The idea that medical errors and the adverse events they cause are major public health concerns is not likely to be news to readers of this Newsletter. It has been seven years since the Institute of Medicine (IOM) highlighted the fact that up to 98,000 Americans die every year due to medical errors.1 This places medical error as the leading cause of accidental death in the United States, surpassing the combined totals of motor vehicle accidents, fire, and drowning. Since then, similar data have been found in the Canadian health care system, with in-hospital adverse events accounting for between 9,200 and 24,000 deaths.2 A recent report went so far as to suggest that limiting health care to the Medicare population may actually improve mortality rates by decreasing the number of medical errors to which the elderly will be exposed.3
Many potential solutions to the problem of medical error have been proposed, including computerized provider-order-entry,4 site/side documentation for invasive procedures,5 banning ambiguous abbreviations,5 and many others. Teamwork, however, is perhaps the most recommended solution. Again, the idea that teamwork has the potential to improve patient safety is not news. The follow-up report from the IOM published in 2001, Crossing the Quality Chasm, recommended that health care teams better use the concepts of Crew Resource Management (CRM) to improve care.6 There have been small steps in the right direction over the ensuing 5 years. Team training has been associated with improved attitudes, behaviors, and outcomes. Grogan demonstrated that an 8-hour course on teamwork and CRM concepts can improve staff attitudes toward safety and teamwork,7 and the same group has found that team training has improved patient safety in the operating room (Seddon, personal communication). Morey et al. found that classroom-based team training effectively increased teamwork behaviors and improved outcomes.8
Unfortunately, successfully implementing a teamwork structure and changing the culture in which we practice is still the exception rather than the rule. Many forces are impeding the shift to a new, team-based, medical paradigm, including the logistical and financial requirements of such a change, fears that working as a team might increase malpractice exposure, and even intransigence to change itself. However, I believe there is a more fundamental factor at work. I believe that most clinicians simply do not understand what “teamwork” would mean in the medical environment. They do not understand how a medical team would act differently from the way medicine is currently practiced. Worse, since they do not know what the final product should look like, they have no idea how to start to makes the changes that would be necessary to get there. Although some literature does exist,9,10 little has been published describing what teams do or what steps to take to implement teamwork. As a result, even those who might embrace the concepts of teamwork are often left unable to even start the process.
In an attempt to help to fill this gap in understanding, the Society for Obstetric Anesthesia and Perinatology (SOAP) hosted a patient safety panel at its annual meeting in Hollywood, Florida, this year. Three national experts in medical teamwork training presented the training methods they use to train their staff to be a team on their labor and delivery units.
Dr. Benjamin Sachs, Chairman of the Department of Obstetric and Gynecology at Beth Israel Deaconess Medical Center (BIDMC) and Professor at Harvard Medical School presented first. Dr. Sachs indicated that his department began a strong commitment to patient safety after a major adverse event in 2000.11 The training program used at BIDMC was developed in conjunction with the Department of Defense, Tricare, and the American Institute for Research, and with the help of such teamwork experts as Eduardo Salas. Originally developed as part of a multi-center prospective randomized trial on the effects of team training on obstetric outcome, the training course has gone through modifications based on the lessons learned from the study and the most recent understanding of what makes teams work well. The training includes a 4-hour classroom-based training session to teach the basic concepts of teamwork. These concepts include Leadership, Situation Monitoring, Mutual Support, and Communication. The didactic training is supported by the creation of 3 separate types of multidisciplinary teams. The first is the core team, those who administer direct patient care. The second team is the coordinating team, a group that helps to balance work loads and staffing, and is responsible for ensuring that teamwork behaviors such as team meetings and briefings occur. The third team is a pre-determined set of clinicians designated to respond to emergencies, the contingency team. Well-defined tools and behaviors, including team meetings and briefings, communication techniques, check lists, and feedback and conflict resolution strategies are used to remind staff how to act “teamly.” Finally, a structured implementation process helps to bring these concepts, behaviors, and practices into the clinical environment. This implementation process includes a deliberate schedule for adopting each new behavior, a strong coaching effort, strategies for dealing with resistance, and periodic reinforcement of the behaviors to sustain the changes.
Dr. Sachs presented data demonstrating a 25% decrease in major adverse outcomes in their obstetric patients, with the best improvements coming in the high-risk preterm deliveries. In addition, his group found a nearly 50% reduction in malpractice cases since they implemented their teamwork system.
Dr. David Birnbach, Vice Chairman of the Department of Anesthesia and Director of the Center for Patient Safety at the University of Miami presented next. His group uses a high-fidelity simulator at Jackson Memorial Hospital to teach teamwork concepts. The simulation center at Jackson Memorial is state-of-the-art, costing more than $3 million annually in equipment and staffing. It includes an operating room environment, complete with surgical and anesthesia equipment, actors to play the obstetric and nursing staff, and a “dummy” patient that can be manipulated from a control room to simulate nearly any physiologic perturbation. This realistic environment allows staff to be immersed in “real life” obstetric scenarios and requires that they use and practice their teamwork skills. Dr. Birnbach showed multiple videotapes of actual cases from the simulator. These videos are used to debrief the sessions after the staff goes through the training. While clinical skills can be taught and honed in this environment, Dr. Birnbach indicated that the emphasis is on teamwork concepts, especially communication and resource management. Several of the scenarios depicted anesthesia staff getting into trouble and not even telling the rest of the team about the problem or much less asking for help. The hope is that by seeing themselves make these teamwork errors, staff will be able to change their behaviors and better use teamwork skills.
In a novel use of their simulator, Dr. Birnbach is creating “best practice” scenarios. He has taken patient complaints and re-enacted them in the simulator. Actors re-enact both the medical and interpersonal problems as they were described by the patient. A second version of the scenario is then created that demonstrates a better way that the situation could have been handled.
Dr. Paul Preston was the third panelist. Dr. Preston is a staff anesthesiologist at the University of California, San Francisco. He is a leader in developing team training educational programs in the Kaiser Permanente system. After working with Dr. David Gaba in the use of simulators to teach Anesthesia Crisis Resource Management and Dr. Michael Leonard in Humans Factors analysis and training, Dr. Preston has become an expert in teaching staff to work as a team. Dr. Preston presented a team-training model that incorporates both a classroom-based education and simulated crisis management scenarios. The training is a 4-hour course. He starts with a quick review of human factors and CRM concepts. These include briefings, communications skills, assertion for safety, situation awareness, leadership, and resource management. He then brings staff through simulated emergencies. He has a relatively “low-tech” simulator that he is able to bring to the hospital being trained. Thus, staff are able to practice the crisis management scenarios in their usual environment with their colleagues. The simulated cases are based on real cases that focus on potential or identified weaknesses in the system. He has more than 2 dozen obstetric and general medical or surgical emergencies. He videotapes these sessions and then debriefs the staff. Again, these debriefings focus on systems issues, communication, and teamwork, and not clinical skills.
Based on the experience bringing this simulated environment into many hospitals, Dr. Preston was able to present some important lessons learned. These include some not-so-surprising facts (obstetricians are often overloaded and do not communicate well), important leadership facts (nursing leaders are invaluable in getting a “big picture” of the unit and helping the obstetric providers maintain situation awareness), and even rather mundane practical facts (moving to the OR in a stat situation works best if the piggybacked IVs are all unplugged, the epidural is placed on the bed, and one person is in charge of telling people when to go). Dr. Preston stated that perhaps the most powerful effect of the team training is the consistent way that it encourages the clinicians to come together to communicate and to fix problems.
A lively discussion and question and answer period followed the panelists’ presentations. In addition, the Board of SOAP decided to create a patient safety committee in order to ensure that future meetings include similar educational activities.

A snapshot of the control panel and “O.R.” in the simulator at Jackson Memorial Hospital.
The 3 presenters on this panel have successfully brought teamwork into their work environments. More importantly, they have created educational systems that help clinicians to understand what teamwork means in the medical environment and how to gain the skills necessary to become a good team member. The 3 systems are quite different, but each incorporates the necessary components of CRM and has been used successfully. One hopes that those in attendance returned to their practices with a better understanding of what teamwork and CRM mean in medicine and how they can be taught and implemented. With this important step, perhaps many more units can make the necessary changes to a safer team-based practice.
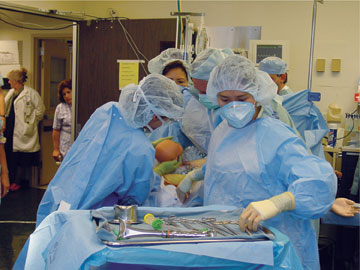
A birth in the Kaiser Simulator.
Dr. Pratt is an Instructor at the Beth Israel Deaconess Medical Center in Boston, MA.
References
- Committee on Quality of Health Care in America, Institute of Medicine. In Corrigan, Kohn, Donaldson (eds). To Err Is Human: Building a Safer Health System. Washington DC: National Academy Press; 1999:26.
- Baker GR, Norton PG, Flintoft V, et al. The Canadian Adverse Events Study: the incidence of adverse events among hospital patients in Canada. CMAJ 2004;170:1678–86.
- Dartmouth Medical School Center for the Evaluative Clinical Sciences. The Care of Patients with Severe Chronic Illness. Dartmouth, NH: The Trustees of Dartmouth College, 2006. Available online at: http://www.dartmouthatlas.org/atlases/2006_Chronic_Care_Atlas.pdf. Accessed June 5, 2006.
- The Leapfrog Group. National Quality Forum Endorsed Safe Practices. Available online at: http://www.leapfroggroup.org/for_hospitals/leapfrog_safety_practices/nqf-safe_practices. Accessed June 5, 2006.
- Staten PA. Patient safety: new goals set for 2003. Nurs Manage 2003;34:14.
- Committee on Quality of Health Care in America. Chapter 5 – Building Organizational Supports for Change. Crossing the Quality Chasm: A New Health System for the 21st Century. Washington, D.C.: National Academy of Sciences, 2001:111–144.
- Grogan EL, Stiles RA, France DJ, et al. The impact of aviation-based teamwork training on the attitudes of health-care professionals. J Am Coll Surg 2004;199:843–8.
- Morey JC, Simon R, Jay GD, et al. Error reduction and performance improvement in the emergency department through formal teamwork training: evaluation results of the MedTeams project. Health Serv Res 2002;37:1553–81.
- Curtis JR, Cook DJ, Wall RJ, et al. Intensive care unit quality improvement: a “how-to” guide for the interdisciplinary team. Crit Care Med 2006;34:211–8.
- Thompson D, Holzmueller C, Hunt D, et al. A morning briefing: setting the stage for a clinically and operationally good day. Jt Comm J Qual Patient Saf 2005;31:476–9.
- Sachs BP. A 38-year-old woman with fetal loss and hysterectomy. JAMA 2005;294:833–40.


 Issue PDF
Issue PDF