Editors note: Dr. Lichton was a recipient of an APSF Research Grant for 1987. He reports here on a portion of his work,
Anesthesia is generally thought to be associated with minimal risk. Nonetheless, certain cases in which anesthesia is thought to be a key factor in the demise of the patient make the headlines because of multimillion dollar settlements. We felt that current impartial data on death after anesthesia and surgery would be useful to assess risk in a variety of settings.
Data tapes representing the National Hospital discharge Survey (NHOS) between the years 1979 and 1984 were examined. The National Master Facility Inventory of Hospitals and Institutions constitutes the basis for hospital selection in this survey. The National Center for Health Statistics has published guidelines for the maintenance of this inventory as well as procedures for insuring completeness of its coverage. Hospitals with fewer than 1,000 beds were stratified according to size and geographical region. Allocation of hospitals in the survey were then made in a controlled fashion so that hospitals were property distributed by type of ownership and geographic division. AU hospitals with 1,000 beds or more were included with certainty in the sample. Smaller hospitals were included by probabilities ranging from certainty for the largest hospitals to I in 40 for the smallest hospitals.
Within hospitals, the smallest fraction of discharged patients were evaluated in the largest hospitals, and the largest fraction was examined in the smallest hospitals. The discharges were selected by a random technique, usually by the last digit in the patient’s medical record number. A weight was assigned for each record which was based on the reciprocals of the probability of sample selection, adjustment for non-responses, and ratio adjustment for fixed totals. The weight allows for extrapolation to national or regional estimates.
Each record includes information on patient age, date of admission and discharge, discharge status, diagnoses (at most seven), procedures performed (at most four), age, bed size of hospital, source of payment, hospital ownership, and region of country. This information was used in our analysis. We selected only those patients who we felt had a high likelihood of requiring general or regional anesthesia for their procedure, whose “discharge status” was “dead”, and who died within six days of their surgical procedure. Ratios were calculated by determining those patients who died who fit a certain criterion and dividing this number by the total number of patients who fit that category. For example, the relative ratio for patients who died and had Medicare was calculated by finding those Medicare patients who died and then dividing this number by the total number of Medicare patients who had surgery.
Between 1979 and 1984, a total of 745 patients from the sample population of hospitals who had surgery were determined to have died within one day of their surgery; using the weighting factors, this represents 135,570 patients in the United States. A total of 1,798 patients, representing 330,499 patients nationwide died within six days of their surgery. In all, 343,800 patients, representing a nationally projected 67 million patients underwent surgery during the six-year period. The incidence of death within one day of surgery was 2.21 per thousand, while the incidence of death was 5.33 per thousand within six days of surgery. The table lists the death rates per thousand for each year during the study. Both crude and standardized rates are listed. Because the average age of patients undergoing surgery has increased between the year 1979 and 1984, the death rates have be-en standardized; we arbitra6y chose to standardize the death rates to the age distribution present in 1979.
Young, Old at Risk
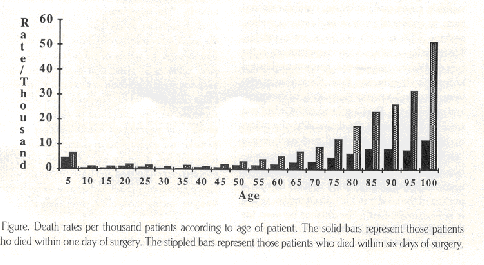
Death rates are highest in the young and old; the figure illustrates death rates according to age of the patient. Hospitals over 300 beds have higher death rates following surgery than do smaller hospitals. Government and church hospitals, both of which have socio-economically disadvantaged, have higher death rates than proprietary hospitals. Patients with Medicare insurance, and those without insurance have greater mortality rates following surgery than do patients with commercial insurance. Patients undergoing thoracic, cardiac, vascular and neurosurgical procedures also have a higher incidence of death following surgery than do patients undergoing other types of procedures.
The results of our study are interesting in several respects. The standardized death rates are relatively constant for patients who died within one and six days of surgery. Anesthesia residency programs tend to emphasize teaching for cardiac, vascular and neurosurgical cases; this practice seems confirmed by the relatively high incidence of patients who died after surgical procedures.
Death rates are relatively higher in government or church-owned hospitals than in proprietary hospitals; the mason for this is not totally clear. Patients with Medicare show the highest ratio of death after surgery. This undoubtedly correlates with advanced age; these patients tend to have a high incidence of organ failure than do their younger counterparts. Patients with self payment or no charge show a high ratio of death, particularly within one day of surgery; this may be artifactual, however, due to the relatively small size of this population (the variance of the measurement is relatively high).
Our results are similar to those obtained in similar current studies of mortality in Europe, and in older studies from the United States. In 1982, the Association of Anaesthetists of Great Britain and Ireland reported an overall mortality rate of 0.53% within six days of operation. The data in our study provides a means for us in the future to quantify changes in our quality of care and patient outcome caused by measures forced on us by cost containment measures, legal influences, or our own beliefs.

Dr. Lichtor is Assistant Professor, Department of Anesthesia and Critical Care, University of Chicago.

