State Society Focuses on Needed Changes
Recognizing the need for personal involvement by individual anesthesiologists, the North Carolina Society of Anesthesiologists (NCSA) organized its 1986 annual meeting in Asheville to focus on a comprehensive strategy to link safety in anesthesia with a plan to implement risk management.
Speakers included Burton A. Dole, Jr., Chairman and President, Puritan-Bennett Corporation, John H. Eichhorn, M.D., Harvard Medical School, Boston; Ellison C (Jeep) Pierce, Jr., M.D., President, Anesthesia Patient Safety Foundation, New England Deaconess Hospital, Boston; William D. Petasnick, Director of Operation, North Carolina Memorial Hospital, Chapel HUI; Robert W. Vaughan, M.D., Professor and Chairman, Department of Anesthesiology, University of North Carolina at Chapel Hill; and Mark D. Wood, Medical Services Manager of Risk Management Division, St. Paul Fire & Marine Insurance Company.
Moderators from the NCSA were Drs. Jerry Calkins and Dana Hershey (President). In organizing this seminar, NCSA leadership in private practice and academics recognized that the current crisis in the cost of medical liability insurance mandates that attention be directed toward risk management and patient safety to reduce the number and severity of anesthesia-related mishaps, For example, although the percentage of anesthesia medical liability claims involves only three or four percent of the total for all of medicine, the indemnity paid out exceeds I 11%. This underlines the importance of severity in the anesthesia cases and the absolute need to reduce risk, especially for hypoxia. Strategy should include combining facts, time, and effort directed at a safety program while working toward the more lengthy process of tort reform.
The program was structured for the first day to define the problems of risk management and liability and on the second day to propose solutions to the problems from different perspectives (i.e., the national and state level, the insurance industry, the manufacturers’ viewpoint, the hospital administrators’ overview, and a comprehensive strategy for linking a focus on patient safety, risk management, and malpractice reform).
Dr. Eichhorn opened the seminar by enumerating the enormous settlements and judgments presently drawing attention in the news media. He noted that anesthesiologists in their practice were more likely to be involved with severe, debilitating injuries than most other physician specialists; that possibly up to 2,000 ASA I patients die per year in the United States; and that a significant number of these deaths from available data appear to be preventable. In reviews of closed and open anesthesia-related claim abstracts, he enumerated that certain types of problems recur while variations in classification make comparisons difficult. These common complications include inadequate ventilation, difficult endotracheal intubation, esophageal intubation, accidental extubation, ventilator disconnects, bronchospasm, and relative or absolute anesthesia overdosase. However, anesthesiology is uniquely fortunate in that early detection of mishaps through use of newer sophisticated monitoring and technological advances is likely more possible than in any other specialty. Moreover, if one were to compare the purchase cost of monitoring devices with the skyrocketing cost of medical liability insurance, the capital outlay for monitoring equipment becomes small indeed. Dr. Eichhorn summarized his opinion regarding the solutions to the malpractice crisis as follows: tort reform extremely unlikely; insurance reform extraordinarily unlikely; system reform essentially impossible; and reduction of patient injuries the only hope. Our job as anesthesiologists seems clear.
Insurance View
Mr. Wood then presented the perspective from the insurance industry by explaining that insurance indemnity functions as a system of risk sharing where the financial resources of the group are made available to pay for the losses of individual members. The biggest problem in insuring the anesthesiologist is the fact that when the losses do occur, they frequently are catastrophic in nature.
For example, preliminary dosed-claims data demonstrate that 22% of cases were hypoxia related, those cases consumed 57.2% of the indemnity, the per case cost was $403,500, and that, alarmingly, 80% of cases were ASA I and If patients. He emphasized that the solution for any anesthesiologist becomes an unwavering resolve to improve the efficacy of anesthetic techniques and to make the best use of available technology for early diagnosis and treatment of hypoxemia and reduction of iatrogenic injury to patients due to anesthetic administration.
Industry Perspective
Mr. Dole explained the viewpoint of the anesthesia equipment industry on safety and risk management. Noting that users and manufacturers of health care equipment are merely different a= of the same effort, he outlined the status of Puritan Bennett (P-B) as a leader in critical health care research and manufacturing. However, despite P-B products’ excellent safety record and despite modest liability claims and settlements, product liability insurance cost rose 656% in 1986. Their cost per $ 1,000 of insurance coverage increased 2700% for the same period while three of their primary insurance carriers become insolvent.
The tort system in 1986 is broken, expensive, inefficient, slow, and wasteful. As a result, industry is being forced to raise prices at a time when the national priority is to control costs and reduce health care expenditures. Consequently, an overwhelming demand has occurred for new legislation in order to guarantee a more reliable and predictable method of assessing damages and fault. As a plan for action, he noted that in the voluntary sector, representatives of the Health Industry Manufacturers Association are meeting with their counterparts at the American Medical Association in an effort to present a more unified front in the health care field to gain much needed tort reform in liability coverage. In much of the business and industry of health care, new research and development monies are being channeled towards patient safety and reduced labor costs. As the home health care market expands, rapidly increased attention is being given to the safe use of such products and the associated potential of liability risk. Mr. Dole closed by emphasizing that a major step forward has been taken with the establishment of the Anesthesia Patient Safety Foundation to focus specific resources of personnel and funds on an educational program for anesthesiologists. This unique effort is targeted to develop grassroots interest in patient safety and risk management. He noted that we need to change public perception. “We are doing a good job. Why are we on the defensive rather than the offensive?”

Hospital Position
Mr. Petasnick discussed the malpractice reform issue from the standpoint of hospital administration. “This is a team effort a partnership!” He noted the shared responsibility of the hospital and anesthesiologists to ensure a safe environment, the cost effectiveness of risk avoidance, and realistic strategies to work out a collaborative relationship between hospital administration and the medical staff. Mr. Petasnick’s experience has been that in many operating rooms in hospitals in North Carolina, anesthesiologists have begun to expect automated, non-invasive blood pressure apparatus; pulse oximeters; and even end-tidal PCO2 devices in addition to the already present electrocardiogram, oxygen analyzer, high and low pressure alarm, and temperature monitoring capabilities. He noted in his own institution how he had heard frequently from anesthesiologists emphasizing safety and risk management. Moreover, surgeons were beginning to recognize the early warning signal of the oximeter registering desaturation at unexpected moments as well as during endotracheal intubation. Pulse oximeters are even proceeding into the recovery room to aid in patient management and safety. There seemed no doubt that many large liability awards for hypoxic accidents could have been prevented by the provision of better monitoring equipment for the anesthesiologists. He further emphasized that with the constraint on the hospital capital equipment budget, an honest and realistic assessment rather than a “wish 6t” would demonstrate integrity and promote relationships necessary to help negotiation among health care colleagues. He applauded anesthesiologists for taking the lead in managing risk and being the first to emphasize patient safety. Mr. Petasnick closed by asking anesthesiologist leaders to approach their hospital administrator with a comprehensive three- to-five year plan including full disclosure of initial cost and maintenance, personnel (upgraded if necessary) needed for the new technology, a prioritized list of needs, and to maintain an ongoing dialogue using the candor necessary to build trust and understanding.
APSF Role
Dr. Pierce shared with the audience the genesis of the Anesthesia Patient Safety Foundation. In October, 1984, the first meeting of the International Symposium on Preventable Anesthesia Morbidity and Mortality was held in Boston under the auspices of the Royal Society of Medicine Foundation and the Harvard Medical School. Following this successful international meeting of invited experts, symposium members considered the future direction should include establishment of a safety foundation. Subsequently, the 1985 House of Delegates of the American Society of Anesthesiology embraced Dr. Pierces proposal for a safety foundation. The Anesthesia Patient Safety Foundation was established as an independent organization with 50% of its board of directors as ASA members and an administrative support office at the ASA headquarters in Park Ridge, Illinois. The 30-person board of directors has been constituted to include 15 anesthesiologists, as well as representatives from equipment manufacturers, CRNA anesthesia, the insurance industry, the legal profession, the American Hospital Association, and the Federal Food & Drug Administration. The mission established was “to insure that no patient shall be harmed by the effects of anesthesia.”
Dr. Pierce has gone on record by stating that “today it is simply unacceptable to allow cost containment and inertia to prevent utilization of state-of-the-art anesthesia and monitoring apparatus. No government official or hospital administrator would ever fly in an airplane without up-to-date equipment and safety devices.” The only difference Dr. Pierce stated in the deaths that he can see is that “anesthesia deaths occur one at a time, whereas in the airline industry they occur in large numbers at once”.
Revolution and Crisis
Dr. Vaughan was asked to give an overview of the health care revolution in which we find ourselves, the liability crisis, and reflect on how our health care colleagues can become allies in the battle. He noted that our U.S. health care revolution includes tremendous cost (over 460 billion dollars spent in 1986 on U.S. health care); population demographics with aging and increased health needs and costs for Medicare and Veterans Administration recipients (Table 1); a huge budget deficit developed over that last six years (greater than one trillion dollars) introducing the severe political crisis in how to control costs; the enormous technology changes that seem almost beyond our ability to afford; and the ethical and moral dilemma presented to physicians to decide who lives, who dies, and who gets how much of what cam The liability coverage issue has become one of unavailable insurance coverage for small business and high risk providers as well as affordability for high risk providers especially with capitated reimbursement schemes (i.e., Massachusetts).

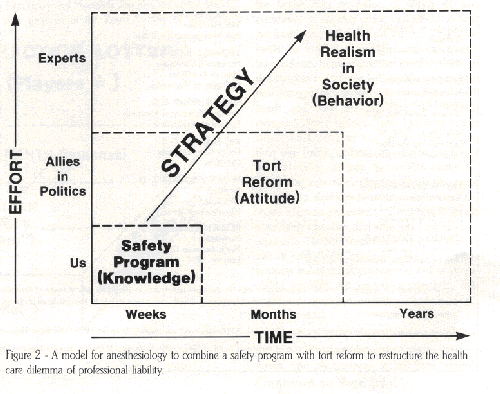
Despite U.S. health cares success in becoming a miracle, an exportable resource, the envy of the world, and phenomenal, it has been severely criticized as inefficient, wasteful, subject to abuse and responsible for collosal costs in an emerging “medical arms race7′ for lithos (helicopters), lithos (lithotripters), and nucleos (MRI’s). Dr. Vaughan summarized the “malpractice lottery” as involving four players (Figure 1). The loser on all accounts becomes American society with maldistribution of minimal benefits for the exorbitant cost of settlements. The present system appears out of control. For example, while $.30 of each malpractice dollar goes to the victim of malpractice, $.70 goes to overhead expenses to reimburse lawyers, court costs, and expert witnesses. Dr. Vaughan suggested a plan which would start with the individual anesthesiologist, having each emphasize a program of saw and risk management by focusing on better monitoring and standards for each of our practices (Figure 2). An ongoing participatory dialogue would address the tort reform issue over time enlisting the assistance of our health care allies in an all out effort to eliminate the malpractice lottery and distribute appropriate compensation to injured patients and family.
Finally, all speakers agreed that anesthesiology was a specialty uniquely positioned to control its fate in terms of risk management. The members of the North Carolina Society of Anesthesiologists agreed in subsequent discussions that the tort system was indeed broken, wasteful, inefficient and unfair, and quite slow (three to five years) to settle claims. North Carolina anesthesiologists are attempting through their practices to demonstrate commitment to the principles enumerated by the Anesthesia Patient Safety Foundation while continuing to speak actively to government and employers as patient advocates in health care.
Dr. Vaughan is Professor and Chairman, Department of anesthesiology, University of North Carolina at Chapel Hill.