediatric cardiac ICU. This effort led to a decrease in postoperative complications and an improvement in 24 hour patient outcomes.12
In the only randomized clinical trial to date on PACU handoffs, Salzwedel and colleagues surveyed senior anesthesiologists at their institution and constructed a checklist consisting of 37 items integral to their PACU handoff.5 They found that the use of a checklist for PACU handoff improved exchange of information, but took significantly longer (35 seconds) when compared to handoffs that did not use a checklist. Our study yielded similar results; handoffs in Group B were 26 seconds longer. It appears that the extra time invested in an organized PACU sign out results in more information exchanged. However, the increased burden it places on the anesthesia provider may deter organizations from implementing similar strategies. We quantified this difference by measuring the “velocity” of the handoffs. Group B, with the use of the checklist, exchanged 7.7 items/second which is an improvement over Group A, which exchanged 8.2 items/second without the checklist.
Our study is the first study to target handoffs by residents. At this early juncture in training, an organized PACU handoff may have increased benefit. Without the polished clinical skills and judgment of a seasoned anesthesia provider, residents may be more likely to miss an important piece of information in their sign out.
There were several inherent limitations to our study. Because our data collectors did not record any qualitative data about the information exchanged, we are unable to tell if any errors were made during these handoffs; in fact, we are not able to comment on the quality of handoffs at all, but simply report the percent of items addressed.
Any effort to create a comprehensive sign out tool will invariably increase the length of the sign out while an effort to create an efficient sign out tool will streamline the sign out while possibly excluding vital information. The information that should be included in a complete, thorough PACU sign out varies greatly from patient to patient; therefore, any standardization tool is often going to be too comprehensive or too efficient.
The anesthesia provider is not the only person providing sign out information to the PACU nurse; our surgical colleagues provide information that is also integral to patient care. Future endeavors will aim to incorporate the surgical handoff in an effort to create a comprehensive, multidisciplinary sign out process. In addition, a larger study will allow us to measure the effect that a standardized sign out process will have on patient outcome.
Dr. Potestio is a CA-2 and Dr. DeGroot is an Associate Professor in the Department of Anesthesiology, Medstar Georgetown University Hospital, Washington, DC.
Mr. Mottla is a 2nd year medical student and Ms.Kelley is an RN in the Post Anesthesia Care Unit, at Medstar Georgetown University Hospital, Washington, DC.
References
- Saager L., Hesler B. D., You J., Turan A., Mascha E. J., Sessler D. I., Kurz A. Intraoperative transitions of anesthesia care and postoperative adverse outcomes. Anesthesiology 2014;121:695-706.
- Arora V., Johnson J. A model for building a standardized hand-off protocol. Joint Commission Journal on Quality and Patient Safety 2006; 32: 646-655.
- American Society of Anesthesiologists Committee on Surgical Anesthesia. Guidelines for patient care in anesthesiology. ASA website. https://www.asahq.org/For-Members/Standards-Guidelines-and-Statements.aspx. Last amended October 19, 2011. Accessed October 19, 2014.
- Hoefner-Notz R., Wintz M., Sammons J., & Markowitw S. Using evidence-based practice to implement standardized anesthesia-to-PACU handoff tool and improve PACU staff satisfaction. Journal of PeriAnesthesia Nursing 2013;28:e3.
- Salzwedel C., Bartz H. J., Kühnelt I., Appel D., Haupt O., Maisch S., & Schmidt G. N. The effect of a checklist on the quality of post-anaesthesia patient handover: a randomized controlled trial. International journal for quality in health care 2013;25:176-181.
- Wilson RM, Runciman WB, Gibberd RW, Harrison BT, Newby L, Hamilton JD. The Quality in Australian Health Care Study. Medical Journal of Australia 1995; 63:458-71.
- Hart E. M., & Owen, H. Errors and omissions in anesthesia: a pilot study using a pilot’s checklist. Anesthesia & Analgesia 2005;101:246-250.
- Sutcliffe K. M., Lewton E., & Rosenthal M. M. Communication failures: an insidious contributor to medical mishaps. Academic Medicine 2004;79:186-194.
- Patterson ES, Roth EM, Woods DD, Chow R, Gomes JO. Handoff strategies in settings with high consequences for failure: lessons for health care operations. Int J Qual Health Care 2004;16:125-132.
- Haynes A. B., Weiser T. G., Berry W. R., Lipsitz S. R., Breizat A. H. S., Dellinger E. P., Herbosa T., Joseph S., Kibatala P.L. Lapitan M.C., Merry A.F., Moorthy K., Reznick, R.K., Taylor B., Gawande A. A. A surgical safety checklist to reduce morbidity and mortality in a global population. New England Journal of Medicine 2009;360:491-499.
- Wolff A. M., Taylor S. A., & McCabe J. F. Using checklists and reminders in clinical pathways to improve hospital inpatient care. Medical Journal of Australia 2004;181:428-431.
- Agarwal H. S., Saville B. R., Slayton J. M., Donahue B. S., Daves S., Christian K. G., Bichell D.P., Harris Z. L. Standardized postoperative handover process improves outcomes in the intensive care unit: a model for operational sustainability and improved team performance. Critical Care Medicine 2012;40:2109-2115.


 Issue PDF
Issue PDF