
A video intubating scope used as a difficult airway teaching tool is demonstrated in the ASA Scientific Exhibits by Dr. Denham Ward of the University of Rochester.
Patient safety occupied its usual position of prominence in the Scientific Papers Sessions presented at the American Society of Anesthesiologists Annual Meeting in San Francisco in October when 76 presentations were given in four separate sessions. Full text of all abstracts from the meeting is available online at www.asa-abstracts.com.
The potential impact on renal function of inhalation anesthetics, carbon dioxide absorbers, and the combination of the two had its own poster-discussion session. A group from Germany studying patients with preexisting renal impairment found no adverse effects from sevoflurane low-flow anesthesia. Likewise, a University of Washington group saw no adverse impact of extended exposure to sevoflurane. While Austrian and Japanese groups presented the issue in general, the Compound A production from CO2 absorber exposed to low-flow sevoflurane was shown by another German group to vary significantly and a new brand advertised as being less liable to this problem did produce less of the toxic substance. Yet a third German group showed dramatic reduction in Compound A when LiOH was substituted in absorber for NaOH and KOH.
Compromise of both ventilation and oxygenation uniquely in morbidly obese patients undergoing gastric banding via laparoscopy rather than open laparotomy was demonstrated by a group from Hamburg, Germany, and the results were offered as a safety warning regarding patients anesthetized for this particular type of surgery. A comparison of bronchodilation effects on the inhalation anesthetics desflurane and sevoflurane following intubation revealed the expected bronchodilation with sevo but not with des and, in fact, airway resistance actually increased with desflurane, especially in patients who smoked.

Award-Winning Exhibit: The APSF’s E.C. Pierce Award for the best scientific exhibit at the ASA Meeting related to patient safety for 2000 went to a team from the University of Pittsburgh for the exhibit “Simulation Based Training in Applying the ASA Difficult Airway Algorithm.” Shown here at the award presentation are (L to R) exhibitors Drs. René Gonzalez and Randolph Wood, Dr. E.C. Pierce, Jr. (APSF Executive Director), lead exhibitor Dr. John Shaefer III, and Dr. Robert Stoelting (APSF President).
Airway management, as always, was the subject of several papers. The intubating laryngeal mask airway was demonstrated as efficacious in obstructive sleep apnea patients by a group from France and a German team showed its utility in model resuscitation situations. A paper by Dr. S. Lussos and associates noted that an automated electronic anesthesia record-based data base revealed 3.5 times as many patients who demonstrated true inability to intubate than were voluntarily reported by the anesthesia providers involved, suggesting that attempts to identify and warn such patients (including with Medic Alert bracelets) need more attention. In the study, there were 41 “true inability to intubate” patients out of 16,794 or 2.4/1000 cases. Comparing efficacy of routes of fiberoptic intubation was done by Dr. P. Szmuk and associates from the University of Texas, Houston, who found that nasal fiberoptic approach with a cuffed oropharyngeal airway in place was 100% successful vs. only 50% for the straight oral approach in anesthetized spontaneously breathing patients.
A study originally initiated through an APSF research grant to Dr. R. Morell of Wake Forest University demonstrated that males were more susceptible than females to ulnar nerve ischemia during the application of a tourniquet. This effort continues that groups ongoing investigation into the mechanism of peripheral nerve injury. A related effort from a group from the Mayo Clinic with similar interests revealed that the lithotomy position itself—but not the externally applied anti-DVT pneumatic stockings—causes increased intracompartment pressure in the legs.
Research into the differences between the two available formulations of propofol was conducted by a British team from Nottingham. This question was featured prominently last year in several issues of the APSF Newsletter. Results offered were: “Propofol Emulsion was significantly less stable than Diprivan after shaking and freezing, possibly due to the differences in pH and additives.”
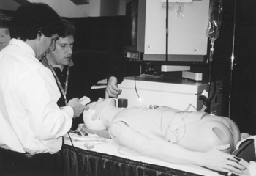
Dr. Gonzalez demonstrated points of the ASA Difficult Airway Algorithm to an exhibit attendee on the simulator and the adjacent fiberoptic scope and monitor.
A much-discussed study from a team at the University of Washington headed by Dr. M. Uppal presented 21 cases of postoperative blindness reported to the Postoperative Visual Loss Registry, all but one due to ischemic optic neuropathy. 12 cases involved extensive spine surgery in the prone position and 6 cases were open-heart surgery. Research into potential mechanisms continues. Expected admonitions about maintaining normal arterial pressure and hemoglobin levels were made but the paper concluded, “Prevention and treatment strategies remain elusive.”
A Japanese team from Osaka studied the predictive value of a diagonal crease in the earlobe of patients over 40 for coronary artery disease. The sign was 93% sensitive and 82% specific with an overall predictive value of approximately 40%. The authors suggest examination for this sign in patients coming for emergency surgery.
The safety and efficacy of sedation of pediatric patients for procedures outside the OR using videotaped reviews of actual procedures was studied by a Dartmouth group. A graphic scoring system based on pain/stress, movement, level of consciousness, and side effects (such as decrease in Hb saturation) was created and tracked. Wide variations in results were seen and a significant resulting QA effort has improved care already.
The relationship of case length and ASA status to adverse anesthetic events was presented in two papers from Montefiore Medical Center in New York. Over 54,200 cases were studied. “Human errors” were rare but 2.3 times more likely in cases more than 3 hours long and “system errors” were more common as ASA PS increased. The two were not found synergistic. Even though the ASA PS was not intended for risk prediction, the incidence of adverse outcomes (622 total) associated with human error did correlate highly with increasing ASA PS classification, the predictive value of which regarding rate and severity of adverse patient outcome was noted. A similar type of investigation from Switzerland found correlation of long term outcome for patients undergoing hepatic resection with preoperative ASA PS.
Inadequate preoperative evaluation of patients with pacemakers occurred 51% of the time, as seen by a team from the University of Florida. In 19% of cases, the pacer was accidentally altered and perioperative problems related to the pacer were seen in 13% of cases. The most often cited causative factor was incorrect placement of the electrocautery “ground” (return) plate.
A provocative study by Dr. J. Thompson of Mt. Sinai in New York examined the relation of relapse rate among 10 IV substance abusing anesthesiologists to the time spent in rehab prior to return to clinical anesthesia practice. Five addicts returning within six months all relapsed compared to none of the five who were in rehab 12 months or more before returning to practice. Even these small numbers were considered dramatic and further investigation was called for. No specific patient safety implications were raised in the paper in spite of the fact that this issue is always present with any discussion of substance-abusing anesthesiologists.

