To the Editor
Operating room (OR) fire is considered a sentinel event in today’s practice of medicine. Despite the safety guidelines that are currently in place at most hospitals, OR fires still occur anywhere from 50-200 times per year. Recent literature suggests that there is poor communication and preparedness of the OR staff for such events. Furthermore, the lack of accurate air-oxygen delivery systems has been cited as an additional problem.

Figure 1. Air-Oxygen blender mounted on the Datex Ohmeda anesthesia machine.
OR fires traditionally require 3 components, known as the “fire triad”: 1) an oxidizer, 2) an ignition source, and 3) fuel.1 Oxidizers, usually supplied by the anesthesia provider, include oxygen and nitrous oxide, and are especially hazardous when an oxidizer-enriched atmosphere exists within a closed or semi-closed system.
Ignition sources are usually the responsibility of the surgeon, and include electrosurgical or cautery devices, lasers, and heated probes.
Fuel sources are usually supplied by the nurse or scrub technician, and include sponges, drapes, alcohol-containing solutions, gowns, and a number of other flammable items.2 The ASA Practice Advisory on OR Fires states that prevention involves 3 components: 1) minimizing an oxidizer-enriched atmosphere near the surgical site, 2) managing ignition sources, and 3) managing fuels.3
The anesthesia provider has a pivotal role in OR fire prevention with regard to oxidizer supply. Current oxygen delivery systems allow for delivery of an inspired FiO2 of 0.24 to 0.90, depending on the oxygen flow rate, via systems such as simple or Venti-masks, non-rebreather face masks, or nasal cannulae.4 Since 2003 the Joint Commission on Accreditation of Healthcare Organizations (JC) has recommended the use of air or FiO2 <30% for open delivery systems to prevent surgical fires.5 The common auxiliary ball-in-tube O2 flowmeter mounted to most anesthesia machines delivers 100% O2, which, when used with the above delivery systems, is not ideal, according to the JC recommendations.
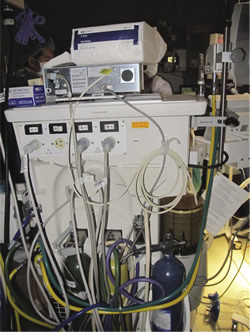
Figure 2. The back of the anesthesia machine, showing oxygen/air connections.
An air-oxygen blender (Precision Medical), can easily be mounted on most modern anesthesia machines via a universal mounting bracket and appropriate gas delivery hoses.6 The blender has a large control dial, which allows users to deliver a precise FiO2 between 21% and 100%, with a 3% error. Gas blends can safely be delivered to infant, pediatric, and adult patients. After being mounted and connected to oxygen and air lines, this device is also attached to a metering device and an oxygen analyzer. A bleed collar vents the air-oxygen mixture to the atmosphere to maintain FiO2 accuracy. Air-oxygen blenders offer a simple solution for anesthesia providers to control delivery of accurate oxygen concentrations, particularly at lower FiO2s. Such a solution allows for better prevention of OR fires and greater compliance with JC recommendations.
The authors have no financial conflicts of interest with Precision Medical or any other air-oxygen blender manufacturer.
O.I. Ahmed, MD, G. Sanchez, BA, K. McAllister, and PA, M. Girshin, MD, Department of Anesthesiology, Metropolitan Hospital Center, New York, NY.
References
- Practice advisory for the prevention and management of operating room fires. Anesthesiology. 108:5, 2008;786-801.
- Stuart RH, Yajnik A, Ashford J, Springer R, Harvey S. Operating room fire safety. The Ochsner Journal. 11:1, 2011;37-42.
- Daane SP, Toth BA. Fire in the operative room: principles and prevention. Plastic and reconstruction surgery. April 15, 2005:115: 73e-75e.
- Bateman NT, Leach RM. ABC of oxygen. Acute oxygen therapy. BMJ. 1998 Sep 19;317(7161):798-801.
- Lampotang S, Gravenstein N, Paulus DA, Granvenstein D. Reducing the incidence of surgical fires: supplying nasal cannulae with sub-100% O2 gas mixtures from anesthesia machines. Anesth Anal 2005;101:1407-12.
- Precision Medical. Air-oxygen service & user manuals. http://www.precisionmedical.com/hospitals/air-oxygen-blenders/blender.


 Issue PDF
Issue PDF