Letter to the Editor:
To the Editor

Fig 1: Protective Device
Malpractice claims for acute postoperative blindness following spine surgery in the prone position are rapidly and greatly increasing1. Sixty-five percent of the reported cases of acute postoperative posterior segment blindness are due to central and branch retinal artery occlusion (RAO), and anterior and posterior ischemic optic neuropathy (ION)2. Greatly increased intraoccular pressures due to malpositioning of the face and eyes in the prone position appear to have the potential to be a primary causative factor in central and branch RAO and anterior and posterior ION induced blindness2. In addition, malpositioning of the face in the prone position can cause skin sloughing and facial nerve injury. Consequently, the standard of care requires “good documentation of periodic checks of the patient’s face… to prove that every attempt was made to avoid elevating intraoccular pressure.”1 Two aspects of currently used support devices strongly contribute to the likelihood that excess pressure will be applied to the eyes. First, the available devices do not easily or properly mate with the wide variety of head and facial shapes and sizes that exist, and thus can create areas of high pressure over sensitive structures. For example, a low nasal bridge in patients of Asian descent is thought to facilitate transmission of pressure to the eyes in the prone position2. Second, these devices do not allow the anesthesia care provider to easily and accurately check pressure sensitive structures, especially the eyes, once the patient is placed in the prone position.
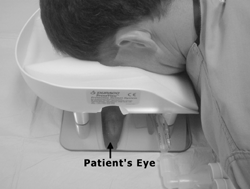
Fig 2: Protective Device demonstrated
To overcome these problems, the ProneView™ Helmet and Protection System was developed by Dupaco, Inc. The system consists of a rigid helmet, soft foam insert, and mirror (Figure 1). The foam insert is contoured to fit comfortably over the face while allowing expansive space to prevent contact with the eyes, nose and mouth. When the foam insert is mated to the helmet and used on a patient in the prone position, pressure is widely dispersed over the entire anterior portion of the skull superior to the anterior orbital rim, over the zygomas, and over the mandible, while no pressure is placed on the eyes, nose, or mouth. When attached to the mirror, the ProneView system permits easy viewing of the eyes from a position above the patient by simply looking at the mirror. The view of the face and eyes can be obtained even if drapes are placed over the patient’s head (as in posterior neck or cervical surgery) by using a flashlight to illuminate the facial structures beneath the drapes.
The ProneView™ system is applied by placing the foam insert into the helmet, and then placing the mated system onto the patient’s face after induction of anesthesia and insertion of the endotracheal tube. The endotracheal tube and pilot balloon are threaded through the mouth opening of the foam, and then directed either left or right into the slots located in the inferior portion of the helmet. The foam is adjusted to make certain that the anterior orbital ridge is exposed, that the foam lying over the zygomas falls below the inferior orbital ridge, and that the endotracheal tube exits the helmet without kinking. If an esophageal temperature probe, or oro/naso-gastric tube is present, these are similarly adjusted to make sure they exit without touching any facial structure. To place the patient in the prone position, the helmet is held using anterior pressure with one hand, while the other hand creates pressure in the opposite direction by supporting the occiput. The endotracheal tube is disconnected, the patient is rolled onto the OR table, and the legs of the helmet are placed on top of the mirror. After reconnecting the endotracheal tube and assuring adequate ventilation, the facial structures are re-examined by direct vision through the mirror to make sure that the foam did not shift upon the face during rollover. Once this proper position is confirmed, the neck is examined to make sure it lies in a neutral position. If necessary, the head is elevated or lowered using towels underneath the mirror or dropping the head section of the OR table, respectively.
Maximum safe surface pressures for facial structures have not been determined. Mattress manufacturers aim to keep maximum surface pressures below 30 mmHg (i.e., the upper limits of capillary blood pressure) to prevent decubitus formation. Using a standard Talley Oxford Pressure monitor, interface pressure measurements were taken on the forehead immediately above the superior orbital rim, on the cheeks, and on the chin in three adult subjects (Table I). Averages for three determinations for each subject, as well as the group averages for each site, are given in Table II. These pressures are significantly below the level considered safe for mattress support systems.
We have used the ProneView system in 56 adult patients, ranging in size from 38 Kg to 130 Kg, receiving general anesthesia while undergoing surgery in the prone position on a variety of OR tables. In all cases, the ease of examination of the facial structures made monitoring of potential pressure injury sites a simple and quick task. There have been no incidences of skin sloughing or eye injury in this group.
Table I: Gender, height, and weight of 3 subjects
Gender Height Weight
Subject 1 male 5’6″ 75 Kg
Subject 2 male 5’10″ 84 Kg
Subject 3 male 6’1″ 95 Kg
Table II: Facial pressure measurements
Transducer Location Pressure
Subject 1
forehead 25.1 mmHg
cheeks 34.0 mmHg
chin 24.1 mmHg
Subject 2
forehead 25.2 mmHg
cheeks 17.8 mmHg
chin 25.3 mmHg
Subject 3
forehead 27.6 mmHg
cheeks 15.6 mmHg
chin 24.0 mmHg
Group
forehead 26.0 mmHg
cheeks 22.4 mmHg
chin 24.5 mmHg
William J. Mazzei, MD
Clinical Professor of Anesthesiology
Jonathan L. Benumof, MD
Professor of Anesthesiology
University of California, San Diego
References
1. Lofsky AS, Gorney M. Induced hypotension tied to possible vision impairments. Anesthesia Patient Safety Foundation Newsletter, 1998;13 (2, Summer):16-17.
2. Roth S, Gillesberg I. Injuries to the visual system and other sense organs. In: Benumof JL, and Saidman JS (eds.) Anesthesia and Perioperative Complications, Second Edition. Philadelphia: Mosby,1999, 377-408.

