In My Opinion
During the 1999-2000 fiscal year, the Institute of Medicine (IOM) released a report entitled “To Err is Human” which essentially told us that the healthcare system in the United States was “broken” and badly in need of repair.1 Subsequent to the IOM report, the Agency for Healthcare Research and Quality (AHRQ) released their recommendation for clear opportunities for safety improvement in the healthcare industry. One of the top 11 patient safety practices was the use of real-time ultrasound guidance during central line insertion to prevent complications. This document,2 authored by Dr. Jeffrey Rothschild, was quite concise and indicated that portable ultrasound could improve safety and success in the placement of central vascular access devices (CVAD). The document, however, indicated that “experienced anesthesiologists can continue to place most CVADs without ultrasound guidance.” We interpret this to mean that in the perioperative setting, experienced anesthesiologists do not require the use of portable ultrasound to facilitate central vascular access. We strongly disagree with this statement. It is our feeling that the safety and success rate of central vascular access, even in the hands of experienced anesthesiologists can be substantially improved with the use of portable ultrasound. A substantial number of recent publications substantiate that increased patient safety and improved success rates accrue from the use of portable ultrasound when performing central vascular access.3-8
 |
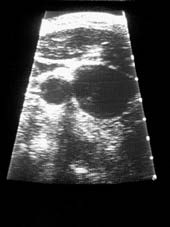 |
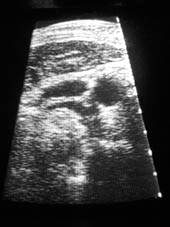
| Portable ultrasound images from left (1A) and right (1B) neck, respectively in the same individual as produced by SiteRite™. Note the rather small internal jugular vein on the left (1A) compared to the very large internal jugular vein on the right (1B). | |
In particular, there is substantial variation in underlying vascular structures when compared to external landmarks. The portable ultrasound allows the practitioner to identify these anatomic variations prior to unintentionally sticking the carotid artery. We also have observed substantial variation in the size of the internal jugular vein from one side to another. It is not unusual for the internal jugular vein to be quite small on one side and to be huge on the contralateral side (Image 1A and B). This fact cannot be discovered without the use of the portable ultrasound. It is our opinion that the portable ultrasound should be used routinely in all elective central vascular access procedures even when performed by experienced anesthesiologists. This does not mean that we recommend the complete guidance process facilitating the vascular access; but merely that the practitioner at least “have a look” with the portable ultrasound device prior to the initial needle stick. We are aware of numerous midadventures related to central vascular access that probably could have been prevented by the use of a portable ultrasound. We are also aware of litigation related to central vascular access where substantial compensation was paid that may have been prevented or mitigated by the use of portable ultrasound. Experts for plaintiff will certainly point to the lack of use of this device (if it was not used) as a criticism of the practitioner in central vascular access malpractice cases. In our experience, puncture of the carotid artery is the most common complication of central vascular access when attempting internal jugular catheterization. Avoidance of carotid artery puncture is clearly facilitated by the use of portable ultrasound.
The variability in location of vascular structures relative to external landmarks becomes a compelling reason to utilize portable ultrasound. Unfortunately, at this time such technology may not be available in all healthcare facilities in the United States. Almost 30 years ago we published the first article describing access of the central circulation utilizing the external jugular vein in conjunction with the flexible angiographic wire catheter guide (J-wire).9 This is a technique that does not depend upon identification of underlying structures utilizing surface landmarks. While not as popular as either the subclavian or internal jugular approach for central vascular access, the external jugular vein can still serve as a valuable access route in situations where the portable ultrasound is not available.
Drs. Webster and Blitt are practice associates at Old Pueblo Anesthesia, Tucson, AZ, and have no financial relationship to any manufacturer of this technology. Dr. Blitt is also a member of the Executive Committee of the APSF.
References
- Committee on Quality Health Care in America. To err is human: building a safer healthcare system. Washington: National Academy Press, 2000.
- Rothschild JM. Ultrasound guidance of central vein catheterization. Evidence Report/Technology Assessment, No. 43. Chapter 21. Making Healthcare Safer. A Critical Analysis of Patient Safety Practices. Agency for Healthcare Research and Quality Publication, No. 01-E058. 2001;245-253. Available on the web at: http://www.ahrq.gov/clinic/ptsafety/.
- Troianso CA, et al. Internal jugular vein and carotid artery anatomic relation as determined by ultrasonography. Anesthesiology 1996;85:43-8.
- Forauer AR, et al. Importance of US findings in access planning during jugular vein hemodialysis catheter placement. J Vasc Interv Radiol 2000;11:233-8.
- Gordon AC, et al. US-guided puncture of the internal jugular vein: complications and anatomic considerations. J Vasc Interv Radiol 1998;9:333-8.
- Conz PA, et al. Cannulation of the internal jugular vein: comparison of the classic Seldinger technique and an ultrasound guided method. J Nephrol 1997;10:311-3.
- Shulman MS, et al. An anteromedial internal jugular vein successfully cannulated using the assistance of ultrasonography. J Clin Anesth 2000;12:83-6.
- Hatfield A, Bodenham A. Portable ultrasound for difficult central venous access. Br J Anaesth 1999;82:822-6. 9. Blitt CD, et al. Central venous catheterization via the external jugular vein. A technique employing the J-WIRE. JAMA 1974;229:817-8.

