Editor’s Note: Dr. Cohen was a recipient of an APSF Research Grant for 1987. She reports here on a portion of her work.
Since mortality from anesthesia has decreased in recent years, nonfatal events have become much more important in assessing quality of care in anesthesia. Studies by Cooper (1978, 1984) looked at anesthetic “near mishaps” rather than at actual deaths or major complications. While extremely helpful, this approach cannot be used to determine the frequency of such occurrences.
Similarly, review of malpractice suits (e.g., Utting, 1979) have proven invaluable in defining deficiencies in anesthetic practices, but cannot be used to determine rates of adverse events. In addition to deaths and “major” complications, it is essential for patient comfort to determine the rate of “minor” anesthetic complications for example, nausea and vomiting, broken teeth, spinal headache and so forth as these are often an indication of poor anesthetic technique. Indeed, it is probably these ” nuisance’ complications that most often lead to patient dissatisfaction and contribute to medical-legal events.
Quality Assurance
According to a World Health Organization Working Group (I 985), there are several reasons to undertake a quality assurance program. The first stems from a desire for health professionals to be self-regulating to identify their deficiencies and thereby their areas for improvement. A second motive for quality assurance programs is the increasing requirement to be accountable to society for monies spent on health services and for safety to the public. In today’s climate of increased expectations, the public wants to be protected from harmful treatments but is also not content with inappropriate or suboptimal care. Thus quality assurance systems are needed to ensure social accountability. Last, the report suggests that quality assurance is necessary to design programs which identify problems and advance the performance of health care systems. The improvement of health care data will permit health planning to proceed based on a more adequate information base
There are three basic types of quality assurance studies those based on structure, process and outcome Donabedian (1980). In a review of the history and evolution of quality assessment programs in the U.S., Sanazaro (1980) pointed out the deficiencies of quality assessment programs based primarily on the structural and process approaches, and called for the development of methods of monitoring “the application of efficacious medical treatment and the attainment of outcomes that have been shown to be the direct results of that treatment”.
The most powerful evaluation of quality care is the outcome study. This evaluates the impact on care on the patients’ health status. Measures of outcome include mortality, morbidity, complication rates, infection rates and patient satisfaction (Lohr 1988). Outcome studies must have some means of controlling for patient “case-mix” such as age and sex adjustment. In a previous publication (Cohen & Duncan, 1988), we used the American Society of Anesthesiologists’ physical status score combined with age, sex and emergency status as case-mix variables.
Outcome Standards
In today’s medical-legal climate, there is a great need to develop outcome (quantitative) standards for anesthetic care. The Canadian Four Centre Study on Anesthetic Outcomes was designed to determine if a systematic system for surveillance of anesthetic outcomes could he developed, a system which could then be subsequently adopted for general use in most hospitals. The second goal of the study was to determine the rate of the more common adverse events attributable to anesthesia, given the advances in technology and therapeutics.
The basic program uses “occurrence screening”. This means that all (or almost all) patients undergoing anesthesia are captured by the Follow-up program. For each patient undergoing surgery, anesthesiologists fill out a check-off form which includes the preoperative physical status assessment, patient characteristics, anesthetic techniques and drugs used, anesthetic monitors, and any complications occurring during the operative procedure. Anesthetists are encouraged to use the check-off items in addition to, or as a replacement for, the usual documentation.
Following the operative procedure, recovery room nursing staff record any complications which occur during the immediate postoperative recovery period. Within 72 hours (usually 24-48), a designated anesthesia nurse reviews all anesthesia records and hospital charts. Inpatients are interviewed to determine “minor” complications. The nurse also checks hospital logs to determine if deaths have occurred among surgical patients. The nurse then returns the form to the anesthesiologist for a final review and for appropriate action to be taken if needed.
After inspection by the anesthesiologists, the form is then sent for computer entry (a personal computer is used with specially designed software). A monthly report outlining patient characteristics and complication rates is then generated. This information is reviewed by the Medical Audit Committee and prints out cases for review by the committee. Parallel programs are being run in the four hospitals.
Preliminary results from the study show that after some technical problems were overcome, it was possible to set up the program in four very different hospitals, each with their own modes of operation. Some of the technical problems which we dealt with were related to the anesthesia record, compliance of the anesthetists, and hiring appropriate nursing staff.
The design of the anesthesia record was accomplished after several months consultation with several groups of interested persons. These included the anesthesia staff, the administration officers, hospital forms committees and others. After development of a prototype, the form was piloted for six months. The record had to meet the needs of the anesthetists, had to be self-explanatory and easy to use and had to be of a certain size to fit into the hospital chart at each institution. The costs of the form also had to be considered since they were somewhat more expensive than the form they replaced.
Compliance of the anesthesia staff was less of a problem than had at first been anticipated once staff were familiar with the form, compliance improved. In two hospitals, the anesthetists’ billing form was part of the anesthesia record leading to improved compliance. lnservices and rounds helped to familiarize staff with the new records. Hiring of appropriate nursing staff and training took several months, but fortunately high quality personnel seemed to be attracted to these nursing positions.
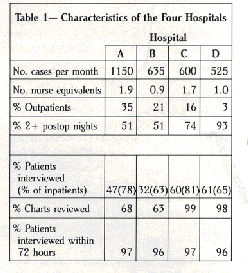
Table I presents the characteristics of the four hospitals. Hospital A performed the most cases per month and the number of cases was similar in the other three centers. Hospital A had the most outpatient surgery and consequently fewer inpatients who were available to be interviewed. Outpatient charts were not accessible for review in hospitals A and B. For those patients interviewed, approximately 96 to 97% were seen within 72 hours (the time period when the majority of anesthesia-related events would occur).
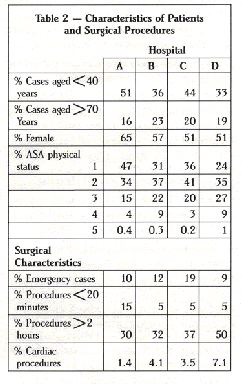
The majority of cases at hospital A were under 41 years of age and were female (Table 2). Hospital B performed the most surgical procedures among the elderly. With regard to physical status, 47% of the cases at hospital A were rated as ” I ” (normal healthy) and hospital D had the sickest patients (10% who were ASA 4 or 5). Approximately 10% of the cases were emergency and at hospitals B, C, and D, 5% of the cases were less than 20 minutes in duration. Conversely, hospital D had 50% of its cases which were two hours or more. Hospital D also performed the most cardiac surgery (7. 1 % of cases).
Aimed at Rare Events
Thus, we are using occurrence screening to carry out an outcome study at four hospitals across Canada. While occurrence screening is probably preferable to study rare events, it may not be possible for all types of hospitals to use such an approach. The resources implicated in this type of follow-up program are not high, but still represent an investment in time and money. Approximately one full time nurse (preferably two half time nurses) are needed for follow-up. While we use data entry (and require a half-time data entry operator), possibly machine readable forms might be available in the future The forms themselves are expensive and represent an investment of resources. Finally a personal computer and someone who can operate it are needed.
The information from the follow-up prognosis can be utilized in several ways. First the individual hospital department of anesthesia could use the data to compare its performance on a monthly or quarterly basis tot hat of its performance (with regard to complication rates or resources used) in the past. Second, the system would identify any unusual patterns of complications which would alert the department to perform an investigation and either remedy the problem or institute measures to prevent the problem from recurring. Third the information ran identify cases of anesthetic related conditions which should be reviewed by the Medical Audit committee in addition to operative deaths (which tend to be the only cases reviewed by most of these committees). Last, the individual performance of any staff member could be compare-d to that of his/her peers (after adjustment for case-mix).
Our study will also help to determine if it is necessary to carry out interviews with ward patients as well as chart reviews and whether phoning day surgical patients is needed. Finally, a hospital may want to consider some combination of follow-up program with the department of surgery. If that is the case, then the optimal time for seeing patients for follow-up wig need to be determined.
Will the presence of a quality assurance program make any difference, either to patient-related morbidity or to medical-legal proceedings? Them is little doubt that documentation of success elicits pride in one’s performance-, and spurs one to improve his/her attributable outcomes. However, it is not yet known if anesthetic-related complications have a minimum rate beyond which further improvements are unlikely. However, there is no evidence to date that we have achieved the ultimate standard of excellence and only sequential quality assurance surveys will confirm when that day arrives.
References
Cohen MM, Duncan PG. Physical status score and trends in anesthetic complications. I Clin Epidemiol 1988;41:83-90.
Cooper IB, Newbower RS, Long CD, McPeek B. Preventable anesthesia mishaps: a study of human factors. Anesthesiology 1978; 49:399AO6.
Cooper IB, Newbower RS, Kitz RI. An analysis of major errors and equipment failures in anesthesia: considerations for prevention and detection. Anesthesiology 1984;60:3842.
Donabedian A. The definition of quality and approaches to its assessment. Ann Arbor, MI, Health Administration, 1980.
Lohr KN. Outcome measurement: concepts and questions. Inquiry 1988;25:37-50.
Sanazaro PI. Quality assessment and quality assurance in medical care. Ann Rev Public Health 1980;1:37-68.
Utting JE, Gray TC, Shelly FC. Human misadventure in anesthesia. Can Anaesth Soc 1 1979;26:472-78.
WHO Working Group in the Principles of Quality Assurance. ‘Me principles of quality assurance. Copenhagen, World Health Organization, 1985.

