The APSF Board of Directors Workshop on Saturday, October 24, 2015, in conjunction with the annual meeting of the American Society of Anesthesiologists, in San Diego, CA addressed the topic, From APSF Educational Videos to Your Practice: How to Make it Happen.

Dr. Jeffrey M. Feldman introduced the APSF operating room fire safety video and noted that obstacles to eliminating preventable fire injuries include (1) reflex use of 100% oxygen by open delivery (face mask, nasal prongs) during monitored anesthesia care and (2) reluctance to control the airway during minor procedures often leading to open delivery of oxygen. Education on sedation with low levels of supplemental oxygen (<30 %) or no supplemental oxygen is needed. Methods for blending oxygen to control the FIO2 may not be readily available, and one may need to consider non-invasive ventilation techniques such as BIPAP.
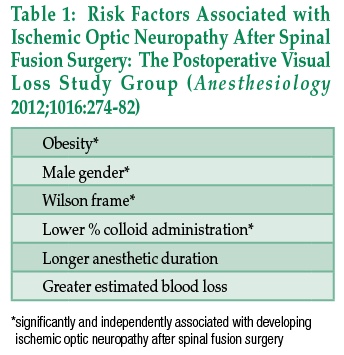
Dr. Lorri A. Lee introduced the APSF videos dealing with perioperative visual loss (POVL) and the companion video presenting various scenarios for obtaining informed consent for patients at risk for POVL. It is important to recognize that posterior ischemic optic neuropathy (PION) following spine surgery, unlike central retinal artery occlusion, is not caused by pressure on the globe. PION seems to be associated with venous congestion of the head (head down prone position). There is increasing acceptance that the informed consent process should include the risk of POVL in selected patients. However, the value of the informed consent to the patient is dependent on those responsible for the patient’s care to be cognizant of the evolving strategies designed to reduce the risk of POVL.
Dr. Feldman’s and Dr. Lee’s introductory comments set the stage for small group discussions to explore strategies to implement the content of the videos into best practices (Figure 1, Tables 1–2) and to share options to overcome barriers to implementation of the safety practices described in the videos.


APSF believes that educational videos provide advantages compared with the traditional written report when addressing anesthesia patient safety issues and advocating for “best practices” to reduce the likelihood of the adverse events described in the videos (Table 3).
The learning objectives of the workshop were
- Apply the content of the patient safety videos as a vehicle to implement best practices in the operating room.
- Recommend approaches to overcome implementation barriers to safety practices described in the videos.
- Understand strategies for utilizing videos for safety improvement
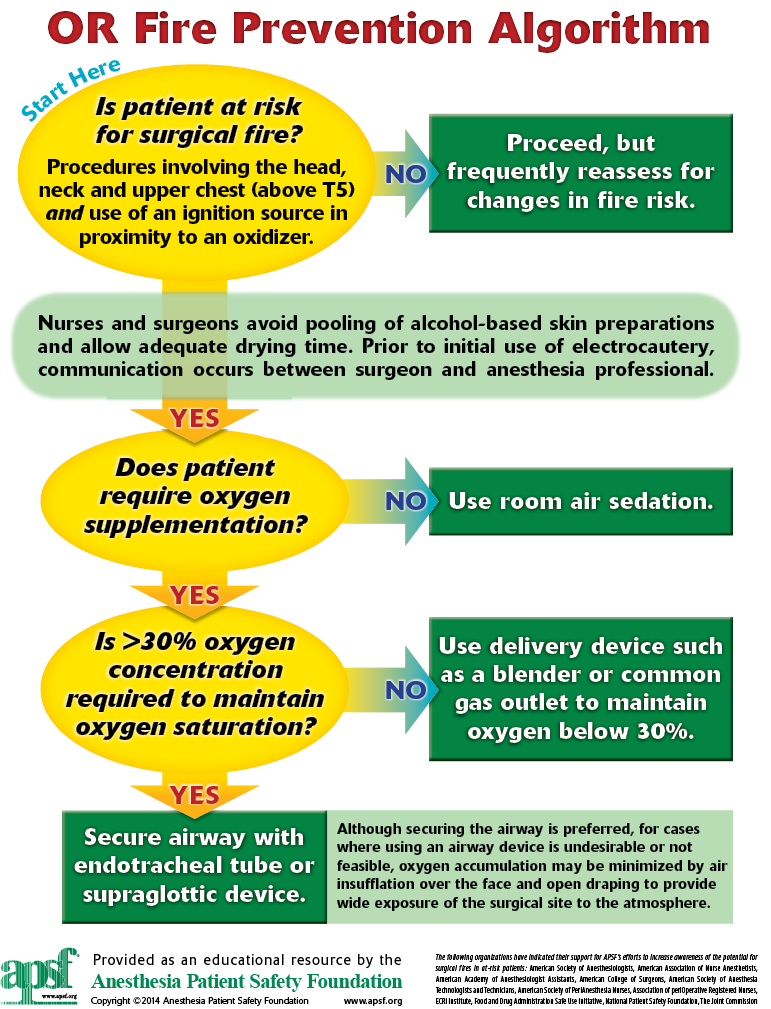
Prevention and Management of Operating Room Fires
https://www.apsf.org/resources/fire-safety
Despite the fact that we know which patients are at risk for fire (surgery above T5 and use of an ignition source in proximity to an oxygen enriched atmosphere) and understand how to prevent a fire (minimize the concentration of oxidizer [oxygen, nitrous oxide]), SURGICAL FIRES CONTINUE TO OCCUR. The root cause of serious fires is typically the use of supplemental oxygen via an open delivery system, thus creating an oxygen-enriched atmosphere in proximity to an ignition source. Anesthesia professionals have direct control over the concentration of oxygen and the method of administration.
Perioperative Visual Loss (POVL)
https://www.apsf.org/resources/povl/
Simulated Informed Consent Scenarios for Patients at Risk for Perioperative Visual Loss (POVL)
https://www.apsf.org/resources/povl-consent/
APSF believes that increased awareness and understanding of risk factors associated with postoperative visual loss (POVL) is a timely patient safety topic. Peer-review literature and data from the American Society of Anesthesiologists (ASA POVL Registry) are evolving in a manner that suggest a patient profile at risk for POVL and steps to take in the surgical and anesthetic management that might decrease the incidence of this devastating complication. There seems to be increasing acceptance that the informed consent for surgery and anesthesia should include the risk of POVL in selected patients. Yet the value of the informed consent to the patient is dependent on those responsible for their care to be cognizant of evolving information and strategies designed to reduce the risk of POVL.
Small Group Discussions
Comments and recommendations from the small group breakout sessions following presentation of the videos included
- An operating room fire was a personal experience of several of the attendees or they were aware of an operating room fire in their practice group. POVL was not a common experience among the attendees.
- The APSF recommendations for best practices for patients at risk for an operating room fire were supported by the attendees, but their acceptance sometimes was not instituted until after an adverse event had occurred.
- There was interest in adding a “time out for fire safety” to the electronic medical records.
- The need for technology (blenders) to titrate the delivered concentration of oxygen was emphasized.
- POVL was an uncommon experience, but the APSF recommendations for best practices in patients at risk for POVL were supported with the caveat that surgeons would likely be reluctant to endorse the need for inclusion of this complication in the informed consent. A personal relationship with the surgeon is important in gaining acceptance of inclusion in the informed consent as part of the at-risk patient’s care. There was agreement that the anesthesia professional should include POVL in the informed consent for at risk patients if the surgeon declined to do so.
- Education (including simulation) for all those caring for patients (especially nurses and surgeons) was viewed as critical for fire safety (understanding that 30% oxygen should be the maximum open delivery concentration) and POVL (recognition of risk factors and the informed consent process).


 Issue PDF
Issue PDF