To the Editor
A newsletter dedicated entirely to patient safety is quite a commendable venture and being a regular reader, I wish to utilize this medium to remind the anesthesiology world of corneal abrasion.
Corneal abrasion under anesthesia is rare, but its occurrence results in foreign body sensation in the eye and significant pain and discomfort that can progress to ocular infection and loss of vision if improperly managed.
Any form of anesthesia that leads to unconsciousness can easily predispose patients to this injury. Risk factors may include long duration surgical procedures, lateral positioning, prone position, as well as head and neck surgeries.
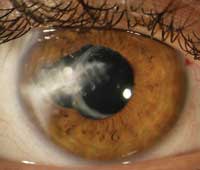
Photo courtesy of Richard Hackel, CRA, Kellogg Eye Center, University of Michigan.
The exact mechanisms of the injuries are not clearly understood, but certain preventive measures appear worthwhile to adopt:
- Pulse oximeter sensors should be placed on the ring or fifth finger because most patients, on emergence from anesthesia, are unlikely to rub their eyes with these fingers.
- In general anesthesia, following induction and immediate loss of consciousness and lid reactivity, the eyes should be taped shut preferably from upper lid down, making sure that the eyelids are properly apposed. This may prevent injury during mask ventilation and laryngoscopy from objects on the anesthesiologist’s wrist (watches, bracelets), breast pocket (identity cards), and neck (stethoscope, jewelry).
- Use of appropriate sized masks for ventilation as opposed to oversized ones that impinge on the eyes.
- There is no proven benefit in the use of eye ointments under anesthesia, but a dry cornea is more susceptible to abrasion. In high risk cases, a benefit may be obtained, but care must be taken during application to prevent the tip of the applicator from contacting the eye.
- Removal of the occlusive tape of the eye at the end of surgery should be gentle and preferably from the upper eyelid to the lower.
In postoperative clinical situations with a high index of suspicion based on anesthetic events and patient complaints, an ophthalmologic consultation is appropriate.
Celestine O. Okwuone, MD
Hershey, PA

